Necrotizing gingivitis

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Necrotizing gingivitis | |
|---|---|
 | |
| Synonyms | Trench mouth, Vincent's infection, Vincent's angina, acute necrotizing ulcerative gingivitis (ANUG) |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Painful, bleeding gums, ulceration of the gums, halitosis |
| Complications | Periodontitis, tooth loss, systemic infection |
| Onset | Sudden |
| Duration | Varies, can be chronic if untreated |
| Types | N/A |
| Causes | Bacterial infection, poor oral hygiene, stress, smoking, malnutrition |
| Risks | Immunocompromised individuals, smokers, poor oral hygiene |
| Diagnosis | Clinical examination, history, sometimes microbiological culture |
| Differential diagnosis | Herpetic gingivostomatitis, aphthous stomatitis, leukemia |
| Prevention | Good oral hygiene, regular dental check-ups, avoiding smoking |
| Treatment | Antibiotics, professional dental cleaning, improved oral hygiene |
| Medication | Metronidazole, Amoxicillin, Chlorhexidine mouthwash |
| Prognosis | Good with treatment, but recurrence possible |
| Frequency | Rare in developed countries, more common in developing regions |
| Deaths | N/A |
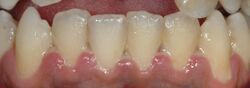
A severe form of gingivitis characterized by tissue necrosis
Necrotizing gingivitis (NG), also known as trench mouth, is a painful infection of the gums that is characterized by necrosis of gingival tissues, bleeding, and halitosis. It is a type of periodontal disease and is considered a dental emergency due to its rapid progression and potential for serious complications.
Signs and symptoms[edit]
Necrotizing gingivitis presents with a number of distinctive signs and symptoms:
- Pain: Patients often experience severe pain in the gums, which can be exacerbated by eating or brushing.
- Bleeding: Spontaneous bleeding of the gums is common, and the gums may bleed easily when touched.
- Ulceration: The gingival tissues exhibit ulcerations, often starting at the tips of the interdental papillae and spreading along the gum line.
- Necrosis: There is visible necrosis of the gingival tissues, which may appear as grayish sloughing areas.
- Halitosis: A characteristic foul odor, often described as "fetid breath," is present due to tissue necrosis and bacterial activity.
- Metallic taste: Some patients report a metallic taste in their mouth.
Causes[edit]
Necrotizing gingivitis is primarily caused by an overgrowth of specific bacteria in the mouth, including Fusobacterium, Prevotella intermedia, and Treponema. These bacteria thrive in conditions of poor oral hygiene, stress, smoking, and immunosuppression. The condition is more prevalent in individuals with compromised immune systems, such as those with HIV/AIDS or malnutrition.
Diagnosis[edit]
Diagnosis of necrotizing gingivitis is typically based on clinical examination. The presence of characteristic symptoms such as gingival pain, bleeding, and necrosis, along with a history of risk factors, aids in diagnosis. In some cases, a microbiological culture may be performed to identify the specific bacterial pathogens involved.
Treatment[edit]
The treatment of necrotizing gingivitis involves several steps:
- Debridement: The primary treatment is the mechanical removal of necrotic tissue and plaque through professional dental cleaning.
- Antibiotics: Systemic antibiotics, such as metronidazole or penicillin, may be prescribed to control bacterial infection.
- Oral hygiene: Patients are advised to maintain meticulous oral hygiene, including gentle brushing and the use of antiseptic mouth rinses.
- Pain management: Analgesics may be used to manage pain.
- Lifestyle modifications: Patients are encouraged to reduce stress, quit smoking, and improve their nutritional status.
Prognosis[edit]
With prompt and appropriate treatment, the prognosis for necrotizing gingivitis is generally good. However, if left untreated, the condition can progress to more severe forms of periodontal disease, such as necrotizing periodontitis or necrotizing stomatitis, which can lead to significant tissue destruction and systemic complications.
Prevention[edit]
Preventive measures for necrotizing gingivitis include maintaining good oral hygiene, regular dental check-ups, stress management, smoking cessation, and ensuring adequate nutrition. Individuals with compromised immune systems should be particularly vigilant in their oral care routines.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian