Postarthroscopic glenohumeral chondrolysis

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Postarthroscopic glenohumeral chondrolysis | |
|---|---|
| |
| Synonyms | PAGCL |
| Pronounce | N/A |
| Specialty | Orthopedic surgery |
| Symptoms | Shoulder pain, stiffness, loss of motion |
| Complications | Osteoarthritis |
| Onset | Post-surgical |
| Duration | Chronic |
| Types | N/A |
| Causes | Arthroscopic surgery complications |
| Risks | Use of intra-articular pain pumps |
| Diagnosis | Clinical examination, MRI, X-ray |
| Differential diagnosis | Osteoarthritis, Rotator cuff tear |
| Prevention | Avoidance of certain pain management techniques |
| Treatment | Physical therapy, NSAIDs, surgery |
| Medication | N/A |
| Prognosis | Variable, often poor without intervention |
| Frequency | Rare |
| Deaths | N/A |
A condition involving cartilage damage in the shoulder joint following arthroscopic surgery
Postarthroscopic glenohumeral chondrolysis (PAGCL) is a rare but serious condition characterized by the rapid degeneration of the articular cartilage in the glenohumeral joint following arthroscopic surgery. This condition can lead to significant pain, stiffness, and loss of function in the affected shoulder.
Pathophysiology[edit]
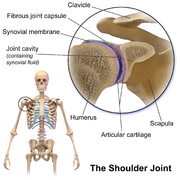
The glenohumeral joint is a ball-and-socket joint formed by the articulation of the humeral head and the glenoid fossa of the scapula. The joint is lined with articular cartilage, which provides a smooth, lubricated surface for joint movement. In PAGCL, this cartilage is rapidly destroyed, leading to exposure of the underlying bone and severe joint dysfunction. The exact mechanism of PAGCL is not fully understood, but it is believed to be associated with the use of intra-articular pain pumps that deliver local anesthetics directly into the joint space. These anesthetics, particularly those containing bupivacaine with epinephrine, have been implicated in chondrolysis due to their toxic effects on cartilage cells.
Clinical Presentation[edit]
Patients with PAGCL typically present with increasing shoulder pain, stiffness, and decreased range of motion following an arthroscopic procedure. Symptoms may develop weeks to months after surgery. On physical examination, there may be tenderness over the joint, crepitus, and significant limitation in both active and passive range of motion.
Diagnosis[edit]
The diagnosis of PAGCL is primarily clinical, supported by imaging studies. Magnetic resonance imaging (MRI) of the shoulder may show loss of cartilage thickness, subchondral bone changes, and joint effusion. X-rays may reveal joint space narrowing and osteophyte formation in advanced cases.
Management[edit]
Management of PAGCL is challenging and focuses on symptom relief and preservation of joint function. Initial treatment may include nonsteroidal anti-inflammatory drugs (NSAIDs), physical therapy, and activity modification. In severe cases, surgical intervention such as arthroscopic debridement, microfracture surgery, or even shoulder arthroplasty may be necessary.
Prevention[edit]
Preventive measures are crucial to reduce the risk of PAGCL. Surgeons are advised to avoid the use of intra-articular pain pumps with potentially chondrotoxic anesthetics. Alternative pain management strategies, such as regional nerve blocks or systemic analgesics, should be considered.
Prognosis[edit]
The prognosis of PAGCL varies depending on the severity of cartilage damage and the effectiveness of treatment. Early diagnosis and intervention can improve outcomes, but many patients may experience persistent pain and functional limitations.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian