Parkes Weber syndrome

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Parkes Weber syndrome | |
|---|---|

| |
| Synonyms | |
| Pronounce | |
| Specialty | Vascular surgery, Genetics |
| Symptoms | Arteriovenous malformation, limb hypertrophy, varicose veins |
| Complications | Heart failure, bleeding, ulceration |
| Onset | Congenital |
| Duration | Chronic |
| Types | |
| Causes | Genetic mutation |
| Risks | |
| Diagnosis | Clinical diagnosis, imaging studies |
| Differential diagnosis | Klippel–Trénaunay syndrome, Proteus syndrome |
| Prevention | |
| Treatment | Surgical intervention, embolization, compression therapy |
| Medication | |
| Prognosis | Variable, depending on severity |
| Frequency | Rare |
| Deaths | |
Alternate names[edit]
PKWS
Definition[edit]
Parkes Weber syndrome is a disorder of the vascular system, which is the body's complex network of blood vessels. The vascular system consists of arteries, which carry oxygen-rich blood from the heart to the body's various organs and tissues; veins, which carry blood back to the heart; and capillaries, which are tiny blood vessels that connect arteries and veins.
Summary[edit]
Parkes Weber syndrome is characterized by vascular abnormalities known as capillary malformations and arteriovenous fistulas (AVFs), which are present from birth. The capillary malformations increase blood flow near the surface of the skin. They usually look like large, flat, pink stains on the skin, and because of their color are sometimes called "port-wine stains."
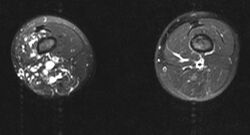
Epidemiology[edit]
Parkes Weber syndrome is a rare condition; its exact prevalence is unknown.
Cause[edit]
Some cases of Parkes Weber syndrome result from mutations in the RASA1 gene. When the condition is caused by RASA1 gene mutations, affected individuals usually have multiple capillary malformations. People with Parkes Weber syndrome who do not have multiple capillary malformations are unlikely to have mutations in the RASA1 gene; in these cases, the cause of the condition is often unknown. The RASA1 gene provides instructions for making a protein known as p120-RasGAP, which is involved in transmitting chemical signals from outside the cell to the nucleus. These signals help control several important cell functions, including the growth and division (proliferation) of cells, the process by which cells mature to carry out specific functions (differentiation), and cell movement. The role of the p120-RasGAP protein is not fully understood, although it appears to be essential for the normal development of the vascular system. Mutations in the RASA1 gene lead to the production of a nonfunctional version of the p120-RasGAP protein. A loss of this protein's activity disrupts tightly regulated chemical signaling during development. However, it is unclear how these changes lead to the specific vascular abnormalities and limb overgrowth seen in people with Parkes Weber syndrome.
Inheritance[edit]
Most cases of Parkes Weber syndrome occur in people with no history of the condition in their family. These cases are described as sporadic. When Parkes Weber syndrome is caused by mutations in the RASA1 gene, it is sometimes inherited from an affected parent. In these cases, the condition has an autosomal dominant pattern of inheritance. Autosomal dominant inheritance means one copy of the altered gene in each cell is sufficient to cause the disorder.
Signs and symptoms[edit]
The signs and symptoms of Parkes Weber syndrome include:
- Birthmarks caused by capillary malformations on the skin; they increase blood flow near the surface of the skin and usually look like large, flat, pink stains on the skin, and because of their color are sometimes called "port-wine stains."
- Hypertrophy (excessive growth) of the bone and soft tissue of the affected limb (which may lead to a difference in size between the affected and non-affected limb).
- Multiple arteriovenous fistulas (AVFs) due to abnormal connections between arteries and veins. These AVFs can be associated with life-threatening complications including abnormal bleeding and heart failure.
Some vascular abnormalities seen in Parkes Weber syndrome are similar to those that occur in a condition called capillary malformation-arteriovenous malformation syndrome (CM-AVM). CM-AVM and some cases of Parkes Weber syndrome have the same genetic cause. For most diseases, symptoms will vary from person to person. People with the same disease may not have all the symptoms listed. 80%-99% of people have these symptoms
- Abnormal bleeding(Bleeding tendency)
- Hypertrophy of the lower limb
- Hypertrophy of the upper limb(Increased size of upper limb)
- Nevus flammeus(port-wine stain)
- Peripheral arteriovenous fistula
- Telangiectasia of the skin
30%-79% of people have these symptoms
5%-29% of people have these symptoms
- Congestive heart failure(Cardiac failure)
- Glaucoma
- Headache(Headaches)
- Hemiparesis(Weakness of one side of body)
Diagnosis[edit]
Making a correct diagnosis for a genetic and rare disease is oftentimes very challenging. So the doctors and other healthcare professions rely on the person's medical history, the severity of the symptoms, physical examination and lab tests to make and confirm a diagnosis. There is a possibility of interpreting the symptoms of PWS with other conditions such as AVMs and or AVFs. This is because AVMs and AVFs also involve the characteristic overgrowth in soft tissue, bone and brain. Also PWS can be misdiagnosed with Klippel–Trenaunay syndrome (KTS). However, KTS consists of the following: triad capillary malformation, venous malformation, and lymphatic malformation. Usually a specific set of symptoms such as capillary and arteriovenous malformations occur together and this is used to distinguish PWS from similar conditions. Arteriovenous malformations (AVMs) and arteriovenous fistulas (AVFs) are caused by RASA1 mutations as well. Therefore, if all the other tests fail to determine PWS, which is highly unlikely, genetic testing such as sequence analysis and gene-targeted deletion/duplication analysis can be performed to identify possible RASA1 gene mutations. PWS can be distinguished from other conditions because of its defining port-wine stains that are large, flat and pink. The port-wine stains and physical examination are enough to diagnose PWS. But additional testing is necessary to determine the extent of the PWS syndrome. The following tests may be ordered by physicians to help determine the appropriate next steps: MRI, ultrasound, CT/CAT scan, angiogram, and echocardiogram. MRI: This is a high-resolution scan that is used to identify the extent of the hypertrophy or overgrowth of the tissues. This can also be used to identify other complications that may arise a result of hypertrophy. Angiogram Ultrasound: this can be necessary to examine the vascular system and determine how much blood is actually flowing through the AVMs. CT/CAT scan: this scan is especially useful for examining the areas affected by PWS and is helpful for evaluating the bones in the overgrown limb. Angiogram: an angiogram can also be ordered to get a detailed look at the blood vessels in the affected or overgrown limb. In this test an interventional radiologist injects a dye into the blood vessels that will help see how the blood vessels are malformed. Echocardiogram: depending on the intensity of the PWS syndrome, an echo could also be ordered to check the condition of the heart. PWS often requires a multidisciplinary care. Depending on the symptoms, patients are dependent on: dermatologists, plastic surgeons, general surgeons, interventional radiologists, orthopedists, hematologists, neurosurgeons, vascular surgeons and cardiologists. Since the arteriovenous and capillary malformations cannot be completely reconstructed and depending on the extent and severity of the malformations, these patients may be in the care of physicians for their entire lives.
Treatment[edit]
No cure currently exists. Treatment depends on the symptoms and usually involves several specialists, such as interventional radiologist, neurosurgeons, vascular surgeons, cardiologists and dermatologists. Heart problems should be treated by a cardiologist. The arteriovenous malformations (AVMs) and/or arteriovenous fistulas are treated with surgery or with embolization. Leg differences are treated by an orthopedist. Capillary malformations can be treated by a dermatologist when the patients are concerned with the cosmetic appearance. Supportive care may include compression garments (tight-fitting pieces of clothing on the affected limb to reduce pain and swelling); these may also protect the limb from bumps and scrapes, which can cause bleeding and are also recommended in cases of lymphedema. Heel inserts may be used if the legs are different lengths, which can aid in walking normally. Various pain medications and antibiotic medications may be prescribed as needed.
Prognosis[edit]
PWS is a progressive condition and advances with age. It is dependent on the extent of the disease and overgrowth, condition of the patient's heart, if the blood vessels are responsive to treatment, overall health of the patient, tolerance of medications and treatments. Based on these factors the prognosis is fair to good. The deformity and overgrowth tend to progress with time until epiphyseal closure. A lot of medical attention is needed to correct the blood vessels.
| Deficiencies of intracellular signaling peptides and proteins | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
Parkes Weber syndrome is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Parkes Weber syndrome
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian