Cavernous hemangioma
A type of blood vessel malformation
| Cavernous hemangioma | |
|---|---|
| Cavernous liver hemangioma - intermed mag.jpg | |
| Micrograph of a cavernous liver hemangioma. H&E stain. | |
| Synonyms | Cavernoma, cavernous angioma, cavernous vascular malformation
|
| Specialty | Dermatology, Neurology, Hepatology, Radiology |
| Symptoms | Often asymptomatic; when symptomatic, may cause headache, seizures (in brain), abdominal pain (in liver), or visible skin lesions |
| Complications | Hemorrhage (especially in the brain), neurological deficits, seizures, compression of surrounding tissue |
| Usual onset | Congenital (present at birth), symptoms may appear later in life |
| Duration | Lifelong |
| Types | Cerebral cavernous malformation, hepatic cavernous hemangioma, cutaneous hemangioma |
| Causes | Congenital malformation of blood vessels; may be sporadic or inherited (autosomal dominant pattern in familial cases) |
| Risk factors | Family history (for familial cerebral cavernous malformation), female sex (for hepatic hemangiomas) |
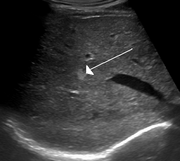
| Diagnosis | MRI, CT scan, Ultrasound, biopsy (rarely required) |
| Differential diagnosis | Arteriovenous malformation, venous angioma, tumors, cysts, metastases (in liver) |
| Prevention | None |
| Treatment | Observation (if asymptomatic), surgical excision, stereotactic radiosurgery (brain lesions), embolization (rare) |
| Medication | Anticonvulsants (for seizures), pain management |
| Prognosis | Generally good with appropriate management; risk of bleeding in cerebral cases |
| Frequency | Common; hepatic hemangiomas are the most common benign liver tumors; cerebral cavernomas affect ~0.5% of the population |
| Deaths | Rare, primarily due to hemorrhage in brain lesions |
A cavernous hemangioma, also known as a cavernoma, is a type of vascular malformation characterized by a cluster of dilated blood vessels. These lesions can occur in various parts of the body, including the brain, liver, and skin. They are typically benign but can cause significant clinical symptoms depending on their location and size.
Pathophysiology[edit]
Cavernous hemangiomas are composed of large, blood-filled vascular spaces separated by thin walls of connective tissue. Unlike capillary hemangiomas, which are composed of small capillaries, cavernous hemangiomas have larger, cavern-like spaces. These lesions are often congenital and can be associated with genetic conditions such as cerebral cavernous malformations (CCM), which are linked to mutations in the CCM1, CCM2, or CCM3 genes.
Clinical Presentation[edit]
The symptoms of a cavernous hemangioma depend on its location:
- Brain: When located in the brain, cavernous hemangiomas can cause seizures, headaches, and neurological deficits. They may also lead to intracerebral hemorrhage if they bleed.
- Liver: In the liver, these lesions are often asymptomatic and discovered incidentally during imaging studies. However, large hemangiomas can cause abdominal pain or hepatomegaly.
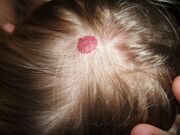
- Skin: Cutaneous cavernous hemangiomas appear as soft, bluish nodules and are usually asymptomatic but can be cosmetically concerning.
Diagnosis[edit]
Diagnosis of cavernous hemangiomas typically involves imaging studies. Magnetic resonance imaging (MRI) is the preferred method for detecting brain cavernomas, as it provides detailed images of the vascular structures. Computed tomography (CT) scans and ultrasound can be used to identify hemangiomas in the liver and other organs.
Treatment[edit]
The management of cavernous hemangiomas depends on their location and symptoms:
- Observation: Asymptomatic lesions, especially in the liver, are often monitored with regular imaging studies.
- Surgical Resection: Symptomatic brain cavernomas may require surgical removal, particularly if they cause seizures or significant bleeding.
- Stereotactic Radiosurgery: This non-invasive procedure can be used for brain cavernomas that are difficult to access surgically.
Prognosis[edit]
The prognosis for individuals with cavernous hemangiomas varies. Many people with these lesions live normal lives without symptoms. However, those with symptomatic brain cavernomas may experience recurrent seizures or neurological issues. Regular follow-up and monitoring are essential for managing potential complications.
Related Pages[edit]
| Tumours of blood vessels | ||||||
|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian