Vogt–Koyanagi–Harada disease
Autoimmune multisystem inflammatory disorder affecting eyes, ears, skin, and CNS
| Vogt–Koyanagi–Harada disease | |
|---|---|
| VKHS.jpg | |
| Dermatologic manifestations of VKH disease | |
| Synonyms | Vogt–Koyanagi–Harada syndrome, uveomeningitis syndrome, uveomeningoencephalitic syndrome
|
| Specialty | Ophthalmology, Neurology, Dermatology, Immunology |
| Symptoms | Eye pain, redness, vision loss, tinnitus, vertigo, headache, meningismus, skin depigmentation, hair whitening |
| Complications | Permanent vision loss, hearing impairment, chronic uveitis |
| Usual onset | Young to middle-aged adults (20–50 years) |
| Duration | Chronic, recurrent |
| Types | Complete, incomplete, probable VKH |
| Causes | Autoimmune response targeting melanocytes |
| Risk factors | Genetic predisposition (HLA-DR4), ethnicity (Asian, Hispanic, Native American descent) |
| Diagnosis | Clinical evaluation, fluorescein angiography, lumbar puncture, imaging studies |
| Differential diagnosis | Sympathetic ophthalmia, sarcoidosis, systemic lupus erythematosus, multiple sclerosis |
| Prevention | None known |
| Treatment | Corticosteroids, immunosuppressants, biologics |
| Medication | Prednisone, azathioprine, cyclosporine, infliximab |
| Prognosis | Generally good with prompt treatment; delayed treatment may result in severe vision impairment |
| Frequency | Rare |
| Deaths | Rare |
Vogt–Koyanagi–Harada disease (VKH disease) is a multisystem, chronic inflammatory disorder of presumed autoimmune origin, primarily affecting tissues containing melanin, particularly the eyes, ears, skin, and central nervous system. The disease is characterized by bilateral diffuse uveitis, neurologic involvement, auditory disturbances, and dermatological manifestations, such as vitiligo, poliosis, and alopecia.
Signs and symptoms[edit]
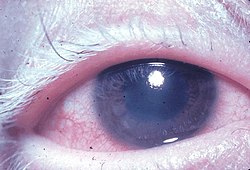
VKH disease progresses through four clinical phases, each marked by distinctive symptoms:
Prodromal phase[edit]
This initial phase typically lasts a few days and often resembles a viral illness, characterized by:
- Fever
- Headache
- Meningismus (neck stiffness, photophobia, headache)
- Auditory symptoms (tinnitus, vertigo, hypoacusis)
- Sensitivity of hair and skin to touch
- Orbital pain, photophobia, excessive tearing
Acute uveitic phase[edit]
This phase occurs shortly after the prodromal period and lasts several weeks, characterized primarily by severe bilateral uveitis:
- Eye redness and pain
- Sudden vision loss or blurred vision
- Anterior chamber inflammation
- Optic disc edema
- Serous retinal detachment
Convalescent phase[edit]
During this stage, inflammation subsides but skin and hair changes become evident:
- Vitiligo (especially in the sacral region)
- Poliosis (white patches of hair, notably eyelashes)
- Alopecia (hair loss)
- Improvement of visual acuity, though residual damage can remain
Chronic recurrent phase[edit]
Intermittent episodes of uveitis recur months to years later, which can result in:
- Permanent visual impairment or blindness
- Chronic inflammation requiring ongoing immunosuppressive therapy
Causes[edit]
VKH disease is presumed to be an autoimmune response against melanocyte-associated antigens. Melanocytes, which produce the pigment melanin, are targeted, leading to inflammation and destruction of pigmented tissues in eyes, skin, and auditory structures.
Risk factors[edit]
The following increase susceptibility to VKH disease:
- Ethnicity: More common in Asian, Hispanic, Native American, and Middle Eastern populations
- Genetic predisposition, particularly association with the HLA-DR4 allele
- Age and gender: Commonly affects young to middle-aged adults (20–50 years), more frequently in females
Pathophysiology[edit]
Autoimmune inflammation targets melanocyte-containing tissues, leading to granulomatous inflammation. In the eyes, this leads to severe uveitis, retinal detachment, and possible vision loss. Similar inflammatory processes affect the meninges, inner ear, and skin, causing characteristic symptoms across multiple organ systems.
Diagnosis[edit]
Diagnosis of VKH is clinical, based on symptoms and exclusion of other diseases, supported by:
- Ophthalmic examination, including fluorescein angiography
- Lumbar puncture showing CSF pleocytosis
- Imaging (MRI) to exclude other neurologic disorders
- Audiometric testing for hearing abnormalities
The diagnosis is classified as complete, incomplete, or probable VKH based on specific clinical and laboratory criteria.
Differential diagnosis[edit]
Conditions considered during differential diagnosis include:
- Sympathetic ophthalmia
- Sarcoidosis
- Systemic lupus erythematosus (SLE)
- Multiple sclerosis
- Acute disseminated encephalomyelitis (ADEM)
Treatment[edit]
Early diagnosis and aggressive treatment improve prognosis significantly. Treatment focuses on controlling inflammation and preventing permanent organ damage:
- High-dose corticosteroids (oral prednisone or intravenous methylprednisolone)
- Immunosuppressive agents (azathioprine, cyclosporine, methotrexate)
- Biological agents (e.g., infliximab) for refractory cases
- Regular follow-up to monitor ocular inflammation and disease recurrence
Complications[edit]
Potential complications of VKH disease include:
- Chronic uveitis leading to cataracts, glaucoma, and vision loss
- Permanent hearing impairment
- Neurological deficits or cognitive impairment due to chronic CNS inflammation
Prognosis[edit]
The prognosis for VKH disease is generally favorable with prompt initiation and adequate duration of immunosuppressive therapy. Delayed diagnosis or inadequate treatment increases the risk of permanent visual impairment and hearing loss. Lifelong monitoring and management are typically required.
Epidemiology[edit]
VKH disease is considered rare globally, though prevalence varies significantly by ethnicity. It is more common among populations with increased melanin content, including Asian, Hispanic, Native American, and Middle Eastern communities. Women are affected more frequently than men, with peak onset occurring between ages 20 and 50.
History[edit]
VKH disease is named after ophthalmologists who described the condition independently:
- Alfred Vogt (Swiss, 1906) described anterior uveitis and depigmentation.
- Yoshizo Koyanagi (Japanese, 1929) reported similar ocular and dermatologic symptoms.
- Einosuke Harada (Japanese, 1926) described the neurologic and audiological manifestations.
Research[edit]
Current research is exploring:
- Genetic susceptibility factors and biomarkers for early diagnosis
- Mechanisms of autoimmune response against melanocytes
- Improved therapeutic approaches using biologic agents and targeted immunotherapies
See also[edit]
External links[edit]
| Hypersensitivity and autoimmune diseases (279.5–6) | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian