Isoniazid
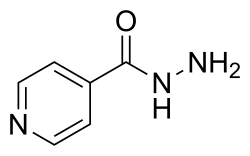
Isoniazid (often abbreviated as INH) is an antibiotic primarily used for the treatment and prevention of tuberculosis (TB). Since its discovery in the early 1950s, it has become a cornerstone drug in first-line anti-tuberculosis regimens worldwide. Its mechanism of action involves inhibiting the synthesis of mycolic acids, which are essential components of the bacterial cell wall of Mycobacterium tuberculosis.
Overview[edit]
Isoniazid is an essential medicine on the World Health Organization's List of Essential Medicines, emphasizing its significance in global health. It is often prescribed in combination with other anti-tuberculosis drugs to enhance efficacy and prevent the emergence of drug-resistant TB strains.
Pharmacology[edit]
- Mechanism of Action: Isoniazid is a prodrug and, once activated by the bacterial catalase enzyme KatG, inhibits the synthesis of mycolic acids in Mycobacterium tuberculosis. This leads to impaired cell wall synthesis and bacterial cell death.
- Metabolism: It is primarily metabolized in the liver via acetylation. Genetic factors determine the rate of acetylation, with individuals being classified as slow or fast acetylators.
- Excretion: The drug is primarily excreted in urine.
Indications[edit]
- Treatment of active tuberculosis, often in combination with other drugs like rifampicin, pyrazinamide, and ethambutol.
- Prophylactic treatment in individuals who have been exposed to active TB cases, especially in close contacts.
- Latent TB infections.
Contraindications[edit]
Isoniazid is contraindicated in individuals:
- With acute liver disease or a history of drug-induced hepatitis.
- With severe hypersensitivity reactions to the drug.
Side Effects[edit]
Like all drugs, isoniazid is associated with a range of side effects:
- Hepatotoxicity: It can cause drug-induced liver injury, ranging from asymptomatic increases in liver enzymes to acute liver failure.
- Peripheral neuropathy: This may manifest as tingling or numbness in the extremities.
- Gastrointestinal symptoms: Including nausea, vomiting, and abdominal discomfort.
- Rash.
- Fever.
- Hematological disorders: Such as anemia, thrombocytopenia, or leukopenia.
- CNS effects: Including seizures, psychosis, or dizziness.
Drug Interactions[edit]
- Isoniazid may increase blood levels of phenytoin, leading to phenytoin toxicity.
- Concurrent use with alcohol increases the risk of hepatotoxicity.
- Antacids can reduce the absorption of isoniazid if taken simultaneously.
Prophylaxis and Management[edit]
To reduce the risk of peripheral neuropathy, pyridoxine (vitamin B6) supplementation is recommended, especially in pregnant women, breastfeeding mothers, malnourished individuals, and those with diabetes or HIV.
Resistance[edit]
Resistance to isoniazid is a growing concern, especially in regions with high TB burden. It is usually due to mutations in the katG gene or inhA promoter of the bacterium.
See Also[edit]
| Antimycobacterials, including tuberculosis treatment and leprostatic agents (J04) | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Monoamine metabolism modulators | ||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| GABA metabolism and transport modulators | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Hydrazines |
|---|
|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian