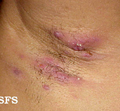
Hidradenitis suppurativa
| Hidradenitis suppurativa | |
|---|---|
| Hidradenitis suppurativa (stage II) in axilla.jpg | |
| Hidradenitis suppurativa (stage II) in the left armpit | |
| Synonyms | Acne inversa, acne conglobata, apocrine acne, Verneuil's disease, Velpeau’s disease
|
| Specialty | Dermatology |
| Symptoms | Multiple inflamed and swollen skin lesions
|
| Usual onset | Young adulthood |
| Duration | Long-term |
| Types | Stage I, II, III |
| Causes | Unknown
|
| Diagnosis | Based on symptoms |
| Differential diagnosis | Acne, acne conglobata, pilonidal cysts
|
| Treatment | Warm baths, laser therapy, surgery |
| Medication | Antibiotics, immunosuppressive medication
|
| Frequency | 1–4% of people |
| Deaths | Rare |
Hidradenitis suppurativa (HS), alternatively known as acne inversa, is a chronic skin disease manifested by recurrent inflamed lesions and nodules. These lesions are frequently painful and prone to rupture, releasing fluid or pus. Scar tissue often forms after the lesions heal. Due to its physical manifestations, HS can have significant psychosocial impacts, including self-consciousness and depression.
Presentation and Affected Areas[edit]
HS typically manifests in areas of the body where skin rubs together, like the axillary (underarm) regions, inframammary (under the breasts) areas, and the groin. Lesions may also develop around the anal and genital areas. The skin condition evolves from small, pimple-like bumps to hard, painful nodules that can persist for weeks or months.
Etiology[edit]
The precise etiology of HS remains uncertain, but it's thought to arise from a combination of genetic predispositions and environmental triggers. Approximately one-third of HS patients have a family history of the disease. Modifiable risk factors, such as obesity and smoking, are also associated with HS. The condition is not infectious, and it does not result from poor hygiene or deodorant use.
The pathogenesis is believed to involve either apocrine sweat gland dysfunction or hair follicle abnormalities, leading to follicular occlusion and secondary bacterial infection and inflammation.
Diagnosis[edit]
Diagnosis of HS is primarily clinical, based on characteristic patient history and physical examination. The recurrent nature of the painful, pus-filled nodules in the characteristic body areas strongly points to this condition.
Treatment[edit]
Management of HS focuses on reducing flare-ups, relieving symptoms, and preventing disease progression. It often involves a combination of lifestyle modifications, medications, and in severe cases, surgical intervention.
References[edit]
See also[edit]
-
Hidradenitis suppurativa
-
Hidradenitis suppurativa growths
-
Hidradenitis suppurativa on abdomen
-
Hidradenitis suppurativa
-
Micrograph of hidradenitis suppurativa
-
Hidradenitis suppurativa lesions
-
Hidradenitis suppurativa on leg
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian