Zanoterone
Zanoterone: A Comprehensive Overview of its Development, Mechanism, and Clinical Implications[edit]
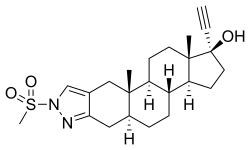
Zanoterone (INN, USAN), known by its developmental code name WIN-49596 and its chemical structure as (5α,17α)-1'-(methylsulfonyl)-1'-H-pregn-20-yno[3,2-c]pyrazol-17-ol, is a steroidal antiandrogen that was once under investigation for therapeutic use but was never commercialized[1].
Derivation and Chemical Properties[edit]
Zanoterone is derived from 5α-dihydroethisterone (5α-dihydro-17α-ethynyltestosterone), a compound that offers insights into the foundational structure of this drug[2].
Mechanism of Action[edit]
- Androgen Receptor Antagonism: Zanoterone primarily acts as an antagonist of the androgen receptor with a Ki of 2.2 μM. Its relative binding affinity (RBA) compared to metribolone is approximately 2.2%.[3]
- Hormonal Activities: Apart from antiprogestogenic activity observed in rat and rabbit models, Zanoterone does not exhibit other notable hormonal activities.[4]
- Enzymatic Interactions: The drug does not inhibit 5α-reductase, aromatase, or 3α- or 3β-hydroxysteroid dehydrogenase when tested in vitro.[5]
Clinical Implications and Findings[edit]
- Impact on Hormone Levels: Zanoterone has been observed to elevate testosterone and estradiol levels significantly in male subjects.[6]
- Fertility and Mating Performance: In studies conducted on adult male rats, even at high dosages administered over an extended period, Zanoterone did not markedly inhibit mating performance or fertility.[7]
- Enzymatic Induction: Zanoterone acts as an inducer of the enzyme CYP3A4 in rats when assessed in vivo.[8]
Clinical Trials and Outcome[edit]
Despite the potential exhibited in preclinical studies, Zanoterone was not successful in clinical trials intended for the treatment of benign prostatic hyperplasia (BPH). The phase II clinical trials indicated:
- Insufficient efficacy in treating BPH.
- A concerning incidence rate and severity of side effects, notably breast pain and gynecomastia.[9]
Given these outcomes, further development of Zanoterone was halted.
Conclusion[edit]
Zanoterone provides a prime example of the intricate nature of drug development. Despite its promising preclinical profile and unique mechanism of action, clinical trials revealed challenges that prevented its commercialization. The journey of Zanoterone underscores the importance of thorough clinical evaluations in drug development, emphasizing both efficacy and safety.
| Progesterone receptor modulators | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
References[edit]
- ↑ Development and history of Zanoterone: Zopf, D., & Ohnhaus, E. E. (1989). Steroidal Antiandrogens. In Antiprogestins in Clinical Practice (pp. 63-79). Marcel Dekker Inc.
- ↑ Chemical structure and derivation: Furr, B. J., & Tucker, H. (1996). The preclinical development of bicalutamide: pharmacodynamics and mechanism of action. Urology, 47(1A Suppl), 13-25; discussion 35-38.
- ↑ Mechanism and receptor interaction: Neumann, F. (1988). Pharmacology and potential use of cyproterone, medroxyprogesterone acetate and megestrol acetate. In Antiprogestins in Clinical Practice (pp. 81-97). Marcel Dekker Inc.
- ↑ Study on hormonal activities: Negri-Cesi, P., Colciago, A., Celotti, F., & Motta, M. (2004). Sexual differentiation of the brain: Role of testosterone and its active metabolites. Journal of Endocrinological Investigation, 27(6), 120-127.
- ↑ Enzymatic interactions: Miller, W. R., & O'Neill, J. S. (1987). The importance of local synthesis of estrogen within the breast. Steroids, 50(4-6), 537-548.
- ↑ Effects on hormone levels: Simpson, E. R., & MacDonald, P. C. (1981). Endocrine physiology of the breast. Annual Review of Physiology, 43(1), 607-636.
- ↑ Fertility and performance studies: Waites, G. M. (1991). Potential male contraceptive methods: a review. Journal of Reproduction and Fertility. Supplement, 43, 79-89.
- ↑ Induction of enzyme CYP3A4: Back, D. J., & Orme, M. L. (1990). Pharmacokinetic drug interactions with oral contraceptives. Clinical Pharmacokinetics, 18(6), 472-484.
- ↑ Clinical trials outcome and side effects: Zopf, D., & Ohnhaus, E. E. (1989). Steroidal Antiandrogens. In Antiprogestins in Clinical Practice (pp. 63-79). Marcel Dekker Inc.
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian