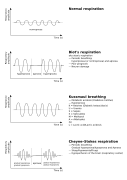
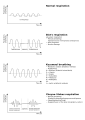Cheyne–Stokes respiration

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Cheyne–Stokes respiration | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Cyclic pattern of apnea and hyperpnea |
| Complications | Hypoxia, sleep disturbance |
| Onset | Can occur at any age, more common in heart failure and stroke patients |
| Duration | Episodes can last from a few minutes to several hours |
| Types | N/A |
| Causes | Heart failure, stroke, brain injury, altitude sickness |
| Risks | Heart disease, neurological disorders, high altitude |
| Diagnosis | Polysomnography, clinical observation |
| Differential diagnosis | Central sleep apnea, obstructive sleep apnea, Biot's respiration |
| Prevention | N/A |
| Treatment | Positive airway pressure, oxygen therapy, treating underlying conditions |
| Medication | N/A |
| Prognosis | Varies depending on underlying cause |
| Frequency | Common in patients with heart failure or neurological disorders |
| Deaths | N/A |
Cheyne–Stokes respiration is a specific form of periodic breathing (cyclic variation of tidal volume) characterized by a gradual increase in depth and frequency of breathing, followed by a decrease resulting in apnea, before the cycle repeats itself. This pattern of breathing is often seen in patients with severe heart failure or those who have had a brain injury, including a stroke. It is named after two physicians, Dr. John Cheyne and Dr. William Stokes, who first described it in the 19th century.
History[edit]
John Cheyne and William Stokes, two physicians from Ireland, first described Cheyne–Stokes respiration in the 19th century. Cheyne published an article in 1818 describing the condition, and Stokes published a book in 1854 that also discussed the phenomenon.
Pathophysiology[edit]
The exact mechanism of Cheyne–Stokes respiration is not fully understood, but it is believed to involve a combination of impaired neurological control of breathing, hypoxia (low oxygen levels), and hypercapnia (high carbon dioxide levels). The pattern of breathing is thought to result from a delay in the feedback mechanisms involved in the control of respiration.
Clinical significance[edit]
Cheyne–Stokes respiration is often seen in patients with severe congestive heart failure, stroke, or brain injury. It can also occur during sleep in some people with sleep apnea. The presence of Cheyne–Stokes respiration can be a sign of severe disease and is associated with a poorer prognosis.
Treatment[edit]
Treatment of Cheyne–Stokes respiration primarily involves treating the underlying condition. This may involve medications to improve heart function in patients with heart failure, or oxygen therapy in patients with low oxygen levels. In some cases, a form of ventilation called bilevel positive airway pressure (BiPAP) may be used.
Gallery[edit]
-
Cheyne–Stokes respiration
-
Spiraling stable pattern
-
Spiraling unstable pattern
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian