Level 1 placental abruption
Placental abruption, a severe obstetric complication, involves the untimely detachment of an ordinarily implanted placenta from the uterus. The Gaia Level 1 Placental Abruption classification focuses on prompt detection and apt intervention, prioritizing the well-being of both mother and fetus.
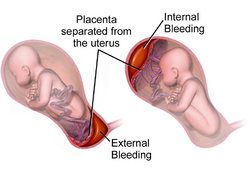
Gaia Level 1 Placental Abruption is discerned by two primary criteria:
- Observance of vaginal bleeding during the second or third trimester, with placenta previa ruled out via ultrasound.
- The presence of either:
- Uterine irritability, denoting inconsistent and frequent uterine activity without distinct contractions in a consistent sequence (commonly termed 'labor').
- Clinical symptoms aligning with hypovolemic shock or coagulopathy.
- An auxiliary definition for Gaia Level 1 emphasizes placental pathology. Here, histologic evidence of a chronic abruption becomes the basis to confirm a Level 1 Placental Abruption.
Pathophysiology[edit]
The onset of placental abruption is triggered by the rupturing of maternal blood vessels, which instigates bleeding at the decidual-placental juncture. This, in turn, can lead the placenta to separate from the uterus. Though the exact etiology remains ambiguous, potential risk factors encompass maternal hypertension, physical trauma, and a preceding episode of placental abruption.
Clinical Implications[edit]
The significance of identifying Gaia Level 1 Placental Abruption is manifold:
- It acts as a preliminary alert of probable evolution to intensified forms of abruption.
- Swift detection and intervention curtail risks for both mother and fetus, encompassing fetal distress, early childbirth, and extensive maternal bleeding.
- Chronic placental abruption, as inferred from histologic evidence, poses ramifications for subsequent pregnancies.
Management[edit]
Therapeutic approaches predominantly lean towards ensuring maternal stability and fetal health:
- Uninterrupted monitoring for signs of fetal distress.
- Surveillance of maternal vitals and diagnostic tests to gauge blood loss and coagulation profile.
- Depending on the gestational age, childbirth might be hastened if either the fetus reaches full term or any distress signs emerge in mother or fetus.
- In scenarios with minor abruptions but stable conditions for both mother and fetus, a watchful waiting strategy might be adopted, complemented by meticulous observation.
| Pathology of pregnancy, childbirth, and the puerperium | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
* ' Category'
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian