Limb-girdle muscular dystrophy, type 2C
Alternate names[edit]
Limb-girdle muscular dystrophy with gamma-sarcoglycan deficiency; Gamma-sarcoglycanopathy; LGMD2C; Muscular dystrophy, Duchenne-like; Duchenne-like muscular dystrophy, autosomal recessive, type 1; DMDA1; Adhalin deficiency, secondary; DMDA; Severe childhood autosomal recessive muscular dystrophy, North African type; Maghrebian myopathy; Autosomal recessive limb-girdle muscular dystrophy type 2C; Limb-girdle muscular dystrophy due to gamma-sarcoglycan deficiency; Gamma-sarcoglycan-related limb-girdle muscular dystrophy R5; Gamma-sarcoglycan-related LGMD R5; LGMD due to gamma-sarcoglycan deficiency; LGMD type 2C; Limb-girdle muscular dystrophy type 2C
Definition[edit]
Limb-girdle muscular dystrophy type 2C (LGMD2C) is a genetic condition that affects the voluntary muscles around the hips and shoulders. This condition belongs to a group of muscle disorders called limb-girdle muscular dystrophies, which are characterized by progressive loss of muscle bulk and symmetrical weakening of voluntary muscles.
Onset[edit]
Symptoms of LGMD2C usually appear around 6-8 years of age, may be mild or severe, and can progress to loss of the ability to walk by 12-16 years.
Cause[edit]
LGMD2C is caused by mutations in the SGCG gene.
Inheritance[edit]
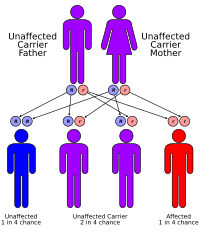
It is inherited in an autosomal recessive manner.
Signs and symptoms[edit]
Symptoms may additionally include: enlargement (hypertrophy) of the calf muscle and tongue, diseases of the heart muscle (cardiomyopathy), and respiratory abnormalities.
For most diseases, symptoms will vary from person to person. People with the same disease may not have all the symptoms listed. 30%-79% of people have these symptoms
- Abnormal macrophage morphology
- Broad-based gait(Wide based walk)
- Calf muscle hypertrophy(Increased size of calf muscles)
- Calf muscle pseudohypertrophy
- Difficulty climbing stairs(Difficulty walking up stairs)
- Difficulty running
- Elevated serum creatine kinase(Elevated blood creatine phosphokinase)
- EMG: myopathic abnormalities
- EMG: myotonic discharges
- EMG: myotonic runs
- EMG: positive sharp waves
- Frequent falls
- Increased endomysial connective tissue
- Increased variability in muscle fiber diameter
- Lumbar hyperlordosis(Excessive inward curvature of lower spine)
- Macroglossia(Abnormally large tongue)
- Right ventricular hypertrophy
- Scapular winging(Winged shoulder blade)
- Upper limb muscle weakness(Decreased arm strength)
- Waddling gait('Waddling' gait)
5%-29% of people have these symptoms
- Achilles tendon contracture(Shortening of the achilles tendon)
- Gowers sign
- Left ventricular systolic dysfunction
- Long face(Elongation of face)
- Neck flexor weakness(Neck flexion weakness)
- Scoliosis
- Tip-toe gait(Walking on tiptoes)
Diagnosis[edit]
- The limb-girdle muscular dystrophies typically show degeneration/regeneration (dystrophic changes) on muscle biopsy, which is usually associated with elevated serum creatine kinase concentration.
- For any male or female suspected of having limb-girdle muscular dystrophy, it is necessary to first rule out an X-linked dystrophinopathy.
- Biochemical testing (i.e., protein testing by immunostaining or immunblotting) performed on a muscle biopsy can establish the diagnosis of the following LGMD types: sarcoglycanopathy, calpainopathy, dysferlinopathy, and O-linked glycosylation defects (also known as dystroglycanopathy).
- In some cases, demonstration of complete or partial deficiencies for any particular protein can then be followed by mutation studies of the corresponding gene.
- Pathogenic variants in a number of genes have been associated with types of LGMD.[1][1].
Treatment[edit]
There is no specific treatment for LGMD2C. Management of the condition is based on each person's symptoms and may include:
- Weight control to avoid obesity
- Physical therapy and stretching exercises to promote mobility and prevent contractures
- Use of mechanical aids such as canes, walkers, orthotics, and wheelchairs as needed to help ambulation and mobility
- Monitoring and surgical intervention as needed for orthopedic complications such as foot deformity and scoliosis
- Monitoring of respiratory function and use of respiratory aids when indicated
- Monitoring for evidence of diseases of the heart muscle (cardiomyopathy)
- Social and emotional support and stimulation to maximize a sense of social involvement and productivity and to reduce the sense of social isolation common in these disorders
References[edit]
- ↑ Pegoraro E, Hoffman EP. Limb-Girdle Muscular Dystrophy Overview – RETIRED CHAPTER, FOR HISTORICAL REFERENCE ONLY. 2000 Jun 8 [Updated 2012 Aug 30]. In: Adam MP, Ardinger HH, Pagon RA, et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993-2020. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1408/
| Muscular dystrophy | ||||||||
|---|---|---|---|---|---|---|---|---|
* Category
|
| Diseases of muscle, neuromuscular junction, and neuromuscular disease | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Inherited disorders of trafficking / vesicular transport proteins | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
See also vesicular transport proteins
|
| Cell membrane protein disorders (other than Cell surface receptor, enzymes, and cytoskeleton) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
See also other cell membrane proteins
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian