MPV17-related hepatocerebral mitochondrial DNA depletion syndrome
MPV17-related hepatocerebral mitochondrial DNA depletion syndrome is an inherited disorder that can cause liver disease and neurological problems. MPV17-related hepatocerebral mitochondrial DNA depletion syndrome is most frequently seen in the Navajo population of the southwestern United States. In this population, the condition is known as Navajo neurohepatopathy.
Epidemiology[edit]
MPV17-related hepatocerebral mitochondrial DNA depletion syndrome is thought to be a rare condition. Approximately 30 cases have been described in the scientific literature, including seven families with Navajo neurohepatopathy. Within the Navajo Nation of the southwestern United States, Navajo neurohepatopathy is estimated to occur in 1 in 1,600 newborns.
Cause[edit]
As the condition name suggests, mutations in the MPV17 gene cause MPV17-related hepatocerebral mitochondrial DNA depletion syndrome. The protein produced from the MPV17 gene is located in the inner membrane of cell structures called mitochondria. Mitochondria are involved in a wide variety of cellular activities, including energy production, chemical signaling, and regulation of cell growth, division, and death. Mitochondria contain their own DNA, known as mitochondrial DNA (mtDNA), which is essential for the normal function of these structures. It is likely that the MPV17 protein is involved in the maintenance of mtDNA. Having an adequate amount of mtDNA is essential for normal energy production within cells.
MPV17 gene mutations that cause MPV17-related hepatocerebral mitochondrial DNA depletion syndrome lead to production of a protein with impaired function. One mutation causes all cases of Navajo neurohepatopathy and results in the production of an unstable MPV17 protein that is quickly broken down. A dysfunctional or absent MPV17 protein leads to problems with the maintenance of mtDNA, which can cause a reduction in the amount of mtDNA (known as mitochondrial DNA depletion). Mitochondrial DNA depletion impairs mitochondrial function in many of the body's cells and tissues, particularly the brain, liver, and other tissues that have high energy requirements. Reduced mitochondrial function in the liver and brain lead to the liver failure and neurological dysfunction associated with MPV17-related hepatocerebral mitochondrial DNA depletion syndrome. Researchers suggest that the less mtDNA that is available in cells, the more severe the features of Navajo neurohepatopathy.
Inheritance[edit]
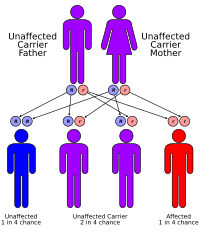
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Signs and symptoms[edit]
The signs and symptoms of this condition begin in infancy and typically include vomiting, diarrhea, and an inability to grow or gain weight at the expected rate (failure to thrive). Many affected infants have a buildup of a chemical called lactic acid in the body (lactic acidosis) and low blood sugar (hypoglycemia).
Within the first weeks of life, infants develop liver disease that quickly progresses to liver failure. The liver is frequently enlarged (hepatomegaly) and liver cells often have a reduced ability to release a digestive fluid called bile (cholestasis). Rarely, affected children develop liver cancer. After the onset of liver disease, many affected infants develop neurological problems, which can include developmental delay, weak muscle tone (hypotonia), and reduced sensation in the limbs (peripheral neuropathy). Individuals with MPV17-related hepatocerebral mitochondrial DNA depletion syndrome typically survive only into infancy or early childhood.
People with Navajo neurohepatopathy tend to have a longer life expectancy than those with MPV17-related hepatocerebral mitochondrial DNA depletion syndrome. In addition to the signs and symptoms described above, people with Navajo neurohepatopathy may have problems with sensing pain that can lead to painless bone fractures and self-mutilation of the fingers or toes. Individuals with Navajo neurohepatopathy may lack feeling in the clear front covering of the eye (corneal anesthesia), which can lead to open sores and scarring on the cornea, resulting in impaired vision. The cause of these additional features is unknown.
Diagnosis[edit]
MPV17-related mitochondrial DNA (mtDNA) maintenance defect should be suspected in individuals with the following clinical features, brain MRI findings, and supportive laboratory findings.
Clinical features
Hepatic
- Liver dysfunction or failure
- Cholestasis and steatosis
- Hepatomegaly
Neurologic
- Developmental delay
- Hypotonia
- Microcephaly
- Motor and sensory peripheral neuropathy
Gastrointestinal
- Gastrointestinal dysmotility
- Feeding difficulties
- Failure to thrive
Brain MRI findings
- White matter abnormalities
- Brain stem signal abnormalities
- Basal ganglia signal abnormalities
Supportive laboratory findings
- Serum testing
- Elevated hepatic transaminases and hyperbilirubinemia
- Lactic acidosis
- Hypoglycemia
- Liver histology
- Steatosis
- Cirrhosis
- Mitochondrial DNA analysis in liver and muscle
Mitochondrial DNA content:
- Is typically reduced in liver tissue (<20% of that found in tissue- and age-matched controls);
- Can also be reduced in muscle tissue (typically <30% of that found in tissue- and age-matched controls).
- Multiple mtDNA deletions have been occasionally described in muscle and liver.
Electron transport chain (ETC) assays in liver and muscle tissue of affected individuals typically show decreased activity of multiple complexes with complex I having reduced activity in 80% of affected individuals .
The diagnosis of MPV17-related mtDNA maintenance defect is established in a proband with biallelic pathogenic variants in MPV17 by molecular genetic testing. Differential Diagnosis Encephalohepatopathic form of MPV17-related mtDNA maintenance defect needs to be differentiated from other mtDNA maintenance defects that present with encephalohepatopathy.
Treatment[edit]
Ideally management is by a multidisciplinary team including specialists in hepatology, neurology, nutrition, clinical genetics, and child development. Nutritional support should be provided by a dietitian experienced in managing children with liver diseases; prevention of hypoglycemia requires frequent feeds and uncooked cornstarch (1-2 g/kg/dose). Although liver transplantation remains the only treatment option for liver failure, it is controversial because of the multisystem involvement in this disorder.
Prevention of secondary complications: Prevent nutritional deficiencies (e.g., of fat-soluble vitamins) by ensuring adequate intake.
Prognosis[edit]
MPV17-related encephalohepatopathy typically has a poor prognosis due to early liver failure. Liver transplantation has been performed in some affected individuals, with high rates of post-transplantation death.
| Diseases of the nervous system, primarily CNS (G04–G47, 323–349) | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
MPV17-related hepatocerebral mitochondrial DNA depletion syndrome is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - MPV17-related hepatocerebral mitochondrial DNA depletion syndrome
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian