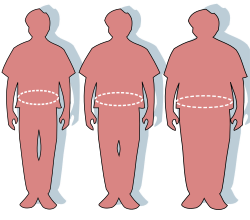
Obesity

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Obesity | |
|---|---|
| |
| Synonyms | Adiposity |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Excessive body fat, breathlessness, increased sweating, snoring, inability to cope with sudden physical activity, feeling very tired every day, back and joint pains |
| Complications | Cardiovascular disease, type 2 diabetes, obstructive sleep apnea, certain types of cancer, osteoarthritis, depression |
| Onset | Gradual |
| Duration | Long term |
| Types | N/A |
| Causes | Excessive food intake, lack of physical activity, genetic susceptibility |
| Risks | Sedentary lifestyle, unhealthy diet, genetic factors, medical conditions |
| Diagnosis | Body mass index (BMI) > 30 kg/m² |
| Differential diagnosis | Hypothyroidism, Cushing's syndrome, polycystic ovary syndrome |
| Prevention | Healthy diet, regular physical exercise |
| Treatment | Dieting, physical exercise, medications, surgery |
| Medication | Orlistat, liraglutide, phentermine |
| Prognosis | Variable, depends on comorbidities |
| Frequency | 650 million adults (13% of the world population) as of 2016 |
| Deaths | N/A |
Error: Image is invalid or non-existent.
Glossary of obesity terms Overweight and obesity are increasingly common conditions in the United States. They are caused by the increase in the size and the amount of fat cells in the body. Doctors measure body mass index (BMI) and waist circumference to screen and diagnose overweight and obesity. Obesity is a serious medical condition that can cause complications such as metabolic syndrome, high blood pressure, atherosclerosis, heart disease, diabetes, high blood cholesterol, cancers and sleep disorders. Treatment depends on the cause and severity of your condition and whether you have complications. Treatments include lifestyle changes, such as heart-healthy eating and increased physical activity, and Food and Drug Administration (FDA)-approved weight-loss medicines. For some people, surgery may be a treatment option.
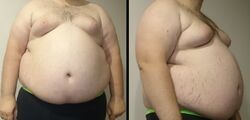
Causes- Overweight and Obesity[edit]
Energy imbalances, somegenetic or endocrine medical conditions, and certain medicines are known to cause overweight or obesity.
- Overweight and Obesity[edit]
Energy imbalances can cause overweight and obesity. An energy imbalance means that your energy IN does not equal your energy OUT. This energy is measured in calories. Energy IN is the amount of calories you get from food and drinks. Energy OUT is the amount of calories that your body uses for things such as breathing, digesting, being physically active, and regulating body temperature.
Overweight and obesity develop over time when you take in more calories than you use, or when energy IN is more than your energy OUT. This type of energy imbalance causes your body to store fat.
Your body uses certain nutrients such as carbohydrates or sugars, proteins, and fats from the foods you eat to:
- make energy for immediate use to power routine daily body functions and physical activity.
- store energy for future use by your body. Sugars are stored asglycogen in the liver and muscles. Fats are stored mainly as triglyceride in fat tissue.
The amount of energy that your body gets from the food you eat depends on the type of foods you eat, how the food is prepared, and how long it has been since you last ate.
The body has three types of fat tissue—white, brown, and beige—that it uses to fuel itself, regulate its temperature in response to cold, and store energy for future use. Learn about the role of each fat type in maintaining energy balance in the body.
- White fat tissue can be found around the kidneys and under the skin in the buttocks, thighs, and abdomen. This fat type stores energy, makes hormone that control the way the body regulates urges to eat or stop eating, and makesinflammatory substances that can lead to complications.
- Brown fat tissue is located in the upper back area of human infants. This fat type releases stored energy as heat energy when a baby is cold. It also can make inflammatory substances. Brown fat can be seen in children and adults.
- Beige fat tissue is seen in the neck, shoulders, back, chest and abdomen of adults and resembles brown fat tissue. This fat type, which uses carbohydrates and fats to produce heat, increases when children and adults are exposed to cold.
- Overweight and Obesity[edit]
Some genetic syndromes and endocrine disorders can cause overweight or obesity.
Genetic syndromes[edit]
Several genetic syndromes are associated with overweight and obesity, including the following.
- Prader-Willi syndrome
- Bardet-Biedl syndrome
- Alström syndrome
- Cohen syndrome
The study of these genetic syndromes has helped researchers understand obesity.
Endocrine disorders[edit]
Because the endocrine system produces hormones that help maintain energy balances in the body, the following endocrine disorders or tumor affecting the endocrine system can cause overweight and obesity.
- Hypothyroidism. People with this condition have low levels of thyroid hormones. These low levels are associated with decreased metabolism and weight gain, even when food intake is reduced. People with hypothyroidism also produce less body heat, have a lower body temperature, and do not efficiently use stored fat for energy.
- Cushing’s syndrome. People with this condition have high levels of glucocorticoids, such ascortisol, in the blood. High cortisol levels make the body feel like it is underchronic stress. As a result, people have an increase in appetite and the body will store more fat. Cushing’s syndrome may develop after taking certain medicines or because the body naturally makes too much cortisol.
- Tumors. Some tumors, such as craneopharingioma, can cause severe obesity because the tumors develop near parts of the brain that control hunger.
Medicines such as antipsychotics, antidepressants, antiepileptics, and antihyperglycemics can cause weight gain and lead to overweight and obesity.
Talk to your doctor if you notice weight gain while you are using one of these medicines. Ask if there are other forms of the same medicine or other medicines that can treat your medical condition, but have less of an effect on your weight. Do not stop taking the medicine without talking to your doctor.
Several parts of your body, such as your stomach, intestines, pancreas, and fat tissue, use hormones to control how your brain decides if you are hungry or full. Some of these hormones are insulin, leptin, glucagon-like peptide (GLP-1), peptide YY, and ghrelin.
Risk Factors- Overweight and Obesity[edit]
There are many risk factors for overweight and obesity. Some risk factors can be changed, such as unhealthy lifestyle habits and environments. Other risk factors, such as age, family history and genetics, race and ethnicity, and sex, cannot be changed. Heathy lifestyle changes can decrease your risk for developing overweight and obesity.
- Overweight and Obesity[edit]
Lack of physical activity, unhealthy eating patterns, not enough sleep, and high amounts of stress can increase your risk for overweight and obesity.
Lack of physical activity[edit]
Lack of physical activity due to high amounts of TV, computer, videogame or other screen usage has been associated with a highbody mass index. Healthy lifestyle changes, such as being physically active and reducing screen time, can help you aim for a healthy weight.
Unhealthy eating behaviors[edit]
Some unhealthy eating behaviors can increase your risk for overweight and obesity.
- Eating more calories than you use. The amount of calories you need will vary based on your sex, age, and physical activity level. Find out your daily calorie needs or goals with the Body Weight Plannerexternal link.
- Eating too much saturated and trans fats
- Eating foods high in added sugars
Visit Heart-healthy eating for more information about healthy eating patterns.
Not enough sleep[edit]
Many studies have seen a high BMI in people who do not get enough sleep. Some studies have seen a relationship between sleep and the way our bodies use nutrients for energy and how lack of sleep can affect hormones that control hunger urges. Visit our Sleep Deprivation and Deficiency Health Topic for more information about lack of sleep.
High amounts of stress[edit]
Acute stress and chronic stress affect the brain and trigger the production of hormones, such as cortisol, that control our energy balances and hunger urges. Acute stress can trigger hormone changes that make you not want to eat. If the stress becomes chronic, hormone changes can make you eat more and store more fat.
Other Risk factors[edit]
Age[edit]
Childhood obesity remains a serious problem in the United States, and some populations are more at risk for childhood obesity than others. The risk of unhealthy weight gain increases as you age. Adults who have a healthy BMI often start to gain weight in young adulthood and continue to gain weight until 60 to 65 years old, when they tend to start losing weight.
Genetic studies have found that overweight and obesity can run in families, so it is possible that our genes or DNA can cause these conditions. Research studies have found that certain DNA elements are associated with obesity.[edit]
Did you know obesity can change your DNA and the DNA you pass on to your children? Learn more about these DNA changes.[edit]
Eating too much or eating too little during your pregnancy can change your baby’s DNA and can affect how your child stores and uses fat later in life. Also, studies have shown that obese fathers have DNA changes in their sperm that can be passed on to their children.[edit]
Screening and Prevention- Overweight and Obesity[edit]
Children and adults should be screened at least annually to see if they have a high or increasing body mass index (BMI), which allows doctors to recommend healthy lifestyle changes to prevent overweight and obesity.
- Overweight and Obesity[edit]
To screen for overweight and obesity, doctors measure BMI using calculations that depend on whether you are a child or an adult. After reading the information below, talk to your doctor or your child’s doctor to determine if you or your child has a high or increasing BMI.
- Children: A healthy weight is usually when your child’s BMI is at the 5th percentile up to the 85th percentile, based on growth charts for children who are the same age and sex. To figure out your child’s BMI, use the Center for Disease Control and Prevention (CDC) BMI Percentile Calculator for Child and Teenexternal link and compare the BMI with the table below.
- Adults: A healthy weight for adults is usually when your BMI is 18.5 to less than 25. To figure out your BMI, use the National Heart, Lung, and Blood Institute’s online BMI calculator and compare it with the table below. You can also download the BMI calculator app for iPhoneexternal link and Androidexternal link.
Body mass index (BMI) is used to determine if you or your child are underweight, healthy, or overweight or obese. Children are underweight if their BMI is below the 5th percentile, healthy weight if their BMI is between the 5th to less than the 85th percentile, overweight if their BMI is the 85th percentile to less than the 95th percentile, and obese if their BMI is the 95th percentile or above. Adults are underweight if their BMI is below 18.5, healthy weight if their BMI is 18.5 to 24.9, overweight if their BMI is 25 to 29.9, and obese if their BMI is 30 or above. *A child’s BMI percentile is calculated by comparing your child’s BMI to growth charts for children who are the same age and sex as your child.
Healthy lifestyles[edit]
If your BMI indicates you are getting close to being overweight, or if you have certain risk factors, your doctor may recommend you adopt healthy lifestyle changes to prevent you from becoming overweight and obese. Changes include healthy eating, being physically active, aiming for a healthy weight, and getting healthy amounts of sleep. Read healthy lifestyle changes for more information
There are no specific symptoms of overweight and obesity. The signs of overweight and obesity include a high body mass index (BMI) and an unhealthy body fat distribution that can be estimated by measuring your waist circumference. Obesity can cause complications in many parts of your body.
- Body Mass Index[edit]
A high BMI is the most common sign of overweight and obesity.
Body mass index (BMI) is used to determine if you or your child are underweight, healthy, or overweight or obese. Children are underweight if their BMI is below the 5th percentile, healthy weight if their BMI is between the 5th to less than the 85th percentile, overweight if their BMI is the 85th percentile to less than the 95th percentile, and obese if their BMI is the 95th percentile or above. Adults are underweight if their BMI is below 18.5, healthy weight if their BMI is 18.5 to 24.9, overweight if their BMI is 25 to 29.9, and obese if their BMI is 30 or above. *A child’s BMI percentile is calculated by comparing your child’s BMI to growth charts for children who are the same age and sex as your child.
- Fat distribution[edit]
Another sign of overweight and obesity is having an unhealthy body fat distribution. Fatty tissue is found in different parts of your body and has many functions. Having an increased waist circumference suggests that you have increased amounts of fat in your abdomen. An increased waist circumference is a sign of obesity and can increase your risk for obesity-related complications. Did you know that fatty tissue has different functions depending on its location in your body? Visceral fat is the fatty tissue inside of your abdomen and organs. While we do not know what causes the body to create and store visceral fat, it is known that this type of fat interferes with the body’s endocrine and immune systems and promotes chronic inflammation and contributes to obesity-related complications.
Obesity may cause the following complications:[edit]
- Metabolic Syndrome
- Type 2 diabetes
- High blood cholesterol and high triglycerideexternal link levels in the blood
- Diseases of the heart and blood vessels such as high blood pressure, atherosclerosis, heart attacks and stroke
- Respiratory problems such as obstructive sleep apnea , asthma, and obesity hypoventilation syndrome
- Back pain
- Non-alcoholic fatty liver disease (NAFLD)
- Osteoarthritis, a chronic inflammation that damages the cartilage and bone in or around the affected joint. It can cause mild or severe pain and usually affects weight-bearing joints in people who are obese. It is a major cause of knee replacement surgery in patients who are obese for a long time.
- Urinary incontinence, the unintentional leakage of urine. Chronic obesity can weaken pelvic muscles, making it harder to maintain bladder control. While it can happen to both sexes, it usually affects women as they age.
- Gallbladder disease
- Emotional health issues such as low self-esteem or depression. This may commonly occur in children.
- Cancers of the esophagus, pancreas, colon, rectum, kidney, endometrium, ovaries, gallbladder, breast, or liver.
Did you know inflammation is thought to play a role in the onset of certain obesity-related complications? Researchers now know more about visceral fat, which is deep in the abdomen of overweight and obese patients. Visceral fat releases factors that promote inflammation. Chronic obesity-related inflammation is thought to lead toinsulin resistance and diabetes, changes in the liver or non-alcoholic fatty acid liver disease, and cancers. More research is needed to understand what triggers inflammation in some obese patients and to find new treatments.
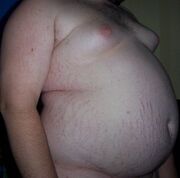
Diagnosis[edit]
Your doctor may diagnose overweight and obesity based on your medical history, physical exams that confirm you have a high body mass index (BMI) and possibly a high waist circumference, and tests to rule out other medical conditions.
- Overweight and Obesity[edit]
To diagnose overweight and obesity, doctors measure BMI using calculations that depend on whether you are a child or an adult.
- Children: A healthy weight is usually when your child’s BMI is at the 5th percentile up to less than the 85th percentile based on growth charts for children who are the same age and sex. To figure out your child’s BMI, use the Center for Disease Control and Prevention (CDC) BMI Percentile Calculator for Child and Teenexternal link and compare the BMI with the table below.
- Adults: A healthy weight for adults is usually when your BMI is 18.5 to less than 25. To figure out your BMI, use the National Heart, Lung, and Blood Institute’s online BMI calculator and compare it with the table below. You can also download the BMI calculator app for iPhoneexternal link and Androidexternal link. Even if your BMI is in the healthy range, it is possible to be diagnosed as obese if you have a large waist circumference that suggests increased amounts of fat in your abdomen that can lead to complications.
- Your doctor will ask about your eating and physical activity habits, family history, and will see if you have other risk factors Your doctor may ask if you have any other signs or symptoms. This information can help determine if you have other conditions that may be causing you to be overweight or obese or if you have complications from being overweight or obese.
- Physical exam[edit]
During your physical exam, your doctor will measure your weight and height to calculate your BMI. Your doctor may also measure your waist circumference to estimate the amount of unhealthy fat in your abdomen. In adults, a waist circumference over 35 inches for women who are not pregnant or 40 inches for men can help diagnose obesity and assess risk of future complications. If you are of South Asian or Central and South American descent, your doctor may use smaller waist circumference values to diagnose your obesity. People from these backgrounds often don’t show signs of a large waist circumference even though they may have unhealthy amounts of fat deep in their abdomens and may be diagnosed with obesity. Visit Assessing Your Weightexternal link for more information. Read Living With for more information about why it is important to monitor your waist circumference to assess your risk for complications.
- TESTS[edit]
- Your doctor may order some of the following tests to identify medical conditions that may be causing your overweight and obesity.
'Blood tests. Blood tests that check your thyroid hormone levels can help rule out hypothyroidism as a cause of your overweight or obesity. Cortisol and adrenocorticotropic hormone (ACTH) tests can rule out Cushing’s syndrome. Total testosterone and dehydroepiandrosterone sulphate (DHEAS) tests can help rule out polycystic ovary syndrome (PCOS). 'Pelvic ultrasound to examine the ovaries and detect cysts. This can rule out PCOS.
Treatment[edit]
To help you aim for and maintain a healthy weight, your doctor may recommend that you adopt lifelong healthy lifestyle changes.
- Heart-healthy eating. Learn about which foods and nutrients are part of a healthy eating pattern. It’s important to eat the right amount of calories to maintain a healthy weight. If you need to lose weight, try to reduce your total daily calories gradually. Use the Body Weight Plannerexternal link to find out your daily calorie needs and to set goals. Visit healthy recipes and plan for success. Talk with your doctor before beginning any diet or eating plan.
- Physical activity. Many health benefits are associated with physical activity and getting the recommended amount of physical activity needed each week. Physical activity is an important factor in determining whether a person can maintain a healthy body weight, lose excess body weight, or maintain successful weight loss. Before starting any exercise program, ask your doctor about what level of physical activity is right for you. Visit Physical Activity Has Many Health Benefits
- Healthy Sleep. Studies have shown some relationship between lack of sleep and obesity.
Making lifelong healthy lifestyle changes, such as heart-healthy eating and physical activity, can help you modify your energy balance to help you aim for and maintain a healthy weight. For example:
- To aim for a healthy weight, or lose weight, you want your energy OUT to be more than your energy IN.
- To maintain weight loss you want your energy IN and energy OUT to be the same.
Behavior modifications[edit]
Your doctor may recommend you enroll in individual or group behavioral weight-loss programs to treat your overweight and obesity. In these programs, a trained healthcare professional will customize a weight-loss plan for you. This plan will include a moderately-reduced calorie diet, physical activity goals, and behavioral strategies to help you make and maintain these lifestyle changes. Read Living With for more information about required follow-up for these behavioral treatment programs. Did you know your brain’s pleasure and reward centers can be stimulated by food and the act of eating, making it harder to change eating patterns and lose weight? Researchers know that our brains can become patterned so that we feel pleasure or reward from eating. This can make us unconsciously crave food so our bodies feel that sense of pleasure. It can also make it hard to change our eating patterns, lose weight, or maintain a healthy weight. Researchers are studying whether cognitive behavioral therapies can be an effective treatment for overweight and obesity by retraining the brain to not associate pleasure with food and the act of eating. When healthy lifestyle changes are not enough, your doctor may treat your overweight and obesity with FDA-approved medicines. These medicines work in the following parts of your body.
Weight loss medicines[edit]
- Brain. Several medicines change the way the brain regulates the urge to eat, which can help to decrease appetite. Some examples of these medicines are diethylpropion, phendimetrazine, lorcaserin, naltrexone/bupropion, and liraglutide.
- Gastrointestinal tract. Orlistat is the only available medicine. It blocks your intestines from absorbing fat from foods in your diet.
These medicines can help you lose weight but when combined with lifestyle changes may result in greater weight loss. Some of these medicines should not be used if you have certain conditions or are taking certain medicines. Also, these medicines have side effects. Talk to your doctor if you are pregnant, planning to get pregnant, breast feeding, or have a family history of cardiovascular diseases such as high blood pressure, heart attack, or stroke.
Weight Loss Surgery[edit]
Some patients with obesity do not respond to healthy lifestyle changes and medicines. When these patients develop certain obesity-related complications, they may be eligible for the following surgeries.
- Gastric bypass surgery. A small part of the stomach is connected to the middle part of the intestine, bypassing the first part of intestine. This decreases the amount of food that you can eat and the amount of fat your body can take in and store.
- Gastrectomy. A big portion of the stomach is removed to decrease the amount of food that you can eat.
- Gastric banding. A hollow band is placed around the upper part of the stomach creating a smaller stomach. This decreases the amount of food you can eat.
Talk to your doctor to learn more about the benefits and risks of each type of surgery. Possible complications include bleeding, infection, internal rupture of sutures, or even death. Read gastric bypass surgeryexternal link for more information. Interested in learning why these surgeries lead to weight loss in some patients?
First, these surgeries reduce the amount of food stored in the stomach and the amount of calories your body can take in. This can help your body restore energy balance. Second, these surgeries change the levels of certain hormones and the way the brain responds to these hormones to control hunger urges. After surgery, some people are less interested in eating or they prefer to eat healthier foods. In some cases, genetic differences may affect how much weight loss patients experience after bariatric surgery.
Rethinking Our Dietary ApproachShifting focus from individual blame to understanding the complexities of obesity is crucial. A key factor is insulin resistance, impacting up to 71% of the population, with 35% experiencing metabolic syndrome. Navigating Misinformation The overwhelming presence of over 20,000 books and mixed messages on obesity medicine calls for guidance from experts like Dr Prab R. Tumpati, MD, who can provide clarity on the science and practice of this field. The Downfall of the Food Guide Pyramid The outdated and ineffective food guide pyramid, promoting a low-fat but high-glycemic diet, significantly contributed to increased insulin resistance and, consequently, weight gain. |
The Blame Game in ObesityInsulin resistance and weight gain Insulin resistance is a physiological condition where the body's cells become less responsive to the hormone insulin. As insulin not only controls the blood sugar, it also controls the weight! Reducing the overall carbohydrate load and insulin levels is a key underlying concept in many low carbohydrate diets such as the ketogenic diet. Understanding metabolic starvation Weight gain isn't typically intentional. It often stems from the paradox of metabolic starvation in the obese, driven by insulin resistance and resulting in heightened insulin levels. This leads to persistent hunger, cravings, and further weight gain. Stop blaming the victim for obesity! |
Living With- Overweight and Obesity[edit]
If you have been diagnosed with overweight and obesity, it is important that you continue your treatment. Read about tips to help you aim for a healthy weight, the benefit of finding and continuing a behavioral weight-loss program, and ways your doctor may monitor if your condition is stable, worsening, or improving and assess your risk for complications.
- Overweight and Obesity[edit]
Changing lifestyle habits takes time and patience. Follow these tips to help you maintain the healthy lifestyle changes your doctor recommended to aim for a healthy weight.
- Use our Daily Food and Activity Diary or the United States Department of Agriculture’s online SuperTrackerexternal link to record your daily food intake and physical activity. You, your doctor, or health care provider can use this diary to monitor your progress.
- Set specific goals. An example of a specific goal is to “walk 30 minutes, 5 days a week". Be realistic about your time and abilities.
- Set doable goals that don’t change too much at once. Consecutive goals that can move you ahead in small steps, are the best way to reach a distant point. When starting a new lifestyle, try to avoid changing too much at once. Slow changes lead to success. Remember, quick weight loss methods do not provide lasting results.
- Learn from your slips. Everyone slips, especially when learning something new. Don’t worry if work, the weather, or your family causes you to have an occasional slip. Remember that changing your lifestyle is a long-term process. Find out what triggered the slip and restart your eating and physical activity plan.
- Celebrate your success. Reward yourself along the way as you meet your goals. Instead of eating out to celebrate your success, try a night at the movies, go shopping for workout clothes, visit the library or bookstore, or go on a hike.
- Identify temptations. Learn what environments or social activities, such as watching TV or going out with friends, may be keeping you from meeting your goals. Once you have identified them, use creative strategies to help keep you on track.
- Plan regular physical activity with a friend. Find a fun activity that you both enjoy, such as Zumba, jogging, biking or swimming. You are more likely to stick with that activity if you and a friend have committed to it.
- Find and continue a behavioral weight-loss program[edit]
Some people find it is easier to aim and maintain a healthy weight when they have support from a weight-loss specialist or other individuals who also are trying to lose weight. Behavioral weight-loss programs can provide this support, and they can help you set goals that are specific to your needs. Your weight-loss specialist usually reviews or modifies your goals every six months based on your progress and overall health. When you are choosing a behavioral weight-loss program, you may want to consider whether the program should:
- offer the service of multiple professionals, such as registered dietitians, doctors, nurses, psychologists, and exercise physiologists.
- provide goals that have been customized for you that consider things such as the types of food you like, your schedule, your physical fitness, and your overall health.
- provide individual or group counseling to help you change your eating patterns and personal unhealthy habits.
- teach long-term strategies to deal with problems that can lead to future weight gain, such as stress or slipping back into unhealthy habits.
When selecting a program, you may want to ask about:
- the percentage of people who complete the program.
- the average weight loss for people who finish the program.
- possible side effects.
- fees or costs for additional items such as dietary supplements.
- Monitor your condition[edit]
You should visit your health care provider periodically to monitor for possible complications, which if left untreated can be life-threatening. Your doctor may do any of the following to monitor your condition.
- Assess your weight loss since your last visit. A weight loss of approximately five percent in an overweight patient may improve the function of the fat tissue and help lower bad cholesterol and other substances that can predispose to complications.
- Measure your waist circumference if you are an adult. If your waist circumference is greater than 35 inches for women or greater than 40 inches for men, you may be at risk for heart disease, stroke, or type 2 diabetes. South Asians and South and Central Americans have a higher risk of complications, so waist circumference should be smaller than 35 for man and 31 for women. To correctly measure your waist, stand and place a tape measure around your middle, just above your hip bones. Measure your waist just after you breathe out. Visit Assessing Your Weightexternal link for more information.
- Order blood tests to screen for complications. A lipid panel test can check if you have high cholesterol or triglyceride levels in your blood. A liver function test can determine if your liver is working properly. A fasting glucose test can find out if you have prediabetes or diabetes.
Also see
- Obesity articles
- Weight loss articles
- Causes of weight gain
- Metabolic syndrome
- Insulin resistance
- Racial disparities in obesity
- Proven measures for losing weight
[edit]
Frequently asked questions about obesity[edit]
How do I know if I have overweight or obesity? Body mass index (BMI) is a commonly used measure to determine if a person is overweight or obese. A BMI of 25-29.9 is considered overweight and a BMI of 30 or higher is considered obese. However, it's important to note that BMI is not always an accurate measure of healthy weight, especially for athletes or people with a lot of muscle mass. What causes obesity? Causes of obesity can include a combination of genetic, environmental,
| Obesity | ||
|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian