Testicular cancer

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Testicular cancer | |
|---|---|
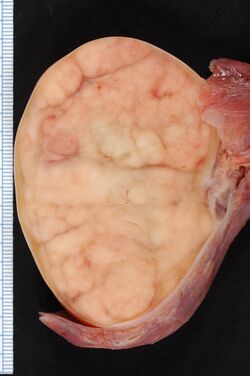 | |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Lump in the testicle, testicular pain, scrotal swelling |
| Complications | Infertility, metastasis |
| Onset | Most common in ages 15–35 |
| Duration | Varies |
| Types | Seminoma, non-seminomatous germ cell tumor |
| Causes | Unknown, risk factors include cryptorchidism, family history |
| Risks | Cryptorchidism, family history, Klinefelter syndrome |
| Diagnosis | Physical examination, ultrasound, tumor markers |
| Differential diagnosis | Epididymitis, hydrocele, spermatocele |
| Prevention | None specific, early detection |
| Treatment | Surgery, radiation therapy, chemotherapy |
| Medication | N/A |
| Prognosis | Generally good with treatment |
| Frequency | Rare, about 1 in 250 men |
| Deaths | Approximately 400 deaths per year in the US |
Testicular cancer is a disease in which malignant (cancer) cells form in the tissues of one or both testicles.Almost all testicular cancers start in the germ cells.
Testicular cancer is most common in young or middle-aged men. Most testicular cancers begin in germ cells (cells that make sperm) and are called testicular germ cell tumors.
Types[edit]
The two main types of testicular germ cell tumors are seminomas and nonseminomas. These 2 types grow and spread differently and are treated differently. Nonseminomas tend to grow and spread more quickly than seminomas. Seminomas are more sensitive to radiation. A testicular tumor that contains both seminoma and nonseminoma cells is treated as a nonseminoma. Testicular cancer is the most common cancer in men 20 to 35 years old.
Risk factors[edit]
Risk factors for testicular cancer include:
- Having had an undescended testicle.
- Having had abnormal development of the testicles.
- Having a personal history of testicular cancer.
- Having a family history of testicular cancer (especially in a father or brother).
- Being white.
Signs and symptoms[edit]
These and other signs and symptoms may be caused by testicular cancer or by other conditions. Check with your doctor if you have any of the following:
- A painless lump or swelling in either testicle.
- A change in how the testicle feels.
- A dull ache in the lower abdomen or the groin.
- A sudden build-up of fluid in the scrotum.
- Pain or discomfort in a testicle or in the scrotum.
Diagnosis[edit]
The following tests and procedures may be used: Physical exam and history: An exam of the body to check general signs of health, including checking for signs of disease, such as lumps or anything else that seems unusual. The testicles will be examined to check for lumps, swelling, or pain. A history of the patient's health habits and past illnesses and treatments will also be taken. Ultrasound exam of the testes: A procedure in which high-energy sound waves (ultrasound) are bounced off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram.
Serum tumor marker test:
A procedure in which a sample of blood is examined to measure the amounts of certain substances released into the blood by organs, tissues, or tumor cells in the body. Certain substances are linked to specific types of cancer when found in increased levels in the blood. These are called tumor markers. The following tumor markers are used to detect testicular cancer:
- Alpha-fetoprotein (AFP).
- Beta-human chorionic gonadotropin (β-hCG).
Tumor marker levels are measured before inguinal orchiectomy and biopsy, to help diagnose testicular cancer. Inguinal orchiectomy: A procedure to remove the entire testicle through an incision in the groin. A tissue sample from the testicle is then viewed under a microscope to check for cancer cells. (The surgeon does not cut through the scrotum into the testicle to remove a sample of tissue for biopsy, because if cancer is present, this procedure could cause it to spread into the scrotum and lymph nodes. It's important to choose a surgeon who has experience with this kind of surgery.) If cancer is found, the cell type (seminoma or nonseminoma) is determined in order to help plan treatment.
Treatment[edit]
There are different types of treatment for patients with testicular cancer. Testicular tumors are divided into 3 groups, based on how well the tumors are expected to respond to treatment. Good Prognosis For nonseminoma, all of the following must be true:
- The tumor is found only in the testicle or in the retroperitoneum (area outside or behind the abdominal wall); and
- The tumor has not spread to organs other than the lungs; and
- The levels of all the tumor markers are slightly above normal.
For seminoma, all of the following must be true:
- The tumor has not spread to organs other than the lungs; and
- The level of alpha-fetoprotein (AFP) is normal. Beta-human chorionic gonadotropin (β-hCG) and lactate dehydrogenase (LDH) may be at any level.
Intermediate prognosis For nonseminoma, all of the following must be true:
- The tumor is found in one testicle only or in the retroperitoneum (area outside or behind the abdominal wall); and
- The tumor has not spread to organs other than the lungs; and
- The level of any one of the tumor markers is more than slightly above normal.
For seminoma, all of the following must be true:
- The tumor has spread to organs other than the lungs; and
- The level of AFP is normal. β-hCG and LDH may be at any level.
Poor prognosis For nonseminoma, at least one of the following must be true:
- The tumor is in the center of the chest between the lungs; or
- The tumor has spread to organs other than the lungs; or
- The level of any one of the tumor markers is high.
- There is no poor prognosis grouping for seminoma testicular tumors.
Five types of standard treatment are used:
- Surgery
- Radiation therapy
- Chemotherapy
- Surveillance
- High-dose chemotherapy with stem cell transplant
Drugs Approved by FDA for Testicular Cancer
- Bleomycin Sulfate
- Cisplatin
- Cosmegen (Dactinomycin)
- Dactinomycin
- Etopophos (Etoposide Phosphate)
- Etoposide
- Etoposide Phosphate
- Ifex (Ifosfamide)
- Ifosfamide
- Vinblastine Sulfate
- Treatment for testicular cancer can cause infertility.
- Certain treatments for testicular cancer can cause infertility that may be permanent.
- Patients who may wish to have children should consider sperm banking before having treatment.
- Sperm banking is the process of freezing sperm and storing it for later use.
Prognosis[edit]
The prognosis (chance of recovery) and treatment options depend on the following:
- Stage of the cancer (whether it is in or near the testicle or has spread to other places in the body, and blood levels of AFP, β-hCG, and LDH).
- Type of cancer.
- Size of the tumor.
- Number and size of retroperitoneal lymph nodes.
Cure[edit]
- Testicular cancer can usually be cured in patients who receive adjuvant chemotherapy or radiation therapy after their primary treatment.
| * Tumors of the male urogenital system | ||||||
|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
Testicular cancer is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Testicular cancer
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian