Metachromatic leukodystrophy
| Metachromatic leukodystrophy | |
|---|---|
| Sulfatide.png | |
| Sulfatide | |
| Synonyms | Arylsulfatase A deficiency
|
| Symptoms | Progressive neurologic decline |
| Complications | Dementia |
| Usual onset | Infantile (1-2 years) or adulthood (around 40s)
|
| Types | Infantile or adulthood |
| Causes | Storage disease
|
| Diagnosis | Enzyme based and genetics
|
| Treatment | Palliative
|
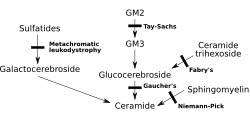
Metachromatic leukodystrophy (MLD) is categorized as a lysosomal storage disease and is commonly associated with both leukodystrophies and sphingolipidoses. This condition stems from anomalies in the metabolism of sphingolipids. Leukodystrophies, by definition, have an impact on the growth and development of myelin, a fatty substance that functions as insulation around nerve fibers across the central and peripheral nervous systems. A hallmark of MLD is the accumulation of cerebroside sulfate.
Inheritance[edit]
MLD predominantly follows an autosomal recessive inheritance pattern. This implies that both parents need to carry the defective gene for their offspring to manifest the disease.
Signs and Symptoms[edit]
MLD manifests in diverse forms which include late infantile, juvenile, and adult variations:
Late Infantile Form:
Represents 50-60% of MLD cases. Symptoms usually appear between 15-24 months after an initial normal development period. Key symptoms involve muscle weakness, rigidity, developmental delays, progressive vision loss, convulsions, swallowing difficulties, paralysis, dementia, and potential comatose states. Life expectancy is generally up to age 5 without treatment. Juvenile Form:
Onset usually between 3 and 10 years. Begins with impaired academic performance and mental decline. Symptoms evolve similarly to the late infantile form but progress slower. Life expectancy ranges from 10-15 years post-symptom onset, although some may live for multiple decades. Adult Form:
Onset post 16 years, typically in the 4th or 5th decade. Often manifests as a psychiatric disorder or progressive dementia. Generally exhibits a slower progression compared to the infantile and juvenile forms. Palliative care has been proven beneficial in symptom management and in enhancing the quality of life and longevity.
Causes[edit]
The direct culprit behind MLD is a deficiency in the enzyme arylsulfatase A (ARSA). Affected individuals exhibit significantly reduced enzyme activity in leukocytes. However, solely measuring ARSA enzyme activity doesn't confirm MLD diagnosis due to the existence of ARSA pseudodeficiency, which shows lower enzyme activity but doesn't result in MLD.
The absence of the necessary enzyme leads to the accumulation of sulfatides in various body tissues, which in turn destroys the protective myelin sheath of the nervous system. When this sheath deteriorates, the functioning of the central and peripheral nervous system, including motor functions, is severely impacted.
Additionally, ARSA requires activation by a non-enzymatic proteinaceous cofactor, saposin B (Sap B). In instances where ARSA levels are normal but sulfatides remain elevated, it suggests the enzyme isn't activated, leading to a condition similar to MLD called saposin B deficiency.
It's essential to highlight that the complete role of sulfatides in MLD is under investigation. Some studies suggest that lysosulfatide, a derivative of sulfatide, could contribute due to its cytotoxic properties.
Genetics[edit]
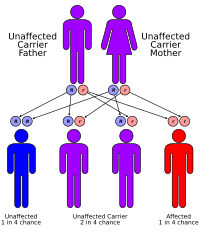
MLD inherits in an autosomal recessive manner, implying that both parents must carry the gene for the offspring to develop the disease. The inheritance probabilities per birth are as follows:
- If both parents are carriers:
- 25% (1 in 4) children will have the disease
- 50% (2 in 4) children will be carriers, but unaffected
- 25% (1 in 4) children will be free of MLD – unaffected child that is not a carrier
- If one parent is affected and one is free of MLD:
- 0% (0) children will have the disorder – only one parent is affected, other parent always gives normal gene
- 100% (4 in 4) children will be carriers (but unaffected)
- If one parent is a carrier and the other is free of MLD:
- 50% (2 in 4) children will be carriers (but unaffected)
- 50% (2 in 4) children will be free of MLD – unaffected child that is not a carrier
Diagnosis[edit]
Initial steps towards an MLD diagnosis often include a clinical examination and MRI. While MRI can suggest the possibility of MLD, it isn't conclusive.
Blood tests measuring ARSA-A enzyme levels paired with urinary sulfatide tests provide the best biochemical confirmation of MLD. Genomic sequencing can further reinforce the diagnosis, but considering the extensive range of known mutations, biochemical tests remain essential.
Treatment[edit]
Current therapeutic approaches for symptomatic late infantile MLD patients, as well as juvenile or adult MLD patients with advanced symptoms, center around symptom management, with no available cure.
However, for pre-symptomatic late infantile MLD patients and those with juvenile or adult forms showcasing mild symptoms, options like bone marrow transplantation (including stem cell transplantation) can be considered. These treatments primarily aim to slow the progression in the central nervous system.
Several experimental therapy options, such as gene therapy, enzyme replacement therapy (ERT), substrate reduction therapy (SRT), and enzyme enhancement therapy (EET), are undergoing clinical trials, mainly targeting late infantile patients.
| Lysosomal storage diseases: Inborn errors of lipid metabolism (Lipid storage disorders) | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Diseases of the nervous system, primarily CNS (G04–G47, 323–349) | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian