Parsonage–Turner syndrome

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Parsonage–Turner syndrome | |
|---|---|
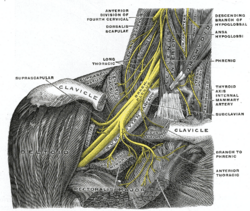 | |
| Synonyms | Brachial neuritis, neuralgic amyotrophy |
| Pronounce | |
| Specialty | Neurology |
| Symptoms | Sudden onset of shoulder pain, followed by muscle weakness and atrophy |
| Complications | N/A |
| Onset | Typically between 20 and 60 years of age |
| Duration | Weeks to months |
| Types | N/A |
| Causes | Idiopathic, possibly autoimmune |
| Risks | Recent infection, surgery, vaccination |
| Diagnosis | Clinical evaluation, electromyography |
| Differential diagnosis | Cervical radiculopathy, rotator cuff tear, frozen shoulder |
| Prevention | N/A |
| Treatment | Physical therapy, pain management |
| Medication | N/A |
| Prognosis | Generally good, but recovery can take months to years |
| Frequency | Rare |
| Deaths | N/A |
Parsonage–Turner syndrome (PTS), also known as acute brachial neuritis or brachial plexopathy, is a rare neurological disorder characterized by sudden onset of severe shoulder and upper arm pain followed by muscle weakness and atrophy. The condition primarily affects the brachial plexus, a network of nerves that sends signals from the spinal cord to the shoulder, arm, and hand.
Signs and Symptoms[edit]
The hallmark of Parsonage–Turner syndrome is the sudden onset of severe pain in the shoulder and upper arm, which can last from hours to weeks. This pain is typically followed by muscle weakness, atrophy, and sometimes sensory loss in the affected areas. The symptoms often appear on one side of the body but can occasionally affect both sides.
Causes[edit]
The exact cause of Parsonage–Turner syndrome is unknown. However, it is believed to be related to an autoimmune response, where the body's immune system mistakenly attacks the nerves of the brachial plexus. Possible triggers include infections, vaccinations, surgery, or trauma.
Diagnosis[edit]
Diagnosis of Parsonage–Turner syndrome is primarily clinical, based on the patient's history and physical examination. Electromyography (EMG) and nerve conduction studies (NCS) can help confirm the diagnosis by showing characteristic patterns of nerve damage. Magnetic resonance imaging (MRI) may also be used to rule out other conditions.
Treatment[edit]
There is no specific cure for Parsonage–Turner syndrome. Treatment focuses on managing pain and improving function. Nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, and physical therapy are commonly used. In some cases, nerve blocks or opioids may be necessary for pain management.
Prognosis[edit]
The prognosis for Parsonage–Turner syndrome varies. While many patients experience significant recovery within 1 to 2 years, some may have persistent weakness or pain. Early intervention with physical therapy can improve outcomes.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian