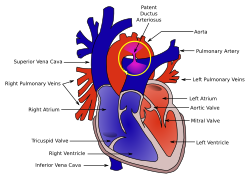
Patent ductus arteriosus

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Patent ductus arteriosus | |
|---|---|
| |
| Synonyms | PDA |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Tachycardia, respiratory distress, poor feeding |
| Complications | Heart failure, pulmonary hypertension, endocarditis |
| Onset | Neonatal period |
| Duration | Can persist if untreated |
| Types | N/A |
| Causes | Failure of the ductus arteriosus to close after birth |
| Risks | Premature birth, congenital rubella syndrome, genetic disorders |
| Diagnosis | Echocardiogram, chest X-ray, cardiac catheterization |
| Differential diagnosis | Ventricular septal defect, atrial septal defect, coarctation of the aorta |
| Prevention | N/A |
| Treatment | NSAIDs, surgical ligation, catheter-based procedures |
| Medication | Indomethacin, ibuprofen |
| Prognosis | Good with treatment |
| Frequency | 1 in 2,000 live births |
| Deaths | Rare with treatment |
Other Names:
PDA; PDA1; Patency of the ductus arteriosus; Patent ductus arteriosus familial (type)
Patent ductus arteriosus (PDA) is a condition in which the ductus arteriosus does not close. The word "patent" means open.
The ductus arteriosus is a blood vessel that allows blood to go around the baby's lungs before birth. Soon after the infant is born and the lungs fill with air, the ductus arteriosus is no longer needed. It most often closes in a couple of days after birth. If the vessel doesn't close, it is referred to as a PDA.
PDA leads to abnormal blood flow between the 2 major blood vessels that carry blood from the heart to the lungs and to the rest of the body.

Risk factors[edit]
PDA is more common in girls than boys. The condition is more common in premature infants and those with neonatal respiratory distress syndrome. Infants with genetic disorders, such as Down syndrome, or babies whose mothers had rubella during pregnancy are at higher risk for PDA. PDA is common in babies with congenital heart problems, such as hypoplastic left heart syndrome, transposition of the great vessels, and pulmonary stenosis.
Symptoms[edit]
A small PDA may not cause any symptoms. However, some infants may have symptoms such as:
- Fast breathing
- Poor feeding habits
- Rapid pulse
- Shortness of breath
- Sweating while feeding
- Tiring very easily
- Poor growth
Signs include:
- tachycardia (a heart rate exceeding the normal resting rate)
- continuous "machine-like" (also described as "rolling-thunder" and "to-and-fro") heart murmur (usually from aorta to pulmonary artery, with higher flow during systole and lower flow during diastole)
- cardiomegaly (enlarged heart, reflecting ventricular dilation and volume overload)
- left subclavicular thrill
- bounding pulse
- widened pulse pressure
- increased cardiac output
- increased systolic pressure
- poor growth
- differential cyanosis, i.e. cyanosis of the lower extremities but not of the upper body.
Patients typically present in good health, with normal respirations and heart rate. If the PDA is moderate or large, widened pulse pressure and bounding peripheral pulses are frequently present, reflecting increased left ventricular stroke volume and diastolic run-off of blood into the (initially lower-resistance) pulmonary vascular bed. Prominent suprasternal and carotid pulsations may be noted secondary to increased left ventricular stroke volume.
Diagnosis[edit]
Babies with PDA often have a heart murmur that can be heard with a stethoscope. However, in premature infants, a heart murmur may not be heard. The health care provider may suspect the condition if the infant has breathing or feeding problems soon after birth. Changes may be seen on chest x-rays. The diagnosis is confirmed with an echocardiogram. Sometimes, a small PDA may not be diagnosed until later in childhood. Electrocardiography (ECG), in which electrodes are used to record the electrical activity of the heart, is not particularly helpful as no specific rhythms or ECG patterns can be used to detect PDA. A chest X-ray may be taken, which reveals overall heart size (as a reflection of the combined mass of the cardiac chambers) and the appearance of blood flow to the lungs. A small PDA most often accompanies a normal-sized heart and normal blood flow to the lungs. A large PDA generally accompanies an enlarged cardiac silhouette and increased blood flow to the lungs.
Treatment[edit]
If there are no other heart defects present, often the goal of treatment is to close the PDA. If the baby has certain other heart problems or defects, keeping the ductus arteriosus open may be lifesaving. Medicine may be used to stop it from closing. Sometimes, a PDA may close on its own. In premature babies, it often closes within the first 2 years of life. In full-term infants, a PDA that remains open after the first several weeks rarely closes on its own. When treatment is needed, medicines such as indomethacin or ibuprofen are often the first choice. Medicines can work very well for some newborns, with few side effects. The earlier treatment is given, the more likely it is to succeed. If these measures do not work or can't be used, the baby may need to have a medical procedure. A transcatheter device closure is a procedure that uses a thin, hollow tube placed into a blood vessel. The doctor passes a small metal coil or other blocking device through the catheter to the site of the PDA. This blocks blood flow through the vessel. These coils can help the baby avoid surgery. Surgery may be needed if the catheter procedure does not work or it cannot be used due to the baby's size or other reasons. Surgery involves making a small cut between the ribs to repair the PDA. The medication(s) listed below have been approved by the Food and Drug Administration (FDA) as orphan products for treatment of this condition.
- Ibuprofen lysine (Brand name: NeoProfen®)For closure of a clinically significant patent ductus arteriosus in premature infants weighing between 500 and 1500 g, who are no more than 32 weeks gestational age when usual medical management (e.g., fluid restriction, diuretics, respiratory support, etc
Additionl images[edit]
[[File:Blausen 0707 PatentDuctusArteriosus.png|Illustration of Patent Ductus Arteriosus Image:Heart patent ductus arteriosus.jpg|Patent ductus arteriosus [[File:Stent tekst.jpg|An echocardiogram of a stented persisting ductus arteriosus: One can see the aortic arch and the stent leaving. The pulmonary artery is not seen. [[File:PDA Coil.png|An echocardiogram of a coiled persisting ductus arteriosus: One can see the aortic arch, the pulmonary artery, and the coil between them.
Prognosis[edit]
If a small PDA stays open, the baby may eventually develop heart symptoms. Babies with a larger PDA could develop heart problems such as heart failure, high blood pressure in the arteries of the lungs, or an infection of the inner lining of the heart if the PDA does not close.
| Congenital vascular defects / Vascular malformation | ||||||
|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian