Infection

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Infection | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Fever, chills, fatigue, muscle aches, cough, diarrhea |
| Complications | Sepsis, organ failure, chronic infection |
| Onset | Varies by type of infection |
| Duration | Acute or chronic |
| Types | N/A |
| Causes | Bacteria, viruses, fungi, parasites |
| Risks | Immunocompromised, poor hygiene, close contact |
| Diagnosis | Blood test, culture, imaging |
| Differential diagnosis | N/A |
| Prevention | Vaccination, hand washing, sanitation |
| Treatment | Antibiotics, antivirals, antifungals, antiparasitics |
| Medication | N/A |
| Prognosis | Varies by type and severity |
| Frequency | Common |
| Deaths | N/A |



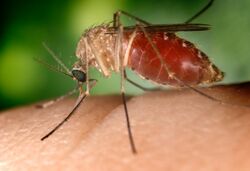






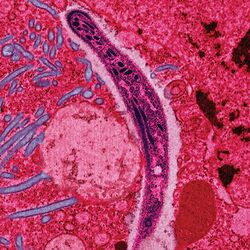
Infection is the invasion of an organism's body tissues by disease-causing agents, such as bacteria, [virus]]es, fungi, parasites, protozoa or other microorganisms. Infection refers to the invasion of an organism's body tissues by disease-causing agents, which can include bacteria, viruses, fungi, parasites, protozoa, and other microorganisms. The resultant interaction between the host and the invading organisms can lead to a variety of outcomes, ranging from symbiosis to severe disease and even death.
Types of Infectious Agents[edit]
There are several classes of infectious agents, each of which has unique properties and modes of infection.
Bacteria[edit]
Bacteria are single-celled microorganisms that can cause a wide range of infections. They are responsible for many common diseases, including strep throat, urinary tract infections, and certain types of pneumonia.[1]
Viruses[edit]
Viruses are small, non-living infectious agents that need a host cell to reproduce. They can cause diseases ranging from the common cold and influenza to more severe diseases like HIV/AIDS and COVID-19.[2]
Fungi[edit]
Fungal infections can be caused by various types of fungi, including yeasts and molds. Examples of fungal infections include ringworm, athlete's foot, and systemic infections like histoplasmosis.[3]
Parasites[edit]
Parasites are organisms that live on or in a host organism and get their food from or at the expense of their host. Parasitic infections can be caused by protozoa (like malaria) or helminths (like tapeworms).[4]
Pathogenesis[edit]
The pathogenesis of an infection involves the mechanisms that lead to the development of disease after the invasion of a host by a pathogen. This process can be influenced by both the characteristics of the pathogen and the host's immune response.[5]
Diagnosis, Treatment, and Prevention[edit]
Infection diagnosis is primarily based on clinical presentation, laboratory testing, and imaging studies. Treatment varies according to the type of infection and can include antibiotics, antivirals, antifungals, or antiparasitics.[6] Prevention measures can include vaccination, hand hygiene, safe food handling, and using insecticide-treated nets.
Glossary of infection control terms[edit]
- ABHR See alcohol-based hand rub
- ACS See ambulatory care settings
- Airborne precautions Actions taken to prevent or minimize the transmission of infectious agents or organisms that remain infectious when suspended in the air.
- Airborne transmission A means of spreading infection in which airborne droplet nuclei are inhaled by uninfected people.
- Alcohol-based hand rub (ABHR) A method of hand hygiene that includes an alcohol-containing preparation designed for application to the hands for reducing the number of viable microorganisms on the hands. ABHR is not an alternative for washing with soap and water if hands are visibly soiled.
- Ambulatory care settings (ACS) Facilities that provide health care to patients who do not remain overnight.
- Antibiotic Type of antimicrobial agent made from a mold or a bacterium that kills, or slows the growth of other microbes, specifically bacteria. Examples include penicillin and streptomycin.
- Antibody A protein found in the blood that is produced in response to foreign substances (e.g., antigens) invading the body. Antibodies protect the body from disease by binding to these organisms and destroying them.
- Antigen A foreign substance, usually protein or carbohydrate substance (as a toxin or enzyme) capable of stimulating an immune response, usually the production of antibodies.
- Antimicrobial agents: A general term for the drugs, chemicals, or other substances that either kill or slow the growth of microbes. Among the antimicrobial agents in use today are antibacterial drugs (which kill bacteria), antiviral agents (which kill viruses), antifungal agents (which kill fungi), and anti- parasitic drugs (which kill parasites).
- Antimicrobial resistance: The result of microbes changing in ways that reduce or eliminate the effectiveness of drugs, chemicals, or other agents to cure or prevent infections. Examples include multi- drug resistant organisms (MDROs) such as methicillin-resistant Staphylococcus aureus (MRSA), and vancomycin-resistant enterococci (VRE). Also known as drug resistance.
- Antiseptic A germicide that is used on skin or living tissue for the purpose of inhibiting or destroying microorganisms. Examples include alcohols, chlorhexidine, chlorine, hexachlorophene, and iodine.
- APIC See Association for Professionals in Infection Control and Epidemiology
- Asepsis: Prevention from contamination with microorganisms. Includes sterile conditions on tissues, on materials, and in rooms, as obtained by excluding, removing, or killing organisms.
- Association for Professionals in Infection Control and Epidemiology (APIC): A voluntary membership organization representing individuals occupationally or professionally involved in the practice and management of infection prevention and control or the application of epidemiology, such as infection preventionists. APIC develops resources and standards, provides educational opportunities, and plays a leadership role in communicating with partners.
- Bacteria Single-celled organisms that live in and around us. Bacteria may be helpful, but in certain conditions may cause illnesses such as strep throat, most ear infections, and pneumonia.
- Barrier precautions Any method or device used to decrease contact with potentially infectious body fluids. Examples may include masks, gloves, and gowns.
- BBP See Bloodborne Pathogens Standard
- Bloodborne Pathogens Standard (BBP) A standard developed, promulgated, and enforced by the Occupational Safety and Health Administration (OSHA) directing employers to protect employees from occupational exposure to blood and other potentially infectious material.
- Bloodborne pathogens: Disease-producing microorganisms spread by contact with blood or other body fluids from an infected person. Examples include hepatitis B and C as well as HIV.
- Bloodstream infection: A condition in which bacteria enter the blood. This may occur through a wound or infection, or through a surgical procedure or injection. In Virginia, central line-associated bloodstream infections (CLABSIs) are reportable to the health department.
- C. difficile See Clostridium difficile
- CABG: See coronary artery bypass graft
- CA-MRSA: Community-associated (CA) methicillin-resistant Staphylococcus aureus (MRSA). Colonization or infection with this organism develops in people who have not recently been evaluated or treated at a healthcare facility therefore, it is defined as originating from the community.
- Caregivers: All persons who are not employees of an organization, are not paid, and provide or assist in providing healthcare to a patient (e.g., family member, friend) and acquire technical training as needed based on the tasks that must be performed.
- Carrier An individual who is found to be colonized at one or more body sites with an organism, but has no signs or symptoms of active infection.
- Catheter: A tubular, flexible surgical instrument that is inserted into a body opening to withdraw or introduce fluid.
- CAUTI See catheter-associated urinary tract infection
- CDAD: See Clostridium difficile-Associated Disease
- CDC: See Centers for Disease Control and Prevention
- CDI: See Clostridium difficile infection
- Centers for Disease Control and Prevention (CDC) A federal agency of the U.S. government that provides facilities and services for the investigation, identification, prevention, and control of disease and is a global leader in public health.
- Centers for Medicare and Medicaid Services (CMS): A federal agency that runs the national health insurance programs Medicare and Medicaid.
- Central line: A flexible tube that is inserted near a patient's heart or into one of the large blood vessels near the heart. A central line can be used to administer fluids, antibiotics, or medical treatments.
- Central line-associated bloodstream infection (CLABSI) An infection that spreads through the blood from its origin on a central line. A CLABSI rate is usually calculated per 1,000 (the total number of CLABSIs divided by the total number of central line days, multiplied by 1,000).
- Chlorhexidine soap: a topical antimicrobial agent used to treat or help prevent infections.
- CLABSI: See central line-associated bloodstream infection
- Cleaning: The removal of visible soil, organic, and inorganic contamination from a device or surface, using either the physical action of scrubbing with a surfactant or detergent and water or an energy- based process with appropriate chemical agents.
- Clostridium difficile: An anaerobic, gram-positive, spore-forming bacillus that can cause diarrhea and other intestinal diseases when competing bacteria in the gut are diminished by antibiotics.
- Clostridium difficile -associated Disease (CDAD): An intestinal illness caused by toxins that are produced by a specific type of bacteria named Clostridium difficile.
- CMS: See Centers for Medicare and Medicaid Services
- Cohorting: The practice of grouping patients infected or colonized with the same infectious agent together to confine their care to one area and prevent contact with susceptible patients.
- Colonization The presence of microorganisms on or within body sites without symptoms, detectable host immune response, cellular damage, or clinical expression. Colonized individuals may become a source of transmission.
- Communicable disease An infectious disease carried by microorganisms and transmitted through people, animals, insects, surfaces, food, or air.
- Community-acquired infections: See community-associated infections
- Community-associated infections (CA) Infections that are contracted outside of a healthcare facility and are present or incubating at the time of admission or develop within a designated period of time after admission, unlike healthcare-associated infections (HAIs). Formerly known as community-acquired infections.
- Contact precautions Type of transmission-based precautions that requires barrier precautions for direct contact with resident or objects/surfaces contaminated with an infectious agent.
- Contamination The presence of an infectious agent on a body surface or on clothes, gowns, gloves, bedding, furniture, computer keyboards, or other inanimate objects that may be capable of producing disease or infection.
- Coronary artery bypass graft (CABG): A surgical replacement for clogged blood vessels located near the heart.
- Decolonization therapy Topical and/or systemic antibiotic treatment used with the intention of eliminating carriage (colonization) of a microorganism.
- Decontamination A process or treatment that renders a medical device, instrument, or environmental surface safe to handle because it is no longer capable of transmitting particles of infectious material.
- Denominator Number of people who are potentially capable of experiencing an event or outcome of interest. The denominator, along with the numerator, is used to calculate a rate. The denominator is the bottom half of a fraction.
- Department of Health Public health agency, providing regulation, inspection, licensing, emergency response, education and other programs to measure and protect the health of residents. The health department works to protect and improve the health of people in the geographic area it serves (state or local).
- Direct contact transmission: Physical transfer of microorganisms between a susceptible host and an infected or colonized person.
- Disinfectant A chemical agent used on inanimate (non-living) objects to destroy virtually all recognized pathogenic microorganisms, but not necessarily all microbial forms (e.g., bacterial spores).
- Disinfection The destruction of pathogenic and other kinds of microorganisms by physical or chemical means. Disinfection is less lethal than sterilization, because it destroys most recognized pathogenic microorganisms, but not necessarily all microbial forms, such as bacterial spores.
- Droplet precautions Actions designed to reduce and prevent the transmission of pathogens spread through close respiratory or mucous membrane contact with respiratory secretions.
- Droplets Small particles of moisture that may be generated when a person coughs or sneezes or when water is converted to a fine mist by an aerator or shower head. Droplets may contain infectious microorganisms and tend to quickly settle out from the air; therefore, risk of disease transmission is generally limited to persons in close proximity to the droplet source.
- Drug resistance See antibiotic resistance
- Endotoxin A toxin produced by certain bacteria. For example, Clostridium difficile toxin can cause diarrhea.
- Epidemiologically important pathogens: Infectious agents that have one or more of the following characteristics: 1) are readily transmissible; 2) have a proclivity toward causing outbreaks; 3) may be associated with a severe outcome; or 4) are difficult to treat. Examples include Acinetobacter, MRSA, and C. difficile.
- Epidemiology The study of the distribution and determinants of disease in human populations. Epidemiologists are often sent to investigate outbreaks.
- ESBL See extended-spectrum β-lactamase
- Exposure time: Period of time during a sterilization or disinfection process in which items are exposed to the sterilant or disinfectant at the parameters specified by the manufacturer, including time, concentration, temperature, pressure.
- Extended-spectrum β-lactamase (ESBL): β-lactamases are enzymes that destroy certain antibiotics; ESBLs are bacteria that have acquired these enzymes and become resistant to those drugs.
- Foley catheter See urinary catheter
- Fungi Single-celled or multicellular organisms that can be opportunistic pathogens that cause infections in immunocompromised persons or pathogens that cause infections in healthy persons. Examples include athlete's foot, yeast infections, and ringworm. Fungi are also used for the development of antibiotics, antitoxins, and other drugs used to control various human diseases.
- Gastroenteritis Inflammation of the stomach and the intestines that causes symptoms such as nausea, vomiting, and diarrhea.
- Gastrointestinal (GI) infection: See gastroenteritis
- HA-MRSA: See healthcare-associated methicillin-resistant Staphylococcus aureus
- HAI: See healthcare-associated infection
- Hand hygiene: A general term that applies the following: 1) hand washing with antimicrobial/non- antimicrobial soap and water or 2) antiseptic handrub (waterless antiseptic product, most often alcohol- based, rubbed on all surfaces of hands).
- HCW: See healthcare worker
- Healthcare-associated infection (HAI): An infection that develops in a patient who is cared for in any setting where healthcare is delivered and is related to receiving health care. Formerly known as nosocomial infection.
- Healthcare-associated methicillin-resistant Staphylococcus aureus (HA-MRSA) MRSA colonization or infection that develops in people who have had recent contact with a healthcare facility or have been in a healthcare facility for greater than 48 hours.
- Healthcare epidemiologist: A person with medical training and/or masters or doctorate-level epidemiological training who has received advanced training in healthcare epidemiology. Typically these professionals direct or provide consultation to an infection prevention program in a hospital, long term care facility (LTCF), or healthcare delivery system.
- Healthcare Infection Control Practices Advisory Committee (HICPAC): A panel of experts who advise the CDC on matters of healthcare-associated infection surveillance, control, and prevention and release guidelines on a regular basis.
- Healthcare worker (HCW) All paid and unpaid persons who work in a healthcare setting.
- HICPAC See Healthcare Infection Control Practices Advisory Committee
- ICP: See infection preventionist
- ICU See intensive care unit
- Immunity: Protection against a disease. Immunity is indicated by the presence of antibodies in the blood and can usually be determined with a laboratory test.
- Immunization The process or procedure by which a subject is rendered immune, or resistant to a specific disease. This term is often used interchangeably with vaccination or inoculation, although the act of inoculation/vaccination does not always result in immunity.
- Immunocompromised: Those whose immune mechanisms are deficient because of congenital or acquired immunologic disorders (e.g., human immunodeficiency virus [HIV] infection), chronic diseases (e.g., diabetes mellitus, cancer, emphysema), malnutrition, or immunosuppressive therapy of another disease process.
- Incidence: The number of new cases of infection or disease or colonization identified in a specific population in a given time period.
- Incidence rate: The number of new cases of disease during a specific time period divided by the population at risk.
- Indirect contact transmission Spread of a disease to a susceptible host through contact with a contaminated intermediate object, usually inanimate.
- Infection preventionist (IP) A healthcare worker who specializes in infection surveillance, control, and prevention. Also know as an Infection Control and Prevention Professional or an Infection Control Practitioner (ICP).
- Infection control and prevention program: A multidisciplinary program that includes a group of activities to ensure that recommended practices for the prevention of healthcare-associated infections are implemented and followed by healthcare workers, making the healthcare setting safe from infection for patients and healthcare personnel. This program usually includes surveillance of healthcare- associated infections (HAIs), investigation of any HAI trends or problems, implementation of prevention practices, evaluation and management of oubtreaks, and reporting HAI data to designated authorities.
- Infection rate: Number of infections reported in a specified period of time divided by the population at risk for the infection during the same specified period of time.
- Infection: The invasion of the body by pathogenic microorganisms and their multiplication which can lead to tissue damage and disease.
- Influenza: Also known as flu. A serious and sometimes deadly respiratory infection that can spread quickly in a community.
- Intensive care unit (ICU) Hospital unit that provides intensive observation and treatment of patients either dealing with or at risk of developing life-threatening problems. Also known as a critical care unit.
- Invasive procedure: A medical procedure that involves entering the body, usually by cutting or puncturing the skin or by inserting instruments into the body.
- IP: See infection preventionist
- Latent tuberculosis infection (LTBI) A condition in which living tubercle bacilli (M. tuberculosis) are present in the body but the disease is not clinically active.
- Long-term care facility (LTCF) Facility that provides rehabilitative, restorative, and/or ongoing skilled nursing care to patients or residents in need of assistance with activities of daily living. Long-term care facilities include nursing homes, rehabilitation facilities, inpatient behavioral health facilities, and long- term chronic care hospitals.
- LTBI: See latent tuberculosis infection
- LTCF: See long-term care facility
- Mask: A term that applies collectively to items used to cover the nose and mouth and includes both procedure masks and surgical masks.
- MDRO: See multidrug-resistant organism
- Methicillin-resistant Staphylococcus aureus (MRSA): A type of bacteria that has become resistant to a group of powerful drugs. Not all Staphylococcus aureus strains are resistant to these drugs. Sensitive strains are called MSSA.
- Microbes: See microorganisms
- Microorganisms: An organism that can be seen only with the aid of a microscope and that typically consists of only a single cell. Microorganisms include bacteria, fungi, parasites, and viruses.
- MRSA: See methicillin-resistant Staphylococcus aureus.
- Multidrug-resistant organism (MDRO): Type of bacteria that has become resistant to many of the drugs that used to be effective against it.
- N-95 respirator One of nine types of disposable particulate respirators. "95" refers to the percentage of particles filtered.
- National Healthcare Safety Network (NHSN): A secure computer system for hospitals throughout America to share information about their healthcare-associated infections. Managed by the Division of Healthcare Quality Promotion (DHQP) at the Centers for Disease Control and Prevention (CDC).
- NHSN See National Healthcare Safety Network
- Norovirus A very contagious virus transmitted from person-to-person or via contaminated food, water, or objects, causing outbreaks of vomiting and diarrhea.
- Nosocomial infection : See healthcare-associated infection
- Numerator Number of individuals who experience an event or outcome of interest. The numerator, along with the denominator, is used to calculate a rate. The numerator is the top half of a fraction.
- Occupational Safety and Health Administration (OSHA): An agency of the United States Department of Labor that has federal industrial safety regulations, including the Bloodborne Pathogens (BBP) Standard.
- Occupational exposure: A reasonably anticipated skin, eye, mucous membrane, or parenteral contact with blood or other potentially infectious materials that may result from the performance of an employee's duties.
- OSHA: See Occupational Safety and Health Administration
- Outbreak: An increase in the incidence of disease in a facility above the baseline level or a cluster of new cases that are epidemiologically linked.
- Parasite: An organism that lives in or on and takes its nourishment from another organism and cannot live independently. Examples include scabies and Giardia.
- Pathogens: Bacteria, viruses, parasites, or fungi that can cause disease.
- Personal protective equipment (PPE) A variety of barriers used alone or in combination to protect mucous membranes, skin, and clothing from contact with infectious agents. PPE includes gloves, masks, respirators, goggles, face shields, and gowns.
- Pneumonia: An infection of one or both lungs caused by bacteria, viruses, fungi, or other organisms.
- Post-exposure prophylaxis: The administration of medications following exposure to a disease in an attempt to prevent infection.
- PPE See personal protective equipment
- Prevalence: The total number of disease cases (new and existing) within a population at a given time.
- Rate An expression of the risk of an event, such as infection or death, in relation to a unit of population during a specified time period.
- Residential care setting A facility in which people live, minimal medical care is delivered, and the psychosocial needs of the residents are provided for.
- Respirator A personal protective device worn by healthcare personnel to protect them from inhalation exposure to airborne infectious agents that are < 5 micrometers in size.
- Respiratory hygiene/ Cough etiquette A combination of measures designed to minimize the transmission of respiratory pathogens via droplet or airborne routes.
- Risk adjustment Because some facilities treat higher-risk patients who have a greater chance of dying or acquiring a healthcare-associated infection, this statistical process is used to adjust rates of illness or death to account for differences in patient risk.
- SCIP See Surgical Care Improvement Project
- SHEA See Society for Healthcare Epidemiology of America
- Society for Healthcare Epidemiology of America (SHEA): A voluntary membership organization representing healthcare epidemiologists that helps publish infection prevention guidelines and best practices. See healthcare epidemiologist.
- Spore: The dormant stage some bacteria will enter when environmental conditions cause stress to the organism or no longer support its continued growth. C. difficile spores are highly resistant to cleaning and disinfection measures, and the spores also make it possible for the organism to survive passage through the stomach, resisting the killing effect of gastric acid.
- SSI: See surgical site infection
- Standard precautions: A group of infection prevention practices that apply to all patients, regardless of infection status. Standard precautions is based on the principle that all blood, body fluids, secretions, excretions except sweat, non-intact skin, and mucous membranes may contain transmissible infectious agents. Standard precautions include hand hygiene, and depending on the anticipated exposure, use of gloves, gown, mask, eye protection, or face shield. Also, equipment or items in the patient environment likely to have been contaminated with infectious fluids must be handled in a manner to prevent transmission of infectious agents. Formerly known as universal precautions.
- Standardized infection ratio (SIR) A summary measure used to compare the healthcare-associated infection experience among one or more groups of patients to that of a standard population. It is calculated as the observed number of infections divided by the expected number of infections.
- Sterile/sterility: State of being free from all living microorganisms.
- Sterilization: The use of a physical or chemical procedure to destroy all microorganisms.
- Surgical Care Improvement Project (SCIP): A series of process measures before, during, or after surgery. Compliance with these measures is considered best practice to reduce the risk of surgical site infection or complication.
- Surgical site infection (SSI) An infection of a surgical wound, tissue, or organ space near the wound.
- Surveillance: The ongoing, systematic collection, analysis, interpretation, and dissemination of data regarding a health-related event for use in public health action to reduce morbidity and mortality and to improve health.
- Terminal cleaning: The thorough cleaning of a person's room following discharge or transfer in order to prevent transmission of potentially infectious organisms to the next room occupant.
- Transmission-based precautions: A set of practices that apply to patients with documented or suspected infection or colonization with highly transmissible or epidemiologically important pathogens for which precautions beyond the standard precautions are needed to interrupt disease transmission.
- Universal precautions: See standard precautions
- Urinary catheter: A small, flexible tube that is inserted into the urethra to the bladder to allow for the drainage of urine. Also known as a Foley catheter.
- Urinary tract infection (UTI) An infection that can happen anywhere along the urinary tract. A UTI that occurs in a patient with a catheter is known as a catheter-associated UTI (CAUTI).
- UTI: See urinary tract infection
- Vaccination See immunization
- Vaccine: A product that produces immunity therefore protecting the body from the disease. Vaccines can be administered by injection, mouth, or aerosol.
- VAP: See ventilator-associated pneumonia
- VDH: See Virginia Department of Health
- Ventilator: A device that pumps air into the lungs of patients who cannot breathe well on their own.
- Ventilator-associated pneumonia (VAP) Severe lung infection that develops after a patient is placed on a ventilator.
- Virginia Department of Health (VDH) Network of state and local health departments in Virginia.
- Virus: A microorganism smaller than bacteria that cannot grow or reproduce apart from a living cell. Examples include influenza, chicken pox, hepatitis, and HIV.
- Infection Prevention-Related Terms
See Also[edit]
- ↑ Madigan, M., & Martinko, J. (Eds.). (2005). Brock Biology of Microorganisms (11th ed.). Prentice Hall.
- ↑ Alberts, B., Johnson, A., Lewis, J., et al. (2002). Molecular Biology of the Cell (4th ed.). Garland Science.
- ↑ Romani, L. (2011). Immunity to fungal infections. Nature Reviews Immunology, 11(4), 275-288.
- ↑ John, D. T., & Petri, W. A. (2006). Markell and Voge's Medical Parasitology (9th ed.). Saunders.
- ↑ Salmon, D. E. (2006). The Bacteriology of Diphtheria: Including Sections on the History, Epidemiology and Pathology of the Disease, the Mortality Caused by It, the Toxins and Antitoxins and the Serum Disease. Read Books.
- ↑ Mims, C., Dockrell, H. M., Goering, R. V., et al. (2004). Medical Microbiology. Mosby.
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian