Apparent mineralocorticoid excess syndrome

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Apparent mineralocorticoid excess syndrome | |
|---|---|
| |
| Synonyms | AME |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Hypertension, hypokalemia, metabolic alkalosis, low renin and aldosterone levels |
| Complications | Cardiovascular disease, stroke, kidney damage |
| Onset | Childhood |
| Duration | Lifelong |
| Types | N/A |
| Causes | Mutations in the HSD11B2 gene |
| Risks | Genetic predisposition |
| Diagnosis | Genetic testing, urinary steroid profile |
| Differential diagnosis | Liddle syndrome, Congenital adrenal hyperplasia, Cushing's syndrome |
| Prevention | N/A |
| Treatment | Spironolactone, amiloride, dexamethasone |
| Medication | Antihypertensives, potassium-sparing diuretics |
| Prognosis | Variable, depends on management |
| Frequency | Rare |
| Deaths | N/A |
Apparent Mineralocorticoid Excess Syndrome (AME) is a rare genetic disorder characterized by early-onset hypertension, hypokalemia, and low plasma renin activity. This condition arises from mutations in the HSD11B2 gene, leading to impaired conversion of cortisol to its inactive form, cortisone. Elevated cortisol levels result in mineralocorticoid receptor activation, mimicking aldosterone effects and causing the clinical manifestations observed in AME patients.
Etiology and Pathophysiology[edit]
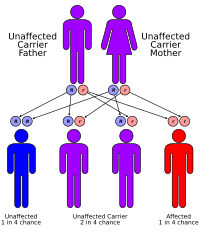
AME is an autosomal recessive disorder caused by mutations in the HSD11B2 gene located on chromosome 16q22.1. This gene encodes the enzyme 11β-hydroxysteroid dehydrogenase type 2 (11β-HSD2), which is responsible for converting active cortisol into inactive cortisone. In the absence of functional 11β-HSD2, cortisol accumulates and aberrantly activates mineralocorticoid receptors in the kidney. This inappropriate activation leads to increased sodium reabsorption, potassium excretion, and water retention, culminating in hypertension and hypokalemia.
Clinical Presentation[edit]
Patients with AME typically present in early childhood with:
- Hypertension: Elevated blood pressure that is often severe and resistant to standard antihypertensive therapies.
- Hypokalemia: Low serum potassium levels, which may manifest as muscle weakness, fatigue, and cardiac arrhythmias.
- Metabolic alkalosis: An increase in blood pH due to excessive bicarbonate retention.
- Low Plasma Renin Activity: Suppressed renin levels resulting from sodium retention and volume expansion.
- Low Aldosterone Levels: Despite the mineralocorticoid excess state, aldosterone levels are low due to feedback inhibition.
Diagnosis[edit]
The diagnosis of AME involves a combination of clinical, biochemical, and genetic evaluations:
- Urinary Steroid Profile: Measurement of urinary free cortisol to cortisone ratio reveals elevated levels in AME patients due to impaired conversion of cortisol to cortisone.
- Genetic Testing: Identification of mutations in the HSD11B2 gene confirms the diagnosis.
- Differential Diagnosis: Conditions such as Liddle's syndrome, congenital adrenal hyperplasia, and other forms of pseudohyperaldosteronism should be considered and excluded.
Management[edit]
Management strategies for AME focus on controlling hypertension and correcting electrolyte imbalances:
- Mineralocorticoid Receptor Antagonists: Medications like spironolactone or eplerenone block the effects of cortisol on mineralocorticoid receptors, reducing sodium retention and potassium loss.
- Potassium-Sparing Diuretics: Agents such as amiloride inhibit sodium reabsorption in the distal nephron, helping to manage hypokalemia and hypertension.
- Dietary Modifications: A low-sodium diet can mitigate sodium retention and assist in blood pressure control.
- Renal Transplantation: In cases unresponsive to medical therapy, renal transplantation has been reported to normalize blood pressure and electrolyte disturbances, as the transplanted kidney provides functional 11β-HSD2 enzyme.
Prognosis[edit]
With appropriate treatment, individuals with AME can achieve significant improvement in blood pressure control and normalization of electrolyte levels. Early diagnosis and management are crucial to prevent complications such as left ventricular hypertrophy, stroke, and chronic kidney disease. Lifelong follow-up is essential to monitor treatment efficacy and adjust therapeutic interventions as needed.
Research Directions[edit]
Ongoing research aims to:
- Elucidate the full spectrum of HSD11B2 mutations and their phenotypic correlations.
- Explore novel therapeutic approaches targeting the molecular mechanisms underlying AME.
- Investigate the long-term outcomes of patients with AME, particularly concerning cardiovascular and renal health.
See Also[edit]
- Hypertension
- Hypokalemia
- Pseudohyperaldosteronism
- Liddle's Syndrome
- Congenital Adrenal Hyperplasia
- Inborn errors of steroid metabolism
- 11β-Hydroxylase I deficiency
- Hyperaldosteronism
- Glucocorticoid-remediable aldosteronism
- Aldosterone and aldosterone synthase
External links[edit]
- Apparent mineralocorticoid excess at NIH's Office of Rare Diseases
| Inborn errors of steroid metabolism | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Adrenal gland disorder | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian