Kwashiorkor

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Kwashiorkor | |
|---|---|

| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Edema, irritability, anorexia, ulcerating dermatoses, enlarged liver |
| Complications | Infection, shock, coma |
| Onset | Typically after weaning |
| Duration | Variable, depending on treatment |
| Types | N/A |
| Causes | Protein deficiency |
| Risks | Malnutrition, poverty, famine |
| Diagnosis | Clinical diagnosis, blood test |
| Differential diagnosis | Marasmus, anemia, liver disease |
| Prevention | Adequate dietary protein intake |
| Treatment | Nutritional rehabilitation, dietary supplements |
| Medication | N/A |
| Prognosis | Good with treatment, poor without |
| Frequency | Common in areas of famine and poverty |
| Deaths | N/A |
Kwashiorkor is a severe form of malnutrition that primarily affects children living in regions where there is a shortage of quality food rich in protein.[1] The condition occurs when a child's diet lacks adequate sources of protein, even though the overall calorie intake may be sufficient. Kwashiorkor is more common in areas of drought and famine, where access to balanced meals is limited.
Etiology[edit]
Kwashiorkor is caused by inadequate protein intake, often coupled with other micronutrient deficiencies. This condition is most prevalent in regions of the world where there is a scarcity of high-protein food, such as regions experiencing famine or areas where the staple diet is high in carbohydrates and low in protein.[2]
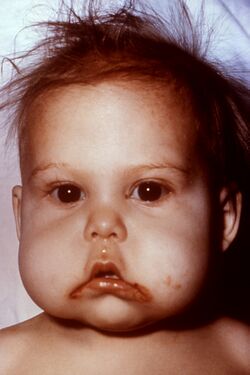
Clinical Presentation[edit]
Children with kwashiorkor typically exhibit swollen and distended bellies due to fluid retention (edema), a condition known as ascites. Other symptoms may include muscle wasting, skin and hair changes (like lighter hair color and flaky or rashy skin), lethargy, and a failure to grow or gain weight.[3]
Diagnosis[edit]
The diagnosis of kwashiorkor is primarily clinical, based on the presence of edema, growth failure, changes in skin and hair, and a history of inadequate protein intake. Laboratory tests may show low levels of serum proteins, particularly albumin, but these tests are not necessary for the diagnosis.[4]
Treatment[edit]
The management of kwashiorkor involves the gradual introduction of a balanced diet, starting with fluids and gradually introducing higher-protein foods. During the initial phase, care must be taken to avoid refeeding syndrome, a potentially fatal condition that can occur when malnourished individuals are fed too quickly.[5] Micronutrient supplements and medications may be used to treat any accompanying conditions or deficiencies.
Prognosis[edit]
With timely and appropriate treatment, the prognosis for children with kwashiorkor is generally good. However, some children may experience long-term complications, such as stunted growth and developmental delays, if treatment is not received promptly.[6]
Prevention[edit]
Prevention of kwashiorkor involves ensuring that children have access to a balanced diet that includes sufficient protein. This often requires efforts at a community or national level to address the underlying issues of food security and poverty. Education about the importance of a balanced diet can also play a significant role.[7]
See Also[edit]
References[edit]
- ↑ "Severe Malnutrition: Report of a Consultation to Review Current Literature".Public Health.2005;4(5)
- 1-16.doi:10.1186/1471-2458-5-8.
- ↑ "Protein Energy Malnutrition".Pediatrics in Review.2003;24(5)
- 154-162.doi:10.1542/pir.24-5-154.
- ↑ Vinay, Robbins Basic Pathology, Philadelphia, PA:Elsevier, 2018, ISBN 978-0-323-35317-5,
- ↑ "Protein energy malnutrition".Indian Journal of Medical Research.2015;141(3)
- 312-325.doi:10.4103/0971-5916.159576.
- ↑ "Guidelines for the inpatient treatment of severely malnourished children".Asia Pacific Journal of Clinical Nutrition.2005;14(2)
- 217-225.
- ↑ "Long-term follow-up showed improved growth status in young children with mild to moderate persistent malnutrition".Journal of Pediatric Gastroenterology and Nutrition.2014;58(1)
- 101-107.doi:10.1097/MPG.0b013e31829c800d.
- ↑ "Prevention and control of childhood malnutrition: the role of education of mothers".Child Care Health and Development.2006;32(5)
- 569-576.doi:10.1111/j.1365-2214.2006.00620.x.
| Malnutrition | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian