Diabesity
Diabesity is a neologism term coined to refer to the twin problems of obesity and diabetes which are often linked.
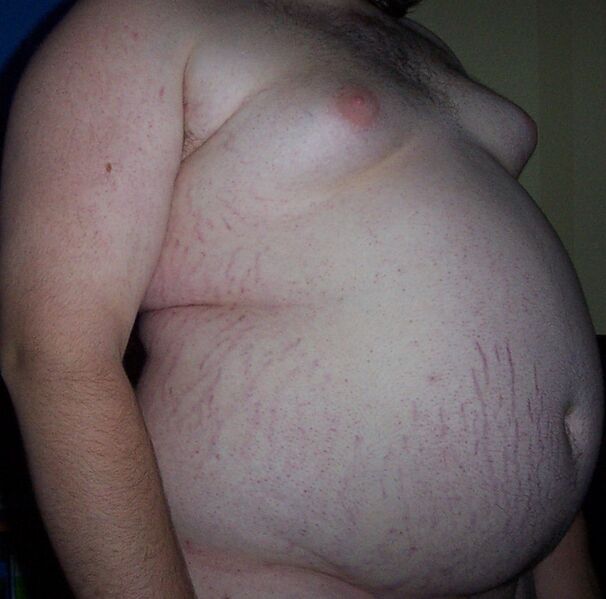
Obesity and diabetes[edit]
Obesity and diabetes are two of the most pressing public health concerns facing our world today. Both conditions are closely linked, with obesity being a major risk factor for the development of type 2 diabetes. In this article, we will explore the relationship between obesity and diabetes and discuss the potential mechanisms behind this association, as well as the potential implications for prevention and treatment.
Obesity[edit]
Obesity is defined as an excessive accumulation of body fat and is generally measured by body mass index (BMI).
Tye 2 diabetes[edit]
Type 2 diabetes is a chronic metabolic disorder characterized by high blood sugar levels and insulin resistance, which not only leads to prediabetes, metabolic syndrome and eventual diabetes but it can also feed back in to the loop of further weight gain as insulin controls hunger and more insulin due to IR means more hunger. The link between obesity and type 2 diabetes is well-established, with numerous studies showing that individuals who are obese are at a significantly increased risk of developing type 2 diabetes.
Link - insulin resistance[edit]
One of the main mechanisms behind the link between obesity and diabetes is insulin resistance. Insulin is a hormone that regulates blood sugar levels by facilitating the uptake of glucose into cells. In individuals who are obese, there is an accumulation of fat in the liver and muscle tissue, which leads to insulin resistance. As a result, the body's ability to properly regulate blood sugar levels is impaired, and over time this can lead to the development of type 2 diabetes.
Inflammation[edit]
Another mechanism that has been proposed to explain the link between obesity and diabetes is the release of inflammatory mediators. Adipose tissue, or fat tissue, is an active endocrine organ that releases various inflammatory mediators, known as cytokines, which can contribute to the development of insulin resistance (Hotamisligil, 2006). Furthermore, obesity can lead to an increase in the production of advanced glycation end products (AGEs) which can also play a role in inflammation and insulin resistance (Eudy, 2018). The Relationship between Diabetes and Obesity
Diabetes and Obesity: A Two-Way Relationship[edit]
Obesity and diabetes are not only connected, but they also interact in a vicious cycle. Obesity is a significant risk factor for type 2 diabetes, and once a person has diabetes, their risk of becoming obese increases. This is due to the fact that high blood glucose levels can cause insulin resistance, which can lead to weight gain and make it more difficult to control blood sugar levels (Centers for Disease Control and Prevention, 2021).
Type 2 diabetes is characterized by insulin resistance, which can be caused by obesity. When the body is insulin-resistant, the pancreas attempts to regulate blood sugar levels by producing more insulin. The pancreas can become exhausted over time, resulting in a decrease in insulin production and the development of type 2 diabetes (World Health Organization, 2020).
The Influence of Diabetes on Health[edit]
- Obesity can have a substantial effect on health, increasing the risk of a variety of chronic health problems. Among the most prevalent health issues associated with obesity are:
- Cardiovascular disease: Obese people are more likely to develop heart disease, stroke, and hypertension, which can increase the risk of heart attack and stroke (American Heart Association, 2021).
- Diabetic nephropathy High blood sugar can damage the kidneys, causing kidney disease and, in severe cases, kidney failure (National Kidney Foundation, 2021).
- Diabetes can cause neuropathy, resulting in numbness, tingling, and pain in the hands and feet (National Institute of Diabetes and Digestive and Kidney Diseases, 2021).
- Retinopathy: High blood sugar can damage the blood vessels in the eyes, resulting in vision loss or even blindness (American Academy of Ophthalmology, 2021).
- Diabetic neuropathy: Diabetic individuals are more likely to develop foot problems, such as foot ulcers and amputations (American Diabetes Association, 2021).
Preventing and Managing Diabesity[edit]
- Preventing and treating diabesity necessitates a multifaceted strategy that targets both obesity and diabetes. These are some of the most effective strategies:
- A diet low in processed foods, high in fiber, and abundant in fruits, vegetables, and whole grains can prevent weight gain and enhance insulin sensitivity (Harvard for Health, 2021).
- Regular physical activity can aid in preventing weight gain and enhancing insulin sensitivity. Most days of the week, aim for at least 30 minutes of moderate-intensity activity (American Heart Association, 2021).
- Maintaining a healthy weight is essential for preventing and treating diabetes. Even modest weight loss can improve insulin sensitivity and reduce the risk of developing type 2 diabetes if you are overweight or obese (Harvest for Health, 2021).
- Medications: Medications may be used, if necessary, to manage blood sugar levels and prevent the complications of diabetes (American Diabetes Association, 2021).
Losing weight is key[edit]
In terms of treatment, weight loss is a key component of managing diabetes in individuals who are obese. Losing weight can improve insulin sensitivity and lower blood sugar levels. This can be achieved through a combination of diet and exercise, and in some cases, medication and/or bariatric surgery may be necessary (Foster, 2015).
Rethinking Our Dietary ApproachShifting focus from individual blame to understanding the complexities of obesity is crucial. A key factor is insulin resistance, impacting up to 71% of the population, with 35% experiencing metabolic syndrome. Navigating Misinformation The overwhelming presence of over 20,000 books and mixed messages on obesity medicine calls for guidance from experts like Dr Prab R. Tumpati, MD, who can provide clarity on the science and practice of this field. The Downfall of the Food Guide Pyramid The outdated and ineffective food guide pyramid, promoting a low-fat but high-glycemic diet, significantly contributed to increased insulin resistance and, consequently, weight gain. |
The Blame Game in ObesityInsulin resistance and weight gain Insulin resistance is a physiological condition where the body's cells become less responsive to the hormone insulin. As insulin not only controls the blood sugar, it also controls the weight! Reducing the overall carbohydrate load and insulin levels is a key underlying concept in many low carbohydrate diets such as the ketogenic diet. Understanding metabolic starvation Weight gain isn't typically intentional. It often stems from the paradox of metabolic starvation in the obese, driven by insulin resistance and resulting in heightened insulin levels. This leads to persistent hunger, cravings, and further weight gain. Stop blaming the victim for obesity! |
Summary[edit]
In conclusion, the link between obesity and type 2 diabetes is well-established, with numerous studies showing that individuals who are obese are at a significantly increased risk of developing type 2 diabetes. The potential mechanisms behind this association include insulin resistance and the release of inflammatory mediators. In order to prevent the development of type 2 diabetes and improve the management of diabetes in individuals who are obese, it is important to focus on strategies to reduce obesity, such as promoting healthy eating and regular physical activity.
References[edit]
- Eudy, A.M. (2018) Advanced Glycation End Products and Diabetes. Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy. 11: 1–8.
- Foster, G.D. (2015) Clinical management of obesity. American Journal of Clinical Nutrition. 102 (Suppl 3): 781S–787S.
- Hotamisligil, G.S. (2006) Inflammation and metabolic disorders. Nature. 444: 860–867.
- Knowler, W.C. (2002) Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. New England Journal of Medicine. 346 (6): 393–403.
| Diabetes | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
| Obesity | ||
|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian