Fracture
A bone fracture (abbreviated FRX or Fx, Fx, or #) is a medical condition in which there is a partial or complete break in the continuity of the bone. In more severe cases, the bone may be broken into several pieces.
Causes[edit]
A bone fracture may be the result of high force impact or stress, or a minimal trauma injury as a result of certain medical conditions that weaken the bones, such as osteoporosis, osteopenia, bone cancer, or osteogenesis imperfecta, where the fracture is then properly termed a pathologic fracture.
Types of fractures[edit]
- Avulsion fracture – a muscle or ligament pulls on the bone, fracturing it.
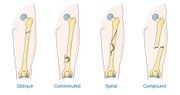
- Comminuted fracture – the bone is shattered into many pieces.
- Compression (crush) fracture – generally occurs in the spongy bone in the spine. For example, the front portion of a vertebra in the spine may collapse due to osteoporosis.
- Fracture dislocation – a joint becomes dislocated, and one of the bones of the joint has a fracture.
- Greenstick fracture – the bone partly fractures on one side, but does not break completely because the rest of the bone can bend. This is more common among children, whose bones are softer and more elastic.
- Hairline fracture – a partial fracture of the bone. Sometimes this type of fracture is harder to detect with routine xrays.
- Impacted fracture – when the bone is fractured, one fragment of bone goes into another.
- Intraarticular fracture – where the break extends into the surface of a joint
- Longitudinal fracture – the break is along the length of the bone.
- Oblique fracture – a fracture that is diagonal to a bone’s long axis.
- Pathological fracture – when an underlying disease or condition has already weakened the bone, resulting in a fracture (bone fracture caused by an underlying disease/condition that weakened the bone).
- Spiral fracture – a fracture where at least one part of the bone has been twisted.
- Stress fracture – more common among athletes. A bone breaks because of repeated stresses and strains.
- Torus (buckle) fracture – bone deforms but does not crack. More common in children. It is painful but stable.
- Transverse fracture – a straight break right across a bone.
Non-healing fracture. A non-healing (nonunion) fracture is a fracture that has failed to unite completely. Nonunion is usually established when a minimum of 9 months has elapsed since the injury and the fracture site has shown no, or minimal, progressive signs of healing for a minimum of 3 months.
- Complex fracture - A complex fracture is a fracture with one or more of the following:
Fracture Healing[edit]
Mechanism of Fracture Healing[edit]
The mechanism of fracture healing is an intricate and fluent process. This process can be broken down into four stages. However, these stages have considerable overlap.
Hematoma Formation (Days 1 to 5)[edit]
This stage begins immediately following the fracture. The blood vessels supplying the bone and periosteum are ruptured during the fracture, causing a hematoma to form around the fracture site. The hematoma clots, and forms the temporary frame for subsequent healing. The injury to bone results in the secretion of pro-inflammatory cytokines like tumor necrosis factor-alpha (TNF-α), bone morphogenetic proteins (BMPs), and interleukins (IL-1, IL-6, IL-11, IL-23). These cytokines act to stimulate essential cellular biology at the site, attracting macrophages, monocytes, and lymphocytes. These cells act together to remove damaged, necrotic tissue and secrete cytokines like vascular endothelial growth factor (VEGF) to stimulate healing at the site.
Fibrocartilaginous Callus Formation (Days 5 to 11)[edit]
The release of VEGF leads to angiogenesis at the site, and within the hematoma, fibrin-rich granulation tissue begins to develop. Further mesenchymal stem cells are recruited to the area and begin to differentiate (driven by BMPs) to fibroblasts, chondroblasts, and osteoblasts. As a result, chondrogenesis begins to occur, laying down a collagen-rich fibrocartilaginous network spanning the fracture ends, with a surrounding hyaline cartilage sleeve. At the same time, adjacent to the periosteal layers, a layer of woven bone is laid down by the osteoprogenitor cells.
Bony Callus Formation (Days 11 to 28)[edit]
The cartilaginous callus begins to undergo endochondral ossification. RANK-L is expressed, stimulating further differentiation of chondroblasts, chondroclasts, osteoblasts, and osteoclasts. As a result, the cartilaginous callus is resorbed and begins to calcify. Subperiosteally, woven bone continues to be laid down. The newly formed blood vessels continue to proliferate, allowing further migration of mesenchymal stem cells. At the end of this phase, a hard, calcified callus of immature bone forms.
Bone Remodelling (Day 18 onwards, lasting months-years)[edit]
With the continued migration of osteoblasts and osteoclasts, the hard callus undergoes repeated remodeling - termed 'coupled remodeling.' This 'coupled remodeling' is a balance of resorption by osteoclasts and new bone formation by osteoblasts. The center of the callus is ultimately replaced by compact bone, while the callus edges become replaced by lamellar bone. Substantial remodeling of the vasculature occurs alongside these changes. The process of bone remodeling lasts for many months, ultimately resulting in regeneration of the normal bone structure.
Factors affecting Fracture Healing[edit]
- Local factors
- Fracture characteristics - excessive movement, misalignment, extensive damage and soft tissues caught within fracture ends can lead to delayed or non-union
- Infection - it can lead to poor healing and delayed or non-union.
- Blood supply - reduced blood supply to the fracture site can lead to delayed or non-union.
- Systemic factors
(the presence of any of these factors predisposes to poor healing)
- Advanced age
- Obesity
- Anemia
- Endocrine conditions - Diabetes mellitus, Parathyroid disease, and Menopause
- Steroid administration
- Malnutrition
- Smoking
- There are multiple methods that the interprofessional team can utilize to promote/stimulate fracture healing, including:
- Dietary supplements - calcium, protein, Vitamins C, and D
- Bone stimulators - which can be electrical, electromagnetic, and ultrasound. The current effectiveness of these methods is still equivocal, and this area requires further research.
- Bone graft - this involves the use of bone to help provide a scaffold to the newly forming bone. This graft can be from the patient's body (autograft) or from a deceased donor (allograft).
| Fractures and cartilage damage | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
| Trauma | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian