Sickle cell disease

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Sickle cell disease | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Anemia, pain crisis, swelling in hands and feet, infections, delayed growth |
| Complications | Stroke, acute chest syndrome, organ damage, pulmonary hypertension |
| Onset | Usually in infancy |
| Duration | Chronic |
| Types | N/A |
| Causes | Genetic mutation in the HBB gene |
| Risks | Family history, African, Mediterranean, Middle Eastern, Indian ancestry |
| Diagnosis | Blood test, genetic testing |
| Differential diagnosis | N/A |
| Prevention | N/A |
| Treatment | Pain management, blood transfusions, hydroxyurea, bone marrow transplant |
| Medication | N/A |
| Prognosis | Variable, improved with treatment |
| Frequency | Common in certain populations |
| Deaths | N/A |
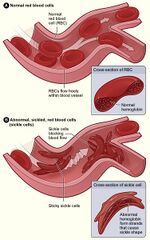
SCD is a hereditary genetic illness in which defective red blood cells transport less oxygen from the lungs to the rest of the body. These aberrant red blood cells aggregate in the blood arteries, causing discomfort, infections, and organ damage.

Cause[edit]
A mutation in the HBB gene, which encodes the beta-globin portion of hemoglobin, causes sickle cell disease. This mutation produces an aberrant form of hemoglobin known as hemoglobin S, which causes red blood cells to become sickle-shaped and less flexible. A person must inherit two copies of the defective gene from each parent in order to develop sickle cell disease.
Symptoms[edit]
Primary sickle cell disease symptoms include:
- Anemia is a deficiency in red blood cells that can result in fatigue and shortness of breath.
- Pain crises: Episodes of extreme agony lasting from hours to days caused by sickle-shaped cells obstructing blood flow in small capillaries.
- High vulnerability to infections as a result of spleen dysfunction.
- Decreased blood supply to organs can result in long-term organ damage, affecting the kidneys, liver, and lungs.
Complications[edit]
Many consequences can result from sickle cell disease, including:
- Acute chest syndrome is a potentially fatal illness marked by chest discomfort, fever, and breathing trouble.
- Stroke is the interruption of blood flow to the brain, which can result in permanent neurological damage.
- Leg ulcers are painful, sluggishly-healing wounds on the legs.
- Visual impairment caused by damage to the blood vessels in the eye, resulting in retinal detachment or other eye issues.
- Gallstones are stones that form in the gallbladder as a result of increased bilirubin production.
Diagnosis[edit]
Blood tests, such as a complete blood count (CBC) and hemoglobin electrophoresis, can detect the presence of aberrant hemoglobin during sickle cell disease diagnosis. In addition to confirming the diagnosis, genetic testing can help identify disease carriers.
Treatment[edit]
Currently, there is no cure for sickle cell disease, although therapies are available to help control symptoms and prevent complications. They consist of:
- Pain treatment medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids, can assist in the management of pain crises.
- Frequent transfusions of blood can minimize anemia and the risk of complications.
- A drug that can minimize the frequency of pain crises and acute chest syndrome is hydroxyurea.
- A potentially curative treatment involving the replacement of the patient's bone marrow with healthy donor bone marrow. Yet, this operation has substantial risks and is not appropriate for many individuals.
Summary[edit]
Sickle cell disease is an inherited disease in which the body makes abnormal red blood cells that carry less oxygen from the lungs to the rest of the body. These abnormal red blood cells form clumps that get stuck in the blood vessels, causing pain, infections, and organ damage.
| Diseases of red blood cells | ||||
|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian