Chorioamnionitis

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Chorioamnionitis | |
|---|---|
| Synonyms | Intra-amniotic infection |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Fever, uterine tenderness, fetal tachycardia, maternal tachycardia, purulent or foul-smelling amniotic fluid |
| Complications | Preterm birth, neonatal sepsis, cerebral palsy |
| Onset | During pregnancy |
| Duration | Variable |
| Types | N/A |
| Causes | Bacterial infection of the amniotic fluid, placenta, fetus, or fetal membranes |
| Risks | Prolonged labor, premature rupture of membranes, multiple vaginal examinations, internal fetal monitoring |
| Diagnosis | Clinical diagnosis, confirmed by amniotic fluid culture |
| Differential diagnosis | Endometritis, urinary tract infection, pyelonephritis |
| Prevention | Antibiotic prophylaxis in high-risk cases |
| Treatment | Antibiotics, delivery of the baby |
| Medication | N/A |
| Prognosis | Generally good with treatment, but can lead to complications if untreated |
| Frequency | Common in cases of preterm labor |
| Deaths | N/A |
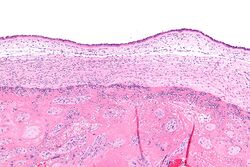
Chorioamnionitis, also known as intra-amniotic infection (IAI), is a bacterial infection that affects the chorion, amnion, and amniotic fluid around the fetus during pregnancy. This condition is a significant cause of preterm birth and can have serious consequences for both the mother and the fetus. It typically arises from a bacterial infection that ascends from the lower genital tract into the uterine cavity. The diagnosis is often based on clinical findings, including maternal fever, uterine tenderness, and foul-smelling amniotic fluid, although laboratory tests can provide further confirmation.
Causes and Risk Factors[edit]
The primary cause of chorioamnionitis is infection by bacteria, most commonly involving species such as Escherichia coli, group B Streptococcus, and anaerobic bacteria. Risk factors for developing chorioamnionitis include prolonged labor, premature rupture of membranes (PROM), multiple vaginal examinations during labor, and the use of internal monitoring devices. Women with a history of preterm delivery or those who have had invasive procedures during pregnancy, such as amniocentesis, are also at increased risk.
Symptoms and Diagnosis[edit]
Symptoms of chorioamnionitis can vary but often include maternal fever, increased heart rate in the mother or fetus, uterine tenderness, and foul-smelling amniotic fluid. Diagnosis is primarily clinical but can be supported by laboratory tests such as elevated maternal white blood cell count, elevated C-reactive protein, and amniotic fluid analysis showing signs of infection.
Treatment[edit]
Treatment for chorioamnionitis typically involves the administration of broad-spectrum antibiotics to the mother. In cases where the pregnancy is at a viable gestational age, delivery is often the recommended course of action to prevent further infection and potential harm to the fetus. Management strategies may also include supportive care for the mother and monitoring for signs of fetal distress.
Complications[edit]
Chorioamnionitis can lead to several serious complications, including preterm birth, neonatal sepsis, pulmonary hypoplasia in the fetus, and increased risk of cesarean section for the mother. Long-term, children born from pregnancies complicated by chorioamnionitis may face increased risks of cerebral palsy and other developmental issues.
Prevention[edit]
Preventive measures for chorioamnionitis focus on minimizing risk factors, such as reducing the number of vaginal examinations during labor and avoiding unnecessary invasive procedures during pregnancy. Early and effective treatment of vaginal infections during pregnancy can also reduce the risk of ascending infections leading to chorioamnionitis.
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian