Kidney
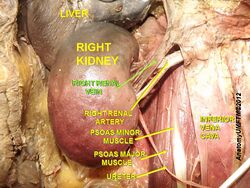
The kidneys are paired, bean-shaped organs in the vertebrate urinary system responsible for filtering blood and excreting waste products and excess fluids in the form of urine. They play a central role in homeostasis, including regulating electrolyte balance, blood pressure, and acid-base balance. The study of the kidneys is known as nephrology (from Greek nephros meaning "kidney"), while the term renal (from Latin renes) is the adjective often used in medical contexts.
Anatomy and Location[edit]
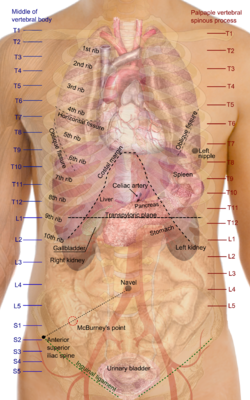
In humans, the kidneys are located in the posterior portion of the abdominal cavity, one on each side of the vertebral column. They lie between vertebral levels T12 and L3 and are considered retroperitoneal, meaning they are located behind the peritoneum. The right kidney typically lies slightly lower than the left to accommodate the overlying liver. Each kidney is topped by an adrenal gland.
The kidneys are partially protected by the 11th and 12th pairs of ribs and are cushioned by a double layer of fat: perirenal and pararenal fat. Rare anatomical variations such as a third kidney may occur.
Structure[edit]
Each adult kidney is approximately 11 cm long and 5 cm thick, weighing about 150 grams. The kidney has a concave medial border with an opening called the renal hilum, where the renal artery, renal vein, ureter, and nerves enter and exit.
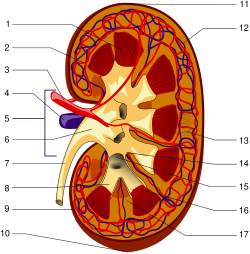
Gross anatomy[edit]
- Renal capsule – A tough fibrous layer surrounding the kidney
- Renal cortex – The outer layer containing glomeruli and blood vessels
- Renal medulla – The inner region organized into cone-shaped renal pyramids
- Renal pelvis – Funnel-shaped structure collecting urine from calyces
- Ureter – Tube carrying urine to the bladder
- Calyces – Chambers that collect urine from the pyramids
- Papilla – Tip of each renal pyramid that empties into a calyx
Blood Supply[edit]
The kidneys receive about 20–25% of the cardiac output through the renal artery, a direct branch of the abdominal aorta. The renal artery branches into:
- Interlobar arteries → Arcuate arteries → Interlobular (cortical radial) arteries
- Afferent arterioles → Glomerulus → Efferent arterioles
- Peritubular capillaries and vasa recta
Filtered blood exits through the renal vein into the inferior vena cava.
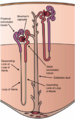
Nephron[edit]
Each kidney contains over a million nephrons – the microscopic functional units. Each nephron consists of:
- Glomerulus – site of filtration
- Bowman's capsule
- Proximal convoluted tubule
- Loop of Henle
- Distal convoluted tubule
- Collecting duct system
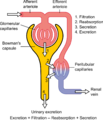
Processes:
- Filtration of blood plasma
- Reabsorption of vital substances (e.g., glucose, Na⁺)
- Secretion of waste (e.g., H⁺, drugs)
- Excretion as urine
Collecting Duct System[edit]
The collecting ducts transport urine through the renal medulla to the renal pelvis. Antidiuretic hormone (ADH) regulates water permeability:
- ↑ADH = concentrated urine
- ↓ADH = dilute urine
Deficiency or resistance to ADH can result in diabetes insipidus.
Physiological Functions[edit]
The kidneys filter roughly 180 liters of blood daily, forming 1.5–2 liters of urine. Functions include:
Waste Excretion[edit]
Removal of nitrogenous waste:
Electrolyte and Fluid Balance[edit]
Regulation of:
- Sodium (Na⁺)
- Potassium (K⁺)
- Calcium (Ca²⁺)
- Phosphate
- Water balance
Acid-Base Balance[edit]
Maintenance of blood pH (~7.4) by:
- H⁺ excretion
- HCO₃⁻ reabsorption
Main transporters:
Blood Pressure Regulation[edit]
Via the Renin–angiotensin–aldosterone system (RAAS):
- ↓Blood pressure → ↑Renin → ↑Angiotensin II → ↑Aldosterone → Na⁺ retention → ↑Blood volume → ↑Blood pressure
Hormone Secretion[edit]
- Erythropoietin – stimulates red blood cell production
- Renin – blood pressure regulation
- Calcitriol – active vitamin D for calcium homeostasis
Medical Terminology[edit]
- Nephro- (Greek) and Renal- (Latin) denote kidney-related terms
- Nephrectomy = surgical removal of a kidney
- Radical nephrectomy = removal of the kidney with surrounding structures
Diseases and Disorders[edit]
Congenital[edit]
- Polycystic kidney disease
- Horseshoe kidney
- Renal dysplasia
- Congenital hydronephrosis
- Duplicated ureter
Acquired[edit]
- Glomerulonephritis
- Nephrotic syndrome
- Pyelonephritis
- Diabetic nephropathy
- Kidney stones
- Renal cell carcinoma
- Lupus nephritis
- Minimal change disease
- Renal failure (acute or chronic)
Chronic Kidney Disease (CKD) Staging[edit]
CKD is staged by glomerular filtration rate (GFR):
- Stage 1: Normal GFR (>90), kidney damage
- Stage 2: GFR 60–89
- Stage 3: GFR 30–59, moderate dysfunction
- Stage 4: GFR 15–29, severe damage
- Stage 5: GFR <15, End-stage renal disease (ESRD), requires dialysis or transplant
Dialysis and Transplantation[edit]
- Dialysis removes waste via machine (hemodialysis) or abdominal lining (peritoneal dialysis)
- Kidney transplantation offers a curative option
- First successful transplant: 1954, Boston
- Types: Living donor and Deceased donor
- Immunosuppressive therapy is required post-transplant
Gallery[edit]
-
Posterior view of the left kidney
-
Schematic of a kidney nephron
-
Diagram showing nephron function
-
Mechanism of secretion and reabsorption in nephrons
-
Diagram of peritoneal dialysis setup
See Also[edit]
- Urology
- Nephrology
- Urinary system
- Kidney development
- Endocrine system
- Kidney transplantation
- Glomerular filtration rate
| Urinary system - Kidney - edit |
|---|
| Renal capsule | Renal cortex | Renal medulla (Renal sinus, Renal pyramids) | Renal calyx | Renal pelvis |
| Nephron - Renal corpuscle (Glomerulus, Bowman's capsule) → Proximal tubule → Loop of Henle → Distal convoluted tubule → Collecting ducts
Juxtaglomerular apparatus (Macula densa, Juxtaglomerular cells) Renal circulation - Renal artery → Interlobar arteries → Arcuate arteries → Cortical radial arteries → Afferent arterioles → Glomerulus → Efferent arterioles → Vasa recta → Arcuate vein → Renal vein |
| Renal physiology |
| Filtration - Ultrafiltration | Countercurrent exchange
Hormones effecting filtration - Antidiuretic hormone (ADH) | Aldosterone | Atrial natriuretic peptide Endocrine - Renin | Erythropoietin (EPO) | Calcitriol (Active vitamin D) | Prostaglandins |
| Assessing Renal function / Measures of Dialysis |
| Glomerular filtration rate | Creatinine clearance | Renal clearance ratio | Urea reduction ratio | Kt/V | Standardized Kt/V | Hemodialysis product |
| Anatomy of the urinary system | ||||||||
|---|---|---|---|---|---|---|---|---|
|
| Diseases of the endocrine system (E00–E35, 240–259) | ||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian