Obstetrics

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC



Obstetrics originates from the Latin term obstare, which translates to "to stand by". This surgical specialty is dedicated to the management and care of a woman throughout her pregnancy, childbirth, and the puerperium phase, which refers to the immediate period following birth. A notable fact is that a significant portion of obstetricians also specialize in gynaecology, leading to the combined discipline of Obstetrics and gynaecology.
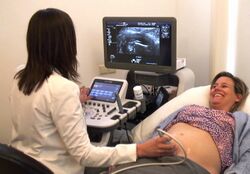
Introduction to Obstetrics[edit]
Obstetrics plays a critical role in ensuring the health and safety of both the mother and her child during the pre-natal and post-natal periods. By continuously monitoring the health and progress of the pregnancy, obstetricians can detect and manage potential complications.
Antenatal Care[edit]
Antenatal care, in the context of obstetrics, encompasses the medical attention and interventions provided to a pregnant woman. The primary aim of these interventions is to track the progress of her pregnancy and to ensure both the mother and fetus remain in optimal health.
Routine Check-ups[edit]
Upon confirming a pregnancy, the obstetrician will schedule regular appointments with the expecting woman to observe the progress of her pregnancy. These visits can differ in frequency based on the availability of medical resources and the presence of risk factors, such as diabetes.
Surveillance and Detection[edit]
Regular antenatal visits provide an opportunity for the early detection and management of potential complications. Some of the complications routinely screened for include:
Pre-eclampsia: This condition is identified by consistently monitoring the blood pressure and examining the urine of a pregnant woman. Placenta praevia: An ultrasound can visualize the placenta, particularly if it obstructs the birth canal. Abnormal Presentation: Late in pregnancy, the fetus might adopt an unconventional position, such as feet-first or buttocks-first (breech), side-on (transverse), or even at an unusual angle (oblique presentation). IUGR (Intrauterine Growth Restriction): IUGR denotes situations where fetal growth is below the 10th percentile for the gestational age. The underlying causes can either be intrinsic to the fetus or external, commonly arising from placental issues.
Signs and Symptoms by Trimester[edit]
Throughout the course of pregnancy, a woman's body undergoes significant changes, leading to a variety of symptoms. These symptoms are typically classified based on the trimester in which they appear.
First Trimester[edit]
Elevated levels of β-hCG (up to 100,000 mIU/mL by 10 weeks GA) can result in morning sickness, fatigue, mood swings, and specific food cravings. These symptoms typically persist until the 12th to 16th week of gestation.
Second Trimester[edit]
The growing fetus leads to an evident abdominal protrusion starting from the pelvis. Signs such as hyperpigmentation and the appearance of the linea nigra are common.
Third Trimester[edit]
The increasing weight of the fetus can induce backaches. The spine's curvature often adapts during pregnancy to counterbalance the shift in weight distribution. Women may experience mild urinary incontinence due to the pressure exerted on the bladder by the enlarging uterus. Heartburn is frequent, resulting from the compression of the stomach.
Overall Pregnancy Signs[edit]
Throughout pregnancy, women may observe several signs and symptoms, including:
- Bluish discoloration of the vagina and cervix (Chadwick's sign).
- Softening and cyanosis of the cervix after 4 weeks (Goodell's sign).
- Uterus softening post 6 weeks (Ladin's sign).
- Enlargement and sensitivity of the breasts.
- Linea nigra extending from the umbilicus to the pubis.
- Visible telangiectasias.
- Palmar erythema.
- Absence of menstruation (Amenorrhea).
- Frequent nausea and vomiting.
- Breast pain.
- Detection of fetal movement.
Pain due to the compression of the sciatic nerve (Sciatica).
Complications[edit]
See Complications of pregnancy
Fetal assessments[edit]
- Common
- ultrasound is used for many functions:
- Dating the gestational age of a pregnancy, most accurate in first trimester
- Detecting fetal anomalies in the second trimester
- biophysical profiles (BPP)
- Blood flow velocity in umbilical cord -- decrease/absence/reversal or diastolic blood flow in the umbilical artery is worrisome.
- Congenital anomalies can be diagnosed with second trimester ultrasound
- Fetal karyotype for the screening of genetic diseases can be obtained via amniocentesis or chorionic villus sampling (CVS)
- Uncommon
- Fetal hematocrit for the assessment of fetal anemia, Rh isoimmunization, or hydrops can be determined by percutaneous umbilical blood sampling (PUBS) which is done by placing a needle through the abdomen into the uterus and taking a portion of the umbilical cord.
- Fetal lung maturity is associated with how much surfactant the fetus is producing. Reduced production of surfactant indicates decreased lung maturity and is a high risk factor for neonatal respiratory distress syndrome (NRDS). Typically a lecithin:sphingomyelin ratio greater than 1.5 is associated with increased lung maturity.
- Nonstress test (NST) for fetal heart rate
- Oxytocin challenge test
Induction[edit]
An obstetrician may recommend a woman have her labour induced if it is felt that continuation would be more dangerous to her, the fetus, or both. Reasons to induce include:
- pre-eclampsia
- IUGR
- diabetes
- other general medical condition, such as renal disease
Induction may occur any time after 24 weeks of gestation if the risk to the fetus or mother is greater than the risk of delivering a premature fetus regardless of lung maturity. Prior to 32 weeks gestation steroids are given to the mother to help mature the fetus's lungs.
If a woman does not eventually labour by 41-42 weeks, induction may be performed, as the placenta may become unstable after this date.
Induction is achieved by 3 methods:
- pessary of Prostin cream, prostaglandin E2
- surgical induction, by piercing the amnion
- infusion of oxytocin
Labour[edit]
During labour itself, the obstetrician may be called on to do a number of things:
- monitor the progress of labour, by reviewing the nursing chart, performing vaginal examination, and assessing the trace produced by a foetal monitoring device (the cardiotocograph)
- accelerate the progress of labour by infusion of the hormone oxytocin
- provide pain relief, either by nitrous oxide (nowadays uncommon, at least in the U.S.), opiates, or by epidural anesthesia done by anaethestists or an anesthesiologist
- surgically assisting labour, by forceps or the Ventouse (a suction cap applied to the fetus' head)
- Caesarean section, if vaginal delivery is decided against or appears too difficult. Caesarean section can either be elective, that is, arranged before labour, or decided during labour as an alternative to hours of waiting. True "emergency" Cesarean sections (where minutes count) are a rarity.
- In the U.S., obstetric routine often includes a circumcision of the newborn. US circumcision stats. This procedure removes the foreskin of the male. In the UK this procedure is considered medically unnecessary so it is no longer recommended. In Australia this procedure is not performed unless specifically requested by the parents and the surgeon consents.
Emergencies in obstetrics[edit]
Two main emergencies are ectopic pregnancy and (pre)eclampsia.
- Ectopic pregnancy is when an embryo implants in the Fallopian tube or (rarely) on the ovary or inside the peritoneal cavity. This may cause massive internal bleeding.
- Pre-eclampsia is a disease caused by mysterious toxins secreted by the placenta. These toxins act on the vascular endothelium, causing hypertension and proteinuria. If severe, it progresses to fulminant pre-eclampsia, with headaches and visual disturbances. This is a prelude to eclampsia, where a convulsion occurs, which is often fatal.
Imaging, monitoring and care[edit]
In present society, medical science has developed a number of procedures to monitor pregnancy.
Antenatal record[edit]
On the first visit to her obstetrician or midwife, the pregnant woman is asked to carry out the antenatal record, which constitutes a medical history and physical examination.
On subsequent visits, the gestational age (GA) is rechecked with each visit. Symphysis-fundal height (SFH; in cm) should equal gestational age after 20 weeks of gestation, and the fetal growth should be plotted on a curve during the antenatal visits. The fetus is palpated by the midwife or obstetrician using Leopold maneuver to determine the position of the baby. Blood pressure should also be monitored, and may be up to 140/90 in normal pregnancies. High blood pressure indicates hypertension and possibly pre-eclampsia, if severe swelling (edema) and spilled protein in the urine are also present.
Fetal screening is also used to help assess the viability of the fetus, as well as congenital problems. Genetic counseling is often offered for families who may be at an increased risk to have a child with a genetic condition. Amniocentesis at around the 20th week is sometimes done for women 35 or older to check for Down's Syndrome and other chromosome abnormalities in the fetus. Even earlier than amniocentesis is performed, the mother may undergo the triple test, nuchal screening, nasal bone, alpha-fetoprotein screening and Chorionic villus sampling, also to check for disorders such as Down Syndrome. Amniocentesis is a prenatal genetic screening of the fetus, which involves inserting a needle through the mother's abdominal wall and uterine wall, to extract fetal DNA from the amniotic fluid. There is a risk of miscarriage and fetal injury with amniocentesis since it involves penetrating the uterus with the baby still in utero.
Imaging[edit]
Imaging is another important way to monitor a pregnancy. The mother and fetus are also usually imaged in the first trimester of pregnancy. This is done to predict problems with the mother; confirm that a pregnancy is present inside the uterus; guess the gestational age; determine the number of fetuses and placentae; evaluate for an ectopic pregnancy and first trimester bleeding; and assess for early signs of anomalies.
X-rays and computerized tomography (CT) are not used, especially in the first trimester, due to the ionizing radiation, which has teratogenic effects on the fetus. Instead, ultrasound is the imaging method of choice in the first trimester and throughout the pregnancy, since it emits no radiation, is portable, and allows for realtime imaging. Ultrasound imaging may be done at any time throughout the pregnancy, but usually happens at the 12th week (dating scan) and the 20th week (detailed scan).
A normal gestation would reveal a gestational sac, yolk sac, and fetal pole. The gestational age can be assessed by evaluating the mean gestation sac diameter (MGD) before week 6, and the crown-rump length after week 6. Multiple gestation is evaluated by the number of placentae and amniotic sacs present.
Pregnancy has different cultural aspects related to the perception of the body, the relationship with partner and to the meaning of the event.
Terms and definitions[edit]
- embryo - conceptus between time of fertilization to 10 weeks of gestation
- fetus - from 10 weeks of gestation to time of birth
- infant - time of birth to 1 year of age
- gestational age - time from last menstrual period (LMP) up to present
- first trimester - up to 14 weeks of gestation
- second trimester - 14 to 28 weeks of gestation
- third trimester - 28 weeks to delivery
- viability - minimum age for fetus survival, ca. third trimester
- previable infant - delivered prior to 24 weeks
- preterm infant - delivered between 24-37 weeks
- term infant - delivered between 37-42 weeks
- gravidity (G) - number of times a woman has been pregnant
- parity (P) - number of pregnancies with a birth beyond 20 weeks GA or an infant weighing more than 500 g
- Ga Pw-x-y-z - a = number of pregnancies, w = number of term births, x = number of preterm births, y = number of miscarriages, z = number of living children; for example, G4P1-2-1-3 means the woman had a total of 4 pregnancies, of which 1 is of term, 2 are preterm, 1 miscarriage, and 3 total living children (1 term + 2 preterm).
External links[edit]
- Childbirth from Embryo to Fetus video clip 2 min.
- Childbirth- Final Stage of Labor video clip 2 min.
- Obstetrics Forums
- Ingenious: archive of historical images related to obstetrics, gynaecology, and contraception.
See also[edit]
| Pregnancy and childbirth | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
| Sexual and reproductive health | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
| Symptoms and signs in obstetrics | ||||
|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian