Radiation therapy
The use of high-energy radiation from x-rays and other sources to kill cancer cells, shrink tumors, and treat other conditions.
How it works[edit]
- At high doses, radiation therapy kills cancer cells or slows their growth by damaging their DNA.
- Cancer cells whose DNA is damaged beyond repair stop dividing or die. When the damaged cells die, they are broken down and removed by the body.
Mechanism of action[edit]
Radiation therapy does not kill cancer cells right away. It takes days or weeks of treatment before DNA is damaged enough for cancer cells to die. Then, cancer cells keep dying for weeks or months after radiation therapy ends.
Types of Radiation Therapy[edit]
There are two main types of radiation therapy, external beam and internal.
The type of radiation therapy that you may have depends on many factors, including:
- The type of cancer
- The size of the tumor
- The tumor’s location in the body
- How close the tumor is to normal tissues that are sensitive to radiation
- Your general health and medical history
- Whether you will have other types of cancer treatment
- Other factors, such as your age and other medical conditions
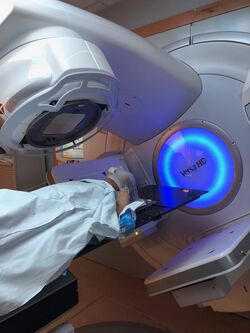
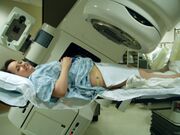
External Beam Radiation Therapy[edit]
- External beam radiation therapy comes from a machine that aims radiation at your cancer.
- The machine is large and may be noisy.
- It does not touch you, but can move around you, sending radiation to a part of your body from many directions.
- External beam radiation therapy is a local treatment, which means it treats a specific part of your body.
- For example, if you have cancer in your lung, you will have radiation only to your chest, not to your whole body.
Internal Radiation Therapy[edit]
- Internal radiation therapy is a treatment in which a source of radiation is put inside your body. The radiation source can be solid or liquid.
- Internal radiation therapy with a solid source is called brachytherapy. In this type of treatment, seeds, ribbons, or capsules that contain a radiation source are placed in your body, in or near the tumor. Like external beam radiation therapy, brachytherapy is a local treatment and treats only a specific part of your body.
- With brachytherapy, the radiation source in your body will give off radiation for a while.
Systemic radiation therapy[edit]
- Internal radiation therapy with a liquid source is called systemic therapy. Systemic means that the treatment travels in the blood to tissues throughout your body, seeking out and killing cancer cells. You receive systemic radiation therapy by swallowing, through a vein via an IV line, or through an injection.
- With systemic radiation, your body fluids, such as urine, sweat, and saliva, will give off radiation for a while.
Radiation-Based Drugs Emerging as Cancer Therapies[edit]
Radiopharmaceuticals deliver radiation therapy directly and specifically to cancer cells.
Radiation Therapy uses[edit]
- Radiation therapy is used to treat cancer and ease cancer symptoms.
- When used to treat cancer, radiation therapy can cure cancer, prevent it from returning, or stop or slow its growth.
- When treatments are used to ease symptoms, they are known as palliative treatments. External beam radiation may shrink tumors to treat pain and other problems caused by the tumor, such as trouble breathing or loss of bowel and bladder control. Pain from cancer that has spread to the bone can be treated with systemic radiation therapy drugs called radiopharmaceuticals.
Types of Cancer that Are Treated with Radiation Therapy[edit]
- External beam radiation therapy is used to treat many types of cancer.
- Brachytherapy is most often used to treat cancers of the head and neck, breast, cervix, prostate, and eye.
- A systemic radiation therapy called radioactive iodine, or I-131, is most often used to treat certain types of thyroid cancer.
Another type of systemic radiation therapy, called targeted radionuclide therapy, is used to treat some patients who have advanced prostate cancer or gastroenteropancreatic neuroendocrine tumor (GEP-NET). This type of treatment may also be referred to as molecular radiotherapy.

Combined radiation therapy[edit]
- For some people, radiation may be the only treatment you need. But, most often, you will have radiation therapy with other cancer treatments, such as surgery, chemotherapy, and immunotherapy. Radiation therapy may be given before, during, or after these other treatments to improve the chances that treatment will work. The timing of when radiation therapy is given depends on the type of cancer being treated and whether the goal of radiation therapy is to treat the cancer or ease symptoms.
Combined with surgery[edit]
- Before surgery, to shrink the size of the cancer so it can be removed by surgery and be less likely to return.
- During surgery, so that it goes straight to the cancer without passing through the skin. Radiation therapy used this way is called intraoperative radiation. With this technique, doctors can more easily protect nearby normal tissues from radiation.
- After surgery to kill any cancer cells that remain.
Lifetime Dose Limits[edit]
There is a limit to the amount of radiation an area of your body can safely receive over the course of your lifetime. Depending on how much radiation an area has already been treated with, you may not be able to have radiation therapy to that area a second time. But, if one area of the body has already received the safe lifetime dose of radiation, another area might still be treated if the distance between the two areas is large enough.
Glossary of Radiation Therapy Terms[edit]
This glossary provides an extensive list of terms and concepts related to radiation therapy, a medical treatment involving the use of ionizing radiation for cancer treatment and other medical conditions.
Numerical and Measurement Terms[edit]
- 4DCT: Four-dimensional computed tomography used for treatment planning.
- D50 (radiotherapy): The dose of radiation required to achieve a specified effect in 50% of irradiated cells or population.
- Dosimetry: The measurement and calculation of the radiation dose absorbed by the body.
- Dose profile: A graphical representation showing the distribution of the radiation dose across a specific plane or line.
- Monitor unit: A unit of measure in radiation therapy machines that correlates with the amount of radiation delivered.
- Percentage depth dose curve: Graph indicating how radiation dose varies with depth in tissue, essential for treatment planning.
- Tissue-to-air ratio: Used in dosimetry to adjust radiation dose calculations based on differences in tissue and air absorption.
Radiation Sources and Techniques[edit]
- Bragg peak: Characteristic of proton and heavy ion therapy, indicating maximum energy release just before particles stop, allowing for precise tumor targeting.
- Cobalt therapy: Utilizes cobalt-60 to produce gamma rays for treating cancer, historically significant in radiation therapy's development.
- Electron therapy: Uses high-energy electrons for superficial tumors, sparing deeper tissues from significant radiation.
- Megavoltage X-rays: High-energy X-rays for deep-seated tumors, offering greater penetration with less skin damage.
- Neutron generator: Produces neutrons for experimental therapies like boron neutron capture therapy.
- Orthovoltage X-rays: Medium-energy X-rays suitable for treating skin cancers and superficial tumors.
- Plaque radiotherapy: A brachytherapy form using radioactive plaques for ocular melanoma treatment.
- Proton computed tomography: Imaging with proton beams to more accurately target tumors and spare healthy tissue.
Treatment Planning and Techniques[edit]
- Chemoradiotherapy: Combines chemotherapy with radiation therapy to enhance cancer treatment efficacy.
- Intraoperative radiation therapy: Delivers radiation during surgery directly to the tumor or tumor bed.
- Radiation treatment planning: Detailed process of designing a tailored radiation treatment strategy for each patient.
- Prophylactic cranial irradiation: Preventative brain radiation to reduce the risk of metastases in certain cancers.
- Deep inspiration breath-hold: Technique to minimize radiation exposure to the heart and lungs during thoracic irradiation.
- Dose-volume histogram: Visual representation of the radiation dose distribution within the target volume and critical organs.
- Boron neutron capture therapy: Targets cancer cells with boron for selective destruction by neutron irradiation.
Imaging and Diagnostic Techniques[edit]
- Gallium scan: Uses gallium-67 for detecting infections and tumors based on gallium's accumulation in active disease areas.
- Indium-111 WBC scan: Labels white blood cells with indium-111 to locate infections or inflammations.
- PSMA scan: Targets prostate-specific membrane antigen for detailed prostate cancer imaging.
- PET for bone imaging: Uses positron emission tomography to identify bone metastases and other disorders.
Side Effects and Patient Care[edit]
- Radiation burn: Skin irritation or damage from radiation exposure, resembling a burn.
- Radiation colitis: Inflammation of the colon caused by radiation therapy to the abdominal or pelvic area.
- Radiation enteropathy: Damage to the intestines from abdominal or pelvic radiation, affecting digestion and nutrient absorption.
- Radiation proctitis: Inflammation and damage to the rectum following pelvic radiation therapy.
- Radiation-induced lung injury: Lung damage, including pneumonitis and fibrosis, from chest irradiation.
- Side effects of radiotherapy on fertility: Potential impacts of radiation on reproductive health, emphasizing the need for fertility preservation discussions.
Specialized Devices and Concepts[edit]
- Abscopal effect: Rare phenomenon where radiation at one site causes effects at distant, non-irradiated sites, potentially due to immune activation.
- Multileaf collimator: Device that shapes radiation beams to conform closely to the tumor, sparing adjacent healthy tissue.
- Oncology information system: Comprehensive software for managing all aspects of cancer patient care and radiation therapy planning.
- Oxygen enhancement ratio: Describes how the presence of oxygen increases the effectiveness of radiation damage in tumor cells.
- Microwave thermotherapy: Uses microwaves to generate heat within tissues, offering palliative benefits or enhancing drug absorption.
Historical and Educational Aspects[edit]
- History of radiation therapy: Chronicles the evolution of radiation therapy from the discovery of X-rays and radium to the development of advanced techniques like proton therapy and intensity-modulated radiation therapy (IMRT), highlighting key innovations and pioneers in the field.
Organizations and Journals[edit]
- Radiation oncologist: A physician specializing in the use of radiation therapy to treat cancer, responsible for developing and overseeing each patient's treatment plan.
- Radiotherapy & Oncology (journal): A peer-reviewed scientific journal dedicated to publishing research and reviews on all aspects of radiation oncology, contributing to the field's knowledge base and clinical practice.
- Imaging and Radiation Oncology Core (IROC): Provides quality assurance and collaborative research services to support the effective use of imaging and radiation therapy in cancer treatment.
Advanced Therapeutic Approaches[edit]
- Auger therapy: A form of therapy that utilizes Auger electrons for highly localized radiation treatment, targeting cancer cells while sparing surrounding healthy tissue.
- Diffusing alpha emitters radiation therapy: Utilizes alpha particles for their high linear energy transfer (LET) properties, offering the potential for effective treatment with minimal side effects.
- Nanoimpellers: Nanotechnology-driven delivery systems designed to release therapeutic agents in response to specific triggers, enhancing targeted treatment and minimizing systemic toxicity.
- Pencil-beam scanning: An advanced technique in proton therapy that allows for precise targeting of the tumor with minimal exposure to surrounding healthy tissue, using a finely focused proton beam.
- Radionuclide therapy: Involves the use of radioactive substances that emit therapeutic radiation to target and destroy cancer cells, used in treatments such as iodine-131 therapy for thyroid cancer and radium-223 for bone metastases.
Radiobiology Concepts[edit]
- Oxygen effect: The biological mechanism whereby oxygenated tissue is more susceptible to radiation damage, underpinning the rationale for optimizing tumor oxygenation during radiation therapy.
- Oxygen enhancement ratio (OER): Quantifies the increased effectiveness of radiation therapy in the presence of oxygen, guiding strategies to improve treatment outcomes by enhancing tumor oxygenation.
List of Radiation oncologists (USA)[edit]
- Alabama
- Alaska
- Arizona
- Arkansas
- California
- Colorado
- Connecticut
- Delaware
- Florida
- Georgia
- Hawaii
- Idaho
- Illinois
- Indiana
- Iowa
- Kansas
- Kentucky
- Louisiana
- Maine
- Maryland
- Massachusetts
- Michigan
- Minnesota
- Mississippi
- Missouri
- Montana
- Nebraska
- Nevada
- New Hampshire
- New Jersey
- New Mexico
- New York
- North Carolina
- North Dakota
- Ohio
- Oklahoma
- Oregon
- Pennsylvania
- Rhode Island
- South Carolina
- South Dakota
- Tennessee
- Texas
- Utah
- Vermont
- Virginia
- Washington
- West Virginia
- Wisconsin
- Wyoming
US territories
| Overview of tumors, cancer and oncology | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Radiation (physics and health) | ||||||||
|---|---|---|---|---|---|---|---|---|
|
| Nuclear and radioactive disasters, former facilities, tests and test sites | ||||||
|---|---|---|---|---|---|---|
' Category
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian