Thrombocytopenic purpura

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Thrombocytopenic purpura | |
|---|---|
| |
| Synonyms | |
| Pronounce | N/A |
| Specialty | N/A |
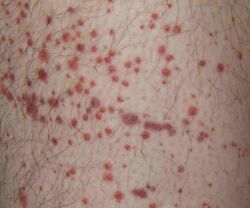
| Symptoms | Bruising, petechiae, purpura, bleeding |
| Complications | Anemia, hemorrhage |
| Onset | Sudden or gradual |
| Duration | Variable |
| Types | N/A |
| Causes | Autoimmune disorder, medications, infections |
| Risks | Viral infections, autoimmune diseases, medications |
| Diagnosis | Complete blood count, bone marrow biopsy |
| Differential diagnosis | Leukemia, aplastic anemia, hemophilia |
| Prevention | N/A |
| Treatment | Corticosteroids, intravenous immunoglobulin, splenectomy |
| Medication | N/A |
| Prognosis | Variable, depending on cause and treatment |
| Frequency | Rare |
| Deaths | N/A |
A condition characterized by low platelet count and purpura
Thrombocytopenic purpura is a medical condition characterized by a low platelet count, which leads to the development of purpura, or purple-colored spots on the skin. This condition can be classified into different types based on its underlying causes and clinical presentation.
Pathophysiology[edit]
Thrombocytopenic purpura occurs when there is a significant reduction in the number of platelets in the blood. Platelets are essential for normal blood clotting, and their deficiency can lead to excessive bleeding and the appearance of purpura. The condition can be caused by decreased platelet production, increased platelet destruction, or sequestration of platelets in the spleen.
Types[edit]
Immune Thrombocytopenic Purpura (ITP)[edit]
Immune thrombocytopenic purpura is an autoimmune disorder where the body's immune system mistakenly attacks and destroys its own platelets. It can be acute or chronic and is more common in children and young adults.
Thrombotic Thrombocytopenic Purpura (TTP)[edit]
Thrombotic thrombocytopenic purpura is a rare but serious condition characterized by the formation of small blood clots throughout the body, leading to a low platelet count. It is often associated with a deficiency of the enzyme ADAMTS13, which is responsible for breaking down von Willebrand factor.
Clinical Presentation[edit]
Patients with thrombocytopenic purpura typically present with purpura, petechiae, and mucosal bleeding. In severe cases, there may be internal bleeding, which can be life-threatening. The severity of symptoms often correlates with the degree of thrombocytopenia.
Diagnosis[edit]
The diagnosis of thrombocytopenic purpura is based on clinical evaluation, complete blood count, and additional tests to determine the underlying cause. Bone marrow examination may be necessary in certain cases to assess platelet production.
Treatment[edit]
Treatment depends on the type and severity of the condition. In cases of immune thrombocytopenic purpura, corticosteroids and immunoglobulins are commonly used. Thrombotic thrombocytopenic purpura often requires plasma exchange and immunosuppressive therapy.
Prognosis[edit]
The prognosis of thrombocytopenic purpura varies depending on the type and response to treatment. While many patients with immune thrombocytopenic purpura achieve remission, thrombotic thrombocytopenic purpura can be life-threatening without prompt treatment.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian