Anticholinergic
- An anticholinergic refers to a substance or medication that blocks the effects of acetylcholine, a neurotransmitter involved in the cholinergic signaling pathway.
- Anticholinergics inhibit the activity of acetylcholine at cholinergic receptors, thereby modulating various physiological processes in the body.
- Anticholinergics binds to and blocks nicotinic and/or muscarinic receptors, thereby preventing the actions of the neurotransmitter acetylcholine (Ach) at these receptors.
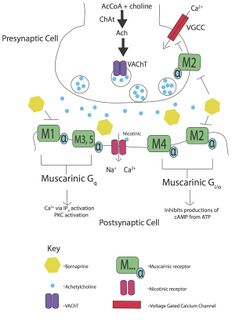
Mechanism of Action[edit]
Anticholinergics exert their effects by binding to and blocking the activation of cholinergic receptors.
These receptors are found throughout the body and are classified into two main types:
- Muscarinic Receptors: These receptors are located in various organs, including the heart, smooth muscles, and glands. Anticholinergics that target muscarinic receptors are referred to as muscarinic antagonists.
- Nicotinic Receptors: Nicotinic receptors are found in the central nervous system, autonomic ganglia, and neuromuscular junctions. Anticholinergics that block nicotinic receptors are called nicotinic antagonists.
- By inhibiting the binding of acetylcholine to these receptors, anticholinergics disrupt the transmission of nerve impulses in cholinergic pathways.
Effects of Anticholinergics[edit]
The blockade of cholinergic receptors by anticholinergics can result in various physiological and pharmacological effects, including:
- Decreased Secretions: Anticholinergics can reduce the production of saliva, tears, sweat, and other secretions by inhibiting the activation of cholinergic receptors in the glands.
- Smooth Muscle Relaxation: Anticholinergics cause relaxation of smooth muscles in the airways, [[gastrointestinal tract], and bladder. This effect can help alleviate symptoms of conditions such as asthma, irritable bowel syndrome, or overactive bladder.
- Increased Heart Rate: In certain situations, anticholinergics can lead to an increase in heart rate by blocking the inhibitory effects of acetylcholine on the heart's pacemaker cells.
- Cognitive and Central Nervous System Effects: Anticholinergics can have central nervous system effects, including sedation, confusion, and memory impairment. These effects are more likely to occur with anticholinergics that can penetrate the blood-brain barrier.
Uses of Anticholinergics[edit]
Anticholinergics find applications in various medical fields:
- Gastrointestinal Disorders: Anticholinergics can be used to relieve symptoms of gastrointestinal conditions such as irritable bowel syndrome, peptic ulcers, and gastrointestinal spasms.
- Respiratory Disorders: In the treatment of respiratory conditions like asthma and chronic obstructive pulmonary disease (COPD), anticholinergics can be used as bronchodilators to help relax the airway smooth muscles and improve airflow.
- Eye Conditions: Anticholinergic eye drops are sometimes prescribed to dilate the pupils (mydriasis) for ophthalmic examinations or to treat certain eye conditions, such as uveitis or iritis.
- Urinary Disorders: Anticholinergics can be used to alleviate symptoms of overactive bladder, such as frequent urination, urgency, and urinary incontinence.
Examples of Anticholinergics[edit]
Some examples of anticholinergic medications include:
- Atropine: Atropine is a classic anticholinergic medication used for various purposes, such as dilating the pupils, reducing salivary and respiratory secretions, and treating certain cardiac conditions.
- Scopolamine: Scopolamine is commonly used to prevent motion sickness and treat nausea and vomiting.
- Tiotropium: Tiotropium is an inhaled anticholinergic medication used in the treatment of chronic obstructive pulmonary disease (COPD) to improve airflow.
- Oxybutynin: Oxybutynin is used to alleviate symptoms of overactive bladder, including urinary frequency, urgency, and incontinence.
- These are just a few examples of the many anticholinergic medications available, each with its specific uses and considerations.
Adverse Effects[edit]
The use of anticholinergics may be associated with certain adverse effects, which can include:
- Dry Mouth and Eyes: Decreased secretions can result in dry mouth and dry eyes, leading to discomfort and increased risk of dental caries or eye irritation.
- Blurred Vision: Anticholinergics can cause temporary blurred vision due to pupillary dilation and reduced ability to focus on nearby objects.
- Constipation: Anticholinergics may slow down bowel movements, leading to constipation.
- Urinary Retention: In some cases, anticholinergics can impair bladder emptying and lead to urinary retention.
- Central Nervous System Effects: Certain anticholinergics can cross the blood-brain barrier and cause central nervous system side effects, such as drowsiness, confusion, dizziness, or memory problems.
Contraindications and Precautions[edit]
There are certain situations in which the use of anticholinergics may be contraindicated or require caution.
These include:
- Glaucoma: Anticholinergics should be used with caution in individuals with narrow-angle glaucoma as they can increase intraocular pressure.
- Urinary Retention: Anticholinergics are generally contraindicated in individuals with urinary retention, as they can exacerbate the condition.
- Gastrointestinal Obstruction: Anticholinergics should be avoided in individuals with gastrointestinal obstruction, as they can further impair gastrointestinal motility.
- Prostate Enlargement: Anticholinergics may worsen urinary symptoms in individuals with prostate enlargement (benign prostatic hyperplasia).
- Cardiovascular Conditions: Some anticholinergics may have cardiac effects and should be used cautiously in individuals with certain cardiovascular conditions, such as arrhythmias or heart failure.
Drug Interactions[edit]
- Anticholinergics may interact with other medications, leading to potential effects or changes in their pharmacological actions.
- It is important to consider possible drug interactions when prescribing or using anticholinergics, especially in combination with the following:
- Antidepressants: Anticholinergics can enhance the anticholinergic effects of certain antidepressant medications, potentially increasing the risk of adverse effects.
- Antihistamines: Concurrent use of antihistamines and anticholinergics can lead to additive anticholinergic effects, resulting in increased side effects such as sedation and dryness.
- Antipsychotics: Some antipsychotic medications have inherent anticholinergic properties. Combining them with anticholinergics can potentiate anticholinergic effects and increase the risk of side effects.
- Other Medications: It is important to consider potential interactions with specific medications, such as certain antiparkinsonian drugs, antispasmodics, or medications used to treat urinary incontinence.
See Also[edit]
- Cholinergic
- Acetylcholine
- Muscarinic antagonist
- Nicotinic antagonist
- Anticholinesterase
- Antimuscarinic
- Parasympatholytic
|
This article is a stub You can help WikiMD by registering and expanding it with useful details, internal links, formatting, and categories. Editing is available only to registered and verified users. WikiMD is a comprehensive, free health and wellness encyclopedia. |
| Pharmacomodulation | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Acetylcholine metabolism and transport modulators | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian
