Triosephosphate isomerase deficiency
| Triosephosphate isomerase deficiency | |
|---|---|
| Autosomal recessive - en.svg | |
| Triosephosphate isomerase deficiency has an autosomal recessive pattern of inheritance. | |
| Synonyms | Triose phosphate-isomerase deficiency, TPI deficiency
|
| Specialty | Hematology, Neurology, Genetics |
| Symptoms | Hemolytic anemia, neuropathy, developmental delay, cardiomyopathy, recurrent infections |
| Complications | Respiratory failure, cardiac arrest, early death |
| Usual onset | Infancy or early childhood |
| Duration | Lifelong
|
| Causes | Mutations in the TPI1 gene |
| Risk factors | Family history of the condition |
| Diagnosis | Genetic testing, enzyme assay, blood smear, clinical presentation |
| Differential diagnosis | Pyruvate kinase deficiency, glucose-6-phosphate dehydrogenase deficiency, metabolic disorders |
| Prevention | Genetic counseling |
| Treatment | Supportive care |
| Medication | Transfusion, antibiotics, experimental enzyme replacement therapy |
| Prognosis | Poor (most cases fatal in early life) |
| Frequency | Extremely rare (<100 known cases worldwide) |
| Deaths | High mortality rate in early childhood |
Triosephosphate isomerase deficiency (TPI deficiency) is an extremely rare autosomal recessive disorder that affects glycolysis, the metabolic pathway responsible for breaking down glucose into energy. The condition results from mutations in the TPI1 gene, leading to deficiency of the triosephosphate isomerase enzyme. It is characterized by hemolytic anemia, severe neurological impairment, recurrent infections, and often early childhood death.
Pathophysiology[edit]
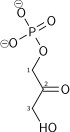
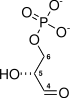
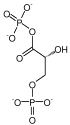
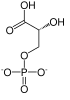
TPI deficiency is classified as a glycolytic enzymopathy, meaning it involves a deficiency of an enzyme in the glycolytic pathway. The triosephosphate isomerase enzyme catalyzes the reversible conversion of dihydroxyacetone phosphate (DHAP) and glyceraldehyde-3-phosphate (G3P), which are intermediates in glycolysis.
In individuals with TPI deficiency, the enzyme's activity is markedly reduced, leading to:
- Accumulation of DHAP
- Decreased cellular energy production
- Increased vulnerability of red blood cells to oxidative stress and premature destruction (hemolysis)
- Impaired neuromuscular and immune system function
Genetics[edit]
TPI deficiency is inherited in an autosomal recessive manner. Affected individuals inherit two defective copies of the TPI1 gene (located on chromosome 12p13). To date, at least thirteen mutations have been identified. These mutations result in either:
- Disrupted protein folding
- Impaired dimerization of the enzyme
- Accelerated degradation of the TPI protein
Carriers (heterozygotes) typically do not show clinical symptoms, even though they may have lower enzyme activity. It has been suggested that there may be a heterozygote advantage in some populations.
Clinical Presentation[edit]
Symptoms typically begin in infancy or early childhood and may include:
- Chronic hemolytic anemia
- Muscle weakness and hypotonia
- Developmental delay
- Seizures
- Recurrent infections due to immune deficiency
- Cardiomyopathy
- Respiratory failure
- Feeding difficulties
- Failure to thrive
The disease is progressive and often fatal during the first decade of life.
Diagnosis[edit]
Diagnosis is based on:
- Clinical signs of hemolytic anemia and neurological dysfunction
- Blood smear showing abnormal erythrocytes
- Enzyme assay showing low or absent TPI activity in red blood cells
- Genetic testing confirming mutations in TPI1
Differential Diagnosis[edit]
Conditions with overlapping symptoms may include:
- Pyruvate kinase deficiency
- Glucose-6-phosphate dehydrogenase deficiency
- Congenital metabolic disorders
- Neuromuscular diseases
Treatment[edit]
There is currently no cure for TPI deficiency. Management is supportive and may include:
- Blood transfusions for severe anemia
- Antibiotics for infections
- Physical therapy and supportive care
- Respiratory support as needed
- Experimental therapies such as enzyme replacement therapy or gene therapy are under investigation
Prognosis[edit]
Prognosis is generally poor. Many affected children die before the age of 5–10 years due to complications such as respiratory failure, severe anemia, or infections. However, disease severity can vary depending on the specific mutation(s) involved.
Epidemiology[edit]
TPI deficiency is exceptionally rare, with fewer than 100 documented cases worldwide. It affects both males and females and occurs in all ethnic groups.
See also[edit]
- Glycolysis
- Enzymopathy
- Hemolytic anemia
- Congenital metabolic disorder
- Autosomal recessive inheritance
External links[edit]
- OMIM entry on TPI deficiency
- NIH Genetic and Rare Diseases Information Center
- Genetic Testing Registry entry
NIH genetic and rare disease info[edit]
Triosephosphate isomerase deficiency is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Triosephosphate isomerase deficiency
|
| Diseases of red blood cells | ||||
|---|---|---|---|---|
|
| Inborn error of carbohydrate metabolism: monosaccharide metabolism disorders (E73–E74, 271) Including glycogen storage diseases (GSD) |
||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian