Ceroid lipofuscinosis neuronal 1
Other Names: CLN1; CLN1 variable age at onset; Neuronal ceroid lipofuscinosis 1
CLN1 disease is an inherited disorder that primarily affects the nervous system.
CLN1 disease is one of a group of disorders known as neuronal ceroid lipofuscinoses (NCLs), which may also be collectively referred to as Batten disease. All these disorders affect the nervous system and typically cause worsening problems with vision, movement, and thinking ability. The different NCLs are distinguished by their genetic cause. Each disease type is given the designation "CLN," meaning ceroid lipofuscinosis, neuronal, and then a number to indicate its subtype.
Epidemiology[edit]
The incidence of CLN1 disease is unknown; more than 200 cases have been described in the scientific literature. Collectively, all forms of NCL affect an estimated 1 in 100,000 individuals worldwide. NCLs are more common in Finland, where approximately 1 in 12,500 individuals are affected.
Cause[edit]
Mutations in the PPT1 gene cause CLN1 disease. The PPT1 gene provides instructions for making an enzyme called palmitoyl-protein thioesterase 1. This enzyme is active in cell compartments called lysosomes, which digest and recycle different types of molecules. Palmitoyl-protein thioesterase 1 removes fats called long-chain fatty acids from certain proteins, which helps to break down the proteins. Palmitoyl-protein thioesterase 1 is also thought to be involved in a variety of other cell functions.
PPT1 gene mutations that cause CLN1 disease decrease or eliminate the production or function of palmitoyl-protein thioesterase 1. A reduction of functional enzyme impairs the removal of fatty acids from certain proteins. These partially broken down fats and proteins accumulate in lysosomes. While accumulation of these substances occurs in cells throughout the body, nerve cells appear to be particularly vulnerable to damage caused by the abnormal cell materials. Early and widespread loss of nerve cells in CLN1 disease leads to severe signs and symptoms and death in childhood.
In the later-onset cases of CLN1 disease, PPT1 gene mutations result in the production of a palmitoyl-protein thioesterase 1 enzyme that has a reduced level of normal function; however, protein function in these individuals is higher than in those who have the condition beginning in early childhood. As a result, long-chain fatty acids are removed from some proteins, allowing for a small amount of proteins to be broken down. Since it takes longer for these substances to accumulate in lysosomes and cause nerve cell death, the signs and symptoms of CLN1 disease in these individuals occur later in life.
Inheritance[edit]
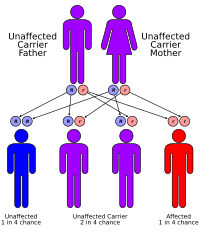
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Signs and symptoms[edit]
Individuals with this condition have normal development in infancy, but typically by 18 months they become increasingly irritable and begin to lose previously acquired skills (developmental regression).
In affected children, nerve cells in the brain die over time, leading to an overall loss of brain tissue (brain atrophy) and an unusually small head (microcephaly). Children with CLN1 disease have decreased muscle tone (hypotonia), intellectual and motor disability, and rarely are able to speak or walk. Some affected children develop repetitive hand movements.
By age 2, individuals with this condition often have muscle twitches (myoclonus), recurrent seizures (epilepsy), and vision loss. Some affected children develop frequent respiratory infections. As the condition worsens, children have severe feeding difficulties that often require a feeding tube.
Children with CLN1 disease usually do not survive past childhood. Some people with CLN1 disease do not develop symptoms until later in childhood or in adulthood. As with younger affected children, older individuals develop a decline in intellectual function, myoclonus, epilepsy, and vision loss. In these individuals, life expectancy depends on when signs and symptoms of CLN1 disease develop and their severity; affected individuals may survive only into adolescence or through adulthood. Adults with CLN1 disease may also have movement disorders, including impaired muscle coordination (ataxia) or a pattern of movement abnormalities known as parkinsonism.
Diagnosis[edit]
The diagnosis of an NCL is increasingly based on assay of enzyme activity and molecular genetic testing. In unusual cases diagnosis relies on electron microscopy (EM) of biopsied tissues. The diagnostic testing strategy in a proband depends on the age of onset.
Electron microscopy (EM) studies can be performed with 5-10 mL of heparinized whole blood (lymphocytes) or tissue biopsies (now usually of skin, but previously of conjunctiva or other tissues).
Granular osmiophilic deposits (GROD) in CLN1 diseas.
Enzyme activity. Three lysosomal enzymes have been identified as being deficient in the neuronal ceroid-lipofuscinoses in white blood cells, fibroblasts, and chorionic villi:
Palmitoyl-protein thioesterase 1 (PPT-1) encoded by PPT1.
A fluorimetric assay for PPT-1 based on the fluorochrome 4-methylumbelliferone detects significantly reduced PPT-1 activity in leukocytes, fibroblasts, lymphoblasts, amniotic fluid cells, or chorionic villi in forms of NCL caused by PPT1 pathogenic variants.
MRI findings are: variable cerebral atrophy; signal change in the thalami and basal ganglia; and thin, hyperintense, periventricular high-signal rims of white matter . The progressive diffuse brain atrophy on MRI seen in children with INCL during the first four years of life then stabilizes.
Treatment[edit]
Symptomatic treatment can be successful in mitigating the manifestations of NCL. Seizures, sleep-related problems, malnutrition, gastroesophageal reflux, pneumonia, sialorrhea, hyperactivity and behavior problems, psychosis, anxiety, spasticity, Parkinsonian symptoms, and dystonia can be palliated.
Seizures
- Antiepileptic drugs (AEDs) should be selected with caution. The stage of the disease, age of the affected individual, and quality of life are important to consider in evaluating the effectiveness of AEDs.
- Lamotrigine (LTG) had a favorable effect on 23/28 individuals with JNCL, 13/19 being continued on monotherapy with 100% control, compared to 70% control for those receiving valproic acid (VPA), 60% control for VPA-clonazepam (CZP), and 60% control for LTG-CZP .Other newer AEDs including levetiracetam and topiramate may also be beneficial .
Other
- Benzodiazepines may be of benefit for seizures, anxiety, spasticity, and sleep disorders.
- Trihexyphenydil improves dystonia and sialorrhea.
- Individuals with swallowing problems may benefit from placement of a gastric (G) tube.
| Lysosomal storage diseases: Inborn errors of lipid metabolism (Lipid storage disorders) | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
Ceroid lipofuscinosis neuronal 1 is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Ceroid lipofuscinosis neuronal 1
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian