Hepatic encephalopathy

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Hepatic encephalopathy | |
|---|---|
| Micrograph showing Alzheimer type II astrocytes, as may be seen in hepatic encephalopathy. H&E stain. | |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Confusion, altered level of consciousness, coma |
| Complications | Cerebral edema, seizures |
| Onset | Gradual or sudden |
| Duration | Variable |
| Types | Type A, Type B, Type C |
| Causes | Liver failure, portosystemic shunt |
| Risks | Cirrhosis, hepatitis, alcoholic liver disease |
| Diagnosis | Clinical diagnosis, ammonia levels, EEG |
| Differential diagnosis | Wernicke's encephalopathy, metabolic encephalopathy, intracranial hemorrhage |
| Prevention | N/A |
| Treatment | Lactulose, rifaximin, dietary protein restriction |
| Medication | N/A |
| Prognosis | Variable, depends on underlying liver disease |
| Frequency | Common in patients with advanced liver disease |
| Deaths | N/A |
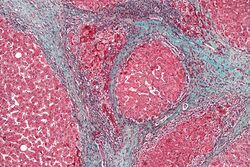
Other Names: Hepatoencephalopathy; Encephalopathy, hepatic Hepatic encephalopathy is a syndrome observed in some patients with cirrhosis. It is defined as a spectrum of neuropsychiatric abnormalities in patients with liver dysfunction, when other known brain disease has been excluded.
Cause[edit]
Although there are many theories and possibilities regarding what exactly causes hepatic encephalopathy, it is thought that one of the main causes is the accumulation of ammonia in the blood, which the liver, damaged by alcoholic liver disease, cannot remove. Researchers have found that ammonia alters the expression of certain genes; the genes that may be affected carry instructions for brain proteins. When the instructions in these genes are not "followed" correctly by the body due to the altered expression of the genes, the cells in the brain can no longer function normally, which may contribute to the signs and symptoms of the disease. However, the genes themselves are not changed in such a way that these changes are passed down to an individual's children.
Inheritance[edit]
Hepatic encephalopathy is not an inherited condition, so an individual who has it cannot pass it on to his/her children. It is brought on by chronic liver failure, particularly in alcoholics with cirrhosis.
Signs and symptoms[edit]
Signs and symptoms may be debilitating, and they can begin mildly and gradually, or occur suddenly and severely. They may include personality or mood changes, intellectual impairment, abnormal movements, a depressed level of consciousness, and other symptoms. The mildest form of hepatic encephalopathy is difficult to detect clinically, but may be demonstrated on neuropsychological testing. It is experienced as forgetfulness, mild confusion, and irritability. The first stage of hepatic encephalopathy is characterised by an inverted sleep-wake pattern (sleeping by day, being awake at night). The second stage is marked by lethargy and personality changes. The third stage is marked by worsened confusion. The fourth stage is marked by a progression to coma. More severe forms of hepatic encephalopathy lead to a worsening level of consciousness, from lethargy to somnolence and eventually coma. In the intermediate stages, a characteristic jerking movement of the limbs is observed (asterixis, "liver flap" due to its flapping character); this disappears as the somnolence worsens. There is disorientation and amnesia, and uninhibited behaviour may occur. In the third stage, neurological examination may reveal clonus and positive Babinski sign. Coma and seizures represent the most advanced stage; cerebral oedema (swelling of the brain tissue) leads to death. Encephalopathy often occurs together with other symptoms and signs of liver failure. These may include jaundice (yellow discolouration of the skin and the whites of the eyes), ascites (fluid accumulation in the abdominal cavity), and peripheral oedema (swelling of the legs due to fluid build-up in the skin). The tendon reflexes may be exaggerated, and the plantar reflex may be abnormal, namely extending rather than flexing (Babinski's sign) in severe encephalopathy. A particular smell on an affected person's breath (foetor hepaticus) may be detected.
Types[edit]
According to this classification, hepatic encephalopathy is subdivided in type A, B and C depending on the underlying cause.
- Type A (=acute) describes hepatic encephalopathy associated with acute liver failure, typically associated with cerebral oedema
- Type B (=bypass) is caused by portal-systemic shunting without associated intrinsic liver disease
- Type C (=cirrhosis) occurs in people with cirrhosis - this type is subdivided in episodic, persistent and minimal encephalopathy
Diagnosis[edit]
- The diagnosis of hepatic encephalopathy can only be made in the presence of confirmed liver disease (types A and C) or a portosystemic shunt (type B), as its symptoms are similar to those encountered in other encephalopathies. To make the distinction, abnormal liver function tests and/or ultrasound suggesting liver disease are required, and ideally a liver biopsy.
- The symptoms of hepatic encephalopathy may also arise from other conditions, such as bleeding in the brain and seizures (both of which are more common in chronic liver disease). A CT scan of the brain may be required to exclude bleeding in the brain, and if seizure activity is suspected an electroencephalograph (EEG) study may be performed.
- Serum ammonia levels are elevated in 90% of people, but not all hyperammonaemia (high ammonia levels in the blood) is associated with encephalopathy.
Treatment[edit]
- Those with severe encephalopathy (stages 3 and 4) are at risk of obstructing their airway due to decreased protective reflexes such as the gag reflex. This can lead to respiratory arrest. Transferring the person to a higher level of nursing care, such as an intensive care unit, is required and intubation of the airway is often necessary to prevent life-threatening complications (e.g., aspiration or respiratory failure).
- The treatment of hepatic encephalopathy depends on the suspected underlying cause (types A, B or C) and the presence or absence of underlying causes.
- If encephalopathy develops in acute liver failure (type A), even in a mild form (grade 1–2), it indicates that a liver transplant may be required, and transfer to a specialist centre is advised.
- Hepatic encephalopathy type B may arise in those who have undergone a TIPS procedure; in most cases this resolves spontaneously or with the medical treatments discussed below, but in a small proportion of about 5%, occlusion of the shunt is required to address the symptoms.
- In hepatic encephalopathy type C, the identification and treatment of alternative or underlying causes is central to the initial management.
- The medication(s) listed below have been approved by the Food and Drug Administration (FDA) as orphan products for treatment of this condition.
- Rifaximin (Brand name: Normix) Reduction in the risk of overt hepatic encephalopathy (HE) recurrence in patients greater than or equal to 18 years of age.
| Diseases of the nervous system, primarily CNS (G04–G47, 323–349) | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Diseases of the human digestive system | ||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
Hepatic encephalopathy is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Hepatic encephalopathy
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian