Malonic aciduria

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Malonic aciduria | |
|---|---|
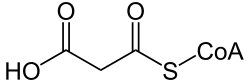 | |
| Synonyms | Malonyl-CoA decarboxylase deficiency |
| Pronounce | |
| Specialty | Medical genetics |
| Symptoms | Developmental delay, seizures, metabolic acidosis, hypoglycemia |
| Complications | N/A |
| Onset | Infancy |
| Duration | Lifelong |
| Types | N/A |
| Causes | Genetic mutation in the MLYCD gene |
| Risks | |
| Diagnosis | Genetic testing, urine organic acid analysis |
| Differential diagnosis | |
| Prevention | |
| Treatment | Dietary management, carnitine supplementation |
| Medication | |
| Prognosis | Variable, depending on severity |
| Frequency | Rare |
| Deaths | |
A rare metabolic disorder
Malonic aciduria, also known as malonyl-CoA decarboxylase deficiency, is a rare metabolic disorder characterized by the accumulation of malonic acid in the body. This condition is caused by a deficiency in the enzyme malonyl-CoA decarboxylase, which is crucial for the proper metabolism of certain fatty acids.
Pathophysiology[edit]
Malonic aciduria results from a deficiency in the enzyme malonyl-CoA decarboxylase, which is responsible for converting malonyl-CoA to acetyl-CoA and carbon dioxide. This enzyme deficiency leads to the accumulation of malonyl-CoA and malonic acid, disrupting normal fatty acid metabolism. The accumulation of these substances can interfere with energy production and other metabolic processes, leading to the symptoms observed in affected individuals.
Clinical Presentation[edit]
Individuals with malonic aciduria may present with a variety of symptoms, which can vary in severity. Common clinical features include:
- Developmental delay
- Hypotonia (reduced muscle tone)
- Seizures
- Cardiomyopathy
- Metabolic acidosis
- Failure to thrive
The onset of symptoms can occur in infancy or early childhood, and the severity can range from mild to life-threatening.
Genetics[edit]

Malonic aciduria is inherited in an autosomal recessive pattern, meaning that an individual must inherit two copies of the defective gene, one from each parent, to be affected by the disorder. The gene responsible for this condition is located on chromosome 16 and is known as MLYCD, which encodes the malonyl-CoA decarboxylase enzyme.
Diagnosis[edit]
The diagnosis of malonic aciduria is typically made based on clinical symptoms, biochemical testing, and genetic analysis. Key diagnostic tests include:
- Measurement of malonic acid levels in the urine and blood
- Enzyme assay to assess malonyl-CoA decarboxylase activity
- Genetic testing to identify mutations in the MLYCD gene
Management[edit]
There is currently no cure for malonic aciduria, and treatment is primarily supportive and symptomatic. Management strategies may include:
- Dietary modifications to reduce the intake of certain fatty acids
- Supplementation with carnitine to enhance fatty acid metabolism
- Medications to manage seizures and other symptoms
- Regular monitoring and supportive care to address developmental and metabolic needs
Prognosis[edit]
The prognosis for individuals with malonic aciduria varies depending on the severity of the enzyme deficiency and the effectiveness of management strategies. Early diagnosis and intervention can improve outcomes and quality of life for affected individuals.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian