Percutaneous transhepatic cholangiography
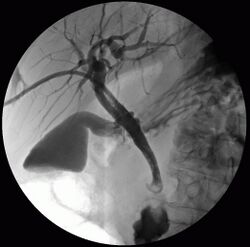
Percutaneous transhepatic cholangiography (PTC) is a medical procedure used to visualize the biliary tree and diagnose obstructions or other abnormalities in the bile ducts. This procedure involves the insertion of a needle through the skin and liver tissue into the bile ducts, followed by the injection of a contrast dye to make the bile ducts visible on X-ray imaging.
Indications[edit]
PTC is typically indicated in patients with jaundice, unexplained abdominal pain, or suspected biliary obstruction. It is also used to evaluate the anatomy of the bile ducts before surgery or endoscopic retrograde cholangiopancreatography (ERCP).
Procedure[edit]
The procedure is usually performed under local anesthesia and may be guided by ultrasound or fluoroscopy. The steps involved in PTC include:
- The patient is positioned, and the skin over the liver is cleaned and sterilized.
- Local anesthesia is administered to numb the area.
- A thin needle is inserted through the skin and liver tissue into a bile duct.
- Contrast dye is injected through the needle to outline the bile ducts on X-ray images.
- X-ray images are taken to visualize the bile ducts and identify any obstructions or abnormalities.
Complications[edit]
While PTC is generally safe, it carries some risks, including:
Alternatives[edit]
Alternatives to PTC include endoscopic retrograde cholangiopancreatography (ERCP) and magnetic resonance cholangiopancreatography (MRCP). These methods may be preferred depending on the patient's condition and the specific clinical scenario.
See also[edit]
- Biliary tree
- Endoscopic retrograde cholangiopancreatography
- Magnetic resonance cholangiopancreatography
- Jaundice
- Abdominal pain
References[edit]
External links[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian