Familial lipoprotein lipase deficiency
Other Names: LPL deficiency; Lipoprotein lipase deficiency; Type I hyperlipoproteinemia; Familial hyperchylomicronemia; Familial LPL deficiency; Burger-Grutz syndrome; Endogenous hypertriglyceridaemia; Familial fat-induced hypertriglyceridemia; Lipase D deficiency; LIPD deficiency; Lipoprotein lipase deficiency, familial
Familial lipoprotein lipase deficiency is a rare genetic disorder is which a person lacks the enzyme lipoprotein lipase, a protein needed to break down fat molecules. Deficiency of this enzyme prevents affected individuals from properly digesting certain fats. This results in the accumulation of fatty droplets called chylomicrons in the blood and an increase in the blood concentration of triglycerides.
Onset[edit]
People with familial lipoprotein lipase deficiency typically develop signs and symptoms before age 10, with one-quarter showing symptoms by age 1.
Epidemiology[edit]
This condition affects about 1 per million people worldwide. It is much more common in certain areas of the province of Quebec, Canada.
Cause[edit]
Mutations in the LPL gene cause familial lipoprotein lipase deficiency. The LPL gene provides instructions for producing an enzyme called lipoprotein lipase, which is found primarily on the surface of cells that line tiny blood vessels (capillaries) within muscles and fatty (adipose) tissue. This enzyme helps break down fats called triglycerides, which are carried by molecules called lipoproteins.
Mutations that cause familial lipoprotein lipase deficiency lead to a reduction or elimination of lipoprotein lipase activity, which prevents the enzyme from effectively breaking down triglycerides. As a result, triglycerides attached to lipoproteins build up in the blood and tissues, leading to the signs and symptoms of familial lipoprotein lipase deficiency.
Inheritance[edit]
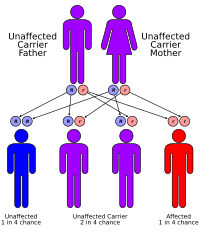
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Researchers speculate that if family members of affected individuals have a mutation in one copy of the LPL gene in each cell, they may have a mild increase in fat levels in the blood, which could increase their risk of health problems such as heart disease or diabetes. However, studies have not clearly demonstrated whether these individuals are more prone to develop these health problems than individuals in the general population.
Signs and symptoms[edit]
The first symptom of this condition is usually abdominal pain, which can vary from mild to severe. The abdominal pain is often due to inflammation of the pancreas (pancreatitis). These episodes of pancreatitis begin as sudden (acute) attacks. If left untreated, pancreatitis can develop into a chronic condition that can damage the pancreas and, in rare cases, be life-threatening.
Affected individuals may also have an enlarged liver and spleen (hepatosplenomegaly). The higher the levels of fat in the body, the larger the liver and spleen become. As fat levels rise, certain white blood cells called macrophages take in excess fat in an attempt to rid fat from the bloodstream. After taking in fat, the macrophages travel to the liver and spleen, where the fatty cells accumulate.
Approximately half of individuals with familial lipoprotein lipase deficiency develop small yellow deposits of fat under the skin called eruptive xanthomas. These fat deposits most commonly appear on the trunk, buttocks, knees, and arms. Eruptive xanthomas are small (about 1 millimeter in diameter), but individual xanthomas can cluster together to form larger patches. They are generally not painful unless exposed to repeated friction or abrasion. Eruptive xanthomas begin to appear when fat intake increases and levels rise; the deposits disappear when fat intake slows and levels decrease.
The blood of people with familial lipoprotein lipase deficiency can have a milky appearance due to its high fat content. When fat levels get very high in people with this condition, fats can accumulate in blood vessels in the tissue that lines the back of the eye (the retina). The fat buildup gives this tissue a pale pink appearance when examined (lipemia retinalis). This fat accumulation does not affect vision and will disappear once fats from the diet are reduced and levels in the body decrease.
In people with familial lipoprotein lipase deficiency, increased fat levels can also cause neurological features, such as depression, memory loss, and mild intellectual decline (dementia). These problems are remedied when dietary fat levels normalize.
Diagnosis[edit]
Familial lipoprotein lipase (LPL) deficiency should be suspected in individuals (particularly those age <40 years) with the following clinical and supportive laboratory findings.
Clinical findings
- Recurrent acute pancreatitis
- Eruptive cutaneous xanthomata
- Hepatosplenomegaly
Supportive laboratory findings
- Impaired clearance of chylomicrons from plasma causing the plasma to have a milky (lactescent or lipemic) appearance
- Plasma triglyceride concentrations greater than 2000 mg/dL in the untreated state, regardless of fasting status
Establishing the Diagnosis The diagnosis of LPL deficiency is established in a proband by the identification of biallelic pathogenic variants in LPL on molecular genetic testing.
Treatment[edit]
Medical nutrition therapy. Morbidity and mortality can be prevented by maintaining plasma triglyceride concentration at less than 2000 mg/dL; a good clinical goal is less than 1000 mg/dL .
Restriction of dietary fat to no more than 20 g/day or 15% of total energy intake is usually sufficient to reduce plasma triglyceride concentration and to keep the individual with familial LPL deficiency free of symptoms.
Medium-chain triglycerides may be used for cooking, as they are absorbed directly into the portal vein without becoming incorporated into chylomicron triglyceride.
The success of therapy depends on the individual's acceptance of the fat restriction, including both unsaturated and saturated fat. Note: Fish oil supplements, which are effective in disorders of excess hepatic triglyceride production, are not effective in LPL deficiency and are contraindicated (see Agents/Circumstances to Avoid).
The enlarged liver and spleen can return to normal size within one week of lowering of triglyceride concentrations.
The xanthomas can clear over the course of weeks to months. Recurrent or persistent eruptive xanthomas indicate inadequate therapy.
Pancreatitis associated with the chylomicronemia syndrome is treated in the manner typical for other forms of pancreatitis.
Discontinuation of oral fat intake stops chylomicron triglyceride formation, and replacement with hypocaloric parenteral nutrition decreases VLDL triglyceride production.
Administration of excess calories, as in hyperalimentation, is contraindicated in the acute state. The intravenous administration of lipid emulsions may lead to persistent or recurrent pancreatitis. If recurrent pancreatitis with severe hypertriglyceridemia occurs, total dietary fat intake needs to be reduced.
| Inborn error of lipid metabolism: dyslipidemia (E78, 272.0–272.6) | ||||||||
|---|---|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
Familial lipoprotein lipase deficiency is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Familial lipoprotein lipase deficiency
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian