Biotin-thiamine-responsive basal ganglia disease

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Biotin-thiamine-responsive basal ganglia disease | |
|---|---|
| |
| Synonyms | BTBGD, SLC19A3 deficiency |
| Pronounce | N/A |
| Specialty | Neurology, Genetics |
| Symptoms | Seizures, ataxia, dystonia, encephalopathy |
| Complications | N/A |
| Onset | Childhood |
| Duration | Chronic |
| Types | N/A |
| Causes | Mutations in the SLC19A3 gene |
| Risks | Family history of the condition |
| Diagnosis | Genetic testing, MRI |
| Differential diagnosis | Leigh syndrome, Wilson's disease, Mitochondrial disorders |
| Prevention | N/A |
| Treatment | Biotin and thiamine supplementation |
| Medication | N/A |
| Prognosis | Variable, can be improved with early treatment |
| Frequency | Rare |
| Deaths | N/A |
Other Names: Biotin-responsive basal ganglia disease; BBGD
Biotin-thiamine-responsive basal ganglia disease is a disorder that affects the nervous system, including a group of structures in the brain called the basal ganglia, which help control movement.
Epidemiology[edit]
Biotin-thiamine-responsive basal ganglia disease is a rare disorder; its prevalence is unknown. Approximately 48 cases have been reported in the medical literature; most of these are individuals from Arab populations.
Cause[edit]
Biotin-thiamine-responsive basal ganglia disease is caused by mutations in the SLC19A3 gene. This gene provides instructions for making a protein called a thiamine transporter, which moves thiamine into cells. Thiamine, also known as vitamin B1, is obtained from the diet and is necessary for proper functioning of the nervous system. Mutations in the SLC19A3 gene likely result in a protein with impaired ability to transport thiamine into cells, resulting in decreased absorption of the vitamin and leading to neurological dysfunction. In this disorder, abnormalities affect several parts of the brain. Using medical imaging, generalized swelling as well as specific areas of damage (lesions) in the brain can often be seen, including in the basal ganglia. The relationship between these specific brain abnormalities and the abnormal thiamine transporter is unknown. It is unclear how biotin is related to this disorder. Some researchers suggest that the excess biotin given along with thiamine as treatment for the disorder may increase the amount of thiamine transporter that is produced, partially compensating for the impaired efficiency of the abnormal protein. Others propose that biotin transporter proteins may interact with thiamine transporters in such a way that biotin levels influence the course of the disease.
Inheritance[edit]
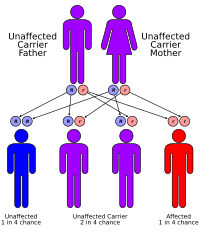
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Signs and symptoms[edit]
The signs and symptoms of biotin-thiamine-responsive basal ganglia disease usually begin between the ages of 3 and 10, but the disorder can appear at any age. Many of the neurological problems that can occur in biotin-thiamine-responsive basal ganglia disease affect movement, and can include involuntary tensing of various muscles (dystonia), muscle rigidity, muscle weakness on one or both sides of the body (hemiparesis or quadriparesis), problems coordinating movements (ataxia), and exaggerated reflexes (hyperreflexia). Movement problems can also affect the face, and may include the inability to move facial muscles due to facial nerve paralysis (supranuclear facial palsy), paralysis of the eye muscles (external ophthalmoplegia), difficulty chewing or swallowing (dysphagia), and slurred speech. Affected individuals may also experience confusion, loss of previously learned skills, intellectual disability, and seizures. Severe cases may result in coma and become life-threatening. Typically, the neurological symptoms occur as increasingly severe episodes, which may be triggered by fever, injury, or other stresses on the body. Less commonly, the signs and symptoms persist at the same level or slowly increase in severity over time rather than occurring as episodes that come and go. In these individuals, the neurological problems are usually limited to dystonia, seizure disorders, and delay in the development of mental and motor skills (psychomotor delay).
Diagnosis[edit]
Biotin-thiamine-responsive basal ganglia disease (BTBGD) should be suspected in individuals with the following: Acute/subacute encephalopathy with seizures, extrapyramidal manifestations (dystonia, cogwheel rigidity, dysarthria, dysphagia), and pyramidal tract signs (quadriparesis, hyperreflexia) typically in a child age three to ten years and usually preceded by febrile illness or some other stress. Cerebellar signs, supranuclear facial nerve palsy, external ophthalmoplegia, and ataxia are variably present. Brain MRI showing the following:
- Swelling and bilateral and symmetric increased T2-weighted signal intensity in the caudate nucleus, putamen, thalamus, infra- and supratentorial brain cortex, and brain stem .
- Vasogenic edema during acute crises as demonstrated by diffusion-weighted imaging / apparent diffusion coefficient MRI
- Chronic changes including atrophy and necrosis of caudate and putamen with diffuse cerebral cortical and (to a lesser extent) cerebellar atrophy .
- Spinal cord involvement (seen in 1 affected individual)
- Normal laboratory investigations, including tandem mass spectrometry of blood; urine gas chromatography-mass spectrometry (GC-MS); serum concentrations of lactic acid,* ammonia, biotin, and thiamine; serum biotinidase enzyme activity; urine amino acids; plasma amino acids; liver enzymes; coagulation profile; lipid profile; and cerebrospinal fluid (CSF) cell count, protein, glucose, and cultures.
- In the early-onset form, high lactate levels in the blood and CSF; high alanine, leucine, and isoleucine in the plasma; and elevated excretion of α-ketoglutarate in the urinary organic acid assays can be observed.
Family history consistent with autosomal recessive inheritance.
Treatment[edit]
Biotin (5-10 mg/kg/day) and thiamine (up to 40 mg/kg/day with a maximum of 1500 mg daily) are given orally as early in the disease course as possible and are continued lifelong. Symptoms typically resolve within days. Acute encephalopathic episodes may require care in an ICU to manage seizures and increased intracranial pressure; during acute decompensations thiamine may be increased to double the regular dose and be given intravenously. Antiepileptic drugs are used to control seizures. Treatment of dystonia is symptomatic and includes administration of trihexyphenidyl or L-dopa. Rehabilitation, physiotherapy, occupational therapy, and speech therapy as needed and adaptation of educational programs to meet individual needs. Education of the family regarding the importance of lifelong compliance with medical therapy.
NIH genetic and rare disease info[edit]
Biotin-thiamine-responsive basal ganglia disease is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Biotin-thiamine-responsive basal ganglia disease
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian