Central retinal vein
Central retinal vein occlusion (CRVO) is a condition affecting the eye that can lead to significant visual impairment. It occurs when the central retinal vein, responsible for draining blood from the retina, becomes blocked or occluded. This blockage can lead to an accumulation of blood and fluid in the retina, causing damage to retinal cells and potentially leading to loss of vision.
Etiology[edit]
The causes of CRVO can be broadly categorized into systemic and ocular factors. Systemic factors include conditions that affect the body's vascular system, such as hypertension, diabetes mellitus, and hypercoagulability disorders. Ocular factors may include glaucoma, which increases the pressure inside the eye, thereby compressing the central retinal vein and leading to occlusion.
Pathophysiology[edit]
The blockage of the central retinal vein leads to an increase in venous pressure, resulting in retinal hemorrhages, edema (swelling), and ischemia (lack of oxygen). This can cause the retina to malfunction, leading to symptoms such as blurred vision or sudden vision loss in the affected eye. Over time, persistent ischemia may lead to neovascularization, where new, fragile blood vessels form on the retina or the iris, potentially leading to further complications such as neovascular glaucoma.
Symptoms[edit]
Patients with CRVO may experience a range of symptoms, including sudden, painless vision loss in one eye, blurred vision, or floaters. The severity of symptoms often depends on the extent of the occlusion and whether it is classified as ischemic or non-ischemic. Ischemic CRVO, which involves more significant blockage and retinal damage, tends to have more severe symptoms and a poorer prognosis.
Diagnosis[edit]
Diagnosis of CRVO involves a comprehensive eye examination, including visual acuity tests, a dilated fundus examination to inspect the retina, and imaging studies such as fluorescein angiography and optical coherence tomography (OCT). These imaging studies help assess the extent of the blockage and the associated retinal damage.
Treatment[edit]
Treatment for CRVO aims to manage the underlying cause and to address the complications arising from the condition. Management may include controlling systemic conditions such as hypertension and diabetes, as well as treatments to reduce retinal swelling and prevent neovascularization. Intravitreal injections of anti-VEGF (vascular endothelial growth factor) agents or corticosteroids are commonly used to treat macular edema and inhibit neovascularization. Laser therapy may also be employed in certain cases to reduce edema or to treat neovascularization.
Prognosis[edit]
The prognosis for patients with CRVO varies widely and depends on several factors, including the severity of the occlusion, the presence of ischemia, and the development of complications such as neovascular glaucoma. While some patients may experience partial recovery of vision, others may suffer from significant and permanent vision loss.
Prevention[edit]
Prevention of CRVO primarily involves the management of systemic risk factors. Regular medical check-ups to control conditions such as hypertension, diabetes, and hyperlipidemia can reduce the risk of vascular occlusions in the eye. Additionally, maintaining a healthy lifestyle with regular exercise and a balanced diet can contribute to overall vascular health and potentially prevent CRVO.
-
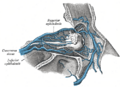
Diagram of the blood vessels of the eye
-
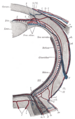
Central retinal vein and its branches
-
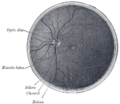
Anatomy of the eye showing the central retinal vein
-
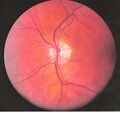
Central retinal vein
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian