2-methyl-3-hydroxybutyric aciduria
Alternate names[edit]
HSD10 deficiency; 3H2MBD deficiency; 3-hydroxy-2-methylbutyryl-CoA dehydrogenase deficiency; Hydroxyacyl-CoA dehydrogenase II deficiency; 2M3HBA; 17 beta-hydroxysteroid dehydrogenase type 10 deficiency; 2-methyl-3-hydroxybutyryl-CoA dehydrogenase deficiency; MHBD deficiency; HSD10 mitochondrial disease; 2-methyl-3-hydroxybutyric aciduria
Definition[edit]
HSD10 disease (also known as 2-methyl-3-hydroxybutyric aciduria) is an inherited disorder in which the body cannot effectively process the amino acid isoleucine. HSD10 disease is a disorder that affects the nervous system, vision, and heart. It is typically more severe in males than in females.
Epidemiology[edit]
HSD10 disease is a very rare disorder. Its prevalence is less than 1 in 1 million people.
Cause[edit]
- HSD10 disease is caused by mutations in the HSD17B10 gene, which provides instructions for making the HSD10 protein.
- This protein is located within mitochondria, the energy-producing centers inside cells, where it is involved in the production (synthesis) of proteins.
- While most protein synthesis occurs in the fluid surrounding the nucleus (cytoplasm), a few proteins are synthesized in the mitochondria.
- During protein synthesis, in either the mitochondria or the cytoplasm, molecules called transfer RNAs (tRNAs) help assemble protein building blocks (amino acids) into chains that form proteins.
- The HSD10 protein is part of a group of proteins (a complex) that is involved in making functional mitochondrial tRNA molecules, which aid in the synthesis of mitochondrial proteins.
- Normal mitochondrial protein production is essential for the formation of the groups of proteins that convert the energy from food into a form cells can use.
Gene mutations[edit]
- The HSD17B10 gene mutations that cause HSD10 disease reduce the amount of HSD10 protein in cells, impair their structure or function, or both, which leads to a deficiency of the functional complex in which it plays a part. This deficiency impairs the production of mitochondrial tRNAs.
- Without enough tRNAs, the mitochondrial synthesis of proteins involved in cellular energy production is reduced.
- A shortage of these proteins results in insufficient energy production in cells of the brain, eyes, and heart, leading to the characteristic features of HSD10 disease.
Inheritance[edit]
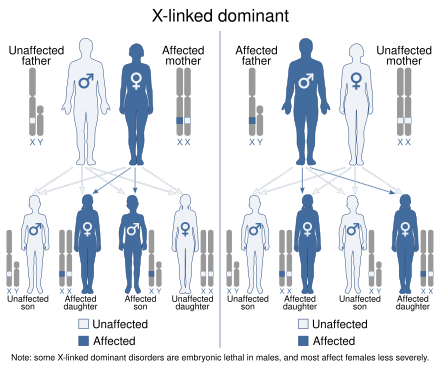
It has an X-linked dominant pattern of inheritance.
Signs and symptoms[edit]
- Signs and symptoms of this condition usually develop in infancy or early childhood and include metabolic acidosis, hypoglycemia, hypotonia, seizures, movement problems, retinal degeneration, and hearing loss.
- Affected males have severe neurodegeneration with loss of developmental milestones, whereas females have mild to moderate developmental delay.
Clinical presentation[edit]
For most diseases, symptoms will vary from person to person. People with the same disease may not have all the symptoms listed.
80%-99% of people have these symptoms
- Abnormal urinary acylglycine profile
30%-79% of people have these symptoms
- Delayed speech and language development(Deficiency of speech development)
- Developmental regression(Loss of developmental milestones)
- Elevated urinary 3-hydroxybutyric acid
- Global developmental delay
- Intellectual disability, moderate(IQ between 34 and 49)
- Progressive visual loss(Progressive loss of vision)
- Seizure
- Specific learning disability
5%-29% of people have these symptoms
- Abnormal social behavior(Abnormal social behaviour)
- Ataxia
- Autistic behavior
- Choreoathetosis
- Chronic lactic acidosis
- Dysarthria(Difficulty articulating speech)
- Focal white matter lesions
- Frontotemporal cerebral atrophy
- Gait disturbance(Abnormal gait)
- Hearing impairment(Deafness)
- Infantile muscular hypotonia(Decreased muscle tone in infant)
- Myoclonus
- Optic atrophy
- Short attention span(Poor attention span)
1%-4% of people have these symptoms
- Drooling(Dribbling)
- Dysphagia(Poor swallowing)
- Gastrointestinal dysmotility
- Hyperreflexia(Increased reflexes)
- Microcephaly(Abnormally small skull)
- Nasogastric tube feeding in infancy
- Nonprogressive encephalopathy
- Nystagmus(Involuntary, rapid, rhythmic eye movements)
- Postnatal growth retardation(Growth delay as children)
- Rigidity(Muscle rigidity)
- Spastic paraparesis
- Tremor
- Ventriculomegaly
Diagnosis[edit]
- Although the diagnosis can be aided by the observation of increased urinary levels of metabolites of isoleucine breakdown (2-methyl-3 hydroxybutyrate and tiglylglycine), there is not a correlation between these laboratory features and the phenotype.
- In addition, patients do not develop severe metabolic crises in the neonatal period as observed in other organic acidurias, but may show persistent lactic acidosis, most likely reflecting mitochondrial dysfunction.
Treatment[edit]
- There is no effective treatment for the disease. A low-protein, high-energy dietary regimen with carnitine supplementation reduces the accumulation of isoleucine metabolites in blood and urine, but does not improve psychomotor deterioration.
- Due to its ability to interfere with mitochondrial energy metabolism, valproic acid should be avoided.
NIH genetic and rare disease info[edit]
2-methyl-3-hydroxybutyric aciduria is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - 2-methyl-3-hydroxybutyric aciduria
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian