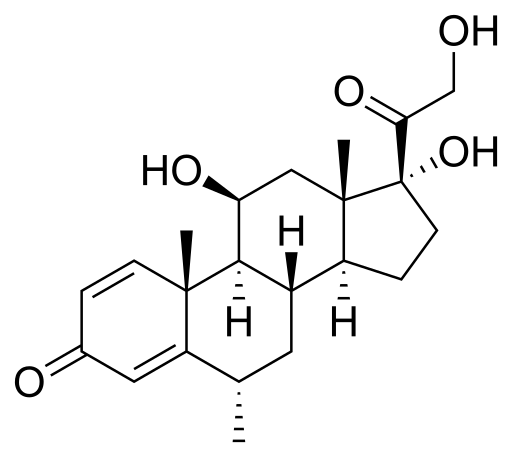
Methylprednisolone
Corticosteroid medication
| Methylprednisolone | |
|---|---|
|
| |
| Trade names | Medrol, Depo-Medrol, Solu-Medrol
|
| Routes | By mouth, intramuscular, intra-articular, intravenous
|
| Metabolism | Liver (CYP3A4) |
| Half-life | 1.8–2.6 hours |
| Excretion | Urine
|
| Identifiers | |
| CAS Number | 83-43-2 |
| PubChem | 6741 |
| DrugBank | DB00959
|
| ChEMBL | 650
|
Methylprednisolone is a synthetic glucocorticoid primarily used for its anti-inflammatory and immunosuppressive properties.
Methylprednisolone is on the World Health Organization’s List of Essential Medicines.
Medical Uses[edit]
Methylprednisolone is prescribed for a variety of conditions, including:
Inflammatory and Autoimmune Disorders
- Rheumatoid arthritis
- Systemic lupus erythematosus (SLE)
- Psoriatic arthritis
- Multiple sclerosis (MS)
- Ulcerative colitis
- Crohn’s disease
Allergic and Respiratory Conditions
- Severe allergies – including angioedema and anaphylaxis.
- Asthma and COPD exacerbations – Used as an oral or IV corticosteroid in severe cases.
Endocrine and Oncological Uses
- Adrenal insufficiency – As an alternative to hydrocortisone when mineralocorticoid activity is not required.
- Cancer therapy – Used in the management of leukemia, lymphoma, and multiple myeloma.
Neurological Disorders
- Multiple sclerosis (MS) relapses – Administered as high-dose IV methylprednisolone.
- Spinal cord injury (off-label) – Used to reduce inflammation in acute cases.
Ophthalmic Conditions
- Optic neuritis (often linked to MS)
- Uveitis, iritis, and scleritis
Administration and Dosage[edit]
Methylprednisolone is available in oral tablets, intramuscular, intra-articular, and intravenous formulations. Dosage depends on the condition being treated:
- Mild to moderate inflammation – 4–16 mg/day (oral)
- Severe inflammation or autoimmune flares – IV pulse therapy (e.g., 500–1000 mg IV)
- Acute asthma exacerbation – 40–80 mg/day PO or IV
Side Effects[edit]
Common Side Effects
- Weight gain
- Mood changes (insomnia, agitation)
- Increased blood sugar levels (hyperglycemia)
- Fluid retention
Serious Adverse Effects Long-term or high-dose use may lead to:
- Osteoporosis and fractures
- Adrenal suppression (requiring tapering)
- Glaucoma and cataracts
- Cushing’s syndrome (moon face, buffalo hump)
- Infections due to immune suppression
Pharmacology[edit]
Mechanism of Action Methylprednisolone is a glucocorticoid receptor agonist that: 1. Suppresses inflammation by inhibiting pro-inflammatory cytokines (IL-1, IL-6, TNF-alpha). 2. Suppresses the immune response by reducing T-cell activation. 3. Regulates metabolism by increasing glucose levels and altering fat distribution.
Metabolism and Elimination
- Metabolized in the liver (CYP3A4 pathway).
- Eliminated via the kidneys.
- Half-life: 1.8–2.6 hours.
Contraindications[edit]
Methylprednisolone should not be used in:
- Systemic fungal infections
- Uncontrolled infections
- Hypersensitivity to corticosteroids
- Live vaccine administration
Drug Interactions[edit]
- NSAIDs – Increased risk of gastric ulcers.
- Diabetes medications – May require higher insulin doses.
- Live vaccines – Risk of severe infection.
- Anticoagulants – May alter warfarin levels.
History[edit]
Methylprednisolone was first synthesized by The Upjohn Company (now Pfizer) and FDA-approved in 1957.
Availability[edit]
Methylprednisolone is available under multiple brand names:
- Medrol (oral tablets)
- Depo-Medrol (intramuscular injection)
- Solu-Medrol (intravenous formulation)
See Also[edit]
| Glucocorticoids and antiglucocorticoids (D07, H02) | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian